The intricate lining of our digestive tract, a crucial barrier protecting our bodies from harmful substances, is surprisingly vulnerable. Recent scientific exploration is shedding light on how everyday consumables, from common over-the-counter medications to dietary staples, can compromise this vital intestinal barrier, leading to a condition colloquially known as "leaky gut." This heightened intestinal permeability, characterized by an impaired barrier function, is emerging as a significant factor in both the prevention and treatment of a growing list of diseases, prompting a reevaluation of our dietary and medicinal habits.
The intestinal barrier, a marvel of biological engineering, is not a simple tube but a complex, folded structure spanning an astonishing 4,000 square feet—larger than a tennis court. Maintaining this expansive surface area requires a substantial commitment from the body, consuming approximately 40% of its total energy expenditure. This immense energy investment underscores the critical role the intestinal barrier plays in overall health, acting as the first line of defense against pathogens and toxins while facilitating nutrient absorption.
The Growing Evidence of Intestinal Permeability’s Role in Disease
A robust and expanding body of research suggests that disruptions to this intestinal barrier integrity are intrinsically linked to the pathogenesis of various health conditions. Notably, celiac disease and inflammatory bowel diseases (IBD), such as Crohn’s disease and ulcerative colitis, have demonstrated a strong correlation with compromised intestinal permeability. These conditions, characterized by chronic inflammation and digestive distress, are increasingly viewed through the lens of a damaged gut barrier allowing for the inappropriate passage of substances into the bloodstream, triggering immune responses and perpetuating inflammation.
Researchers have employed innovative methods to visualize and measure intestinal permeability. One such technique involves the use of a harmless blue food coloring. In individuals with healthy intestinal barriers, this coloring agent remains confined within the digestive tract. However, in critically ill patients suffering from sepsis, a life-threatening systemic inflammatory response, the same coloring agent has been detected in the bloodstream. This stark contrast highlights the profound impact of severe illness on gut barrier function.
However, the development of a "leaky gut" is not confined to intensive care units or extreme medical conditions. Even common, readily available medications can initiate this process. The widespread use of nonsteroidal anti-inflammatory drugs (NSAIDs), such as aspirin and ibuprofen, has been identified as a significant contributor to increased intestinal permeability.
NSAIDs and the Erosion of Gut Health
Studies have provided concrete data on the impact of NSAIDs on the intestinal barrier. For instance, a single dose of two standard 325 mg aspirin tablets, or even two extra-strength 500 mg tablets, has been shown to measurably increase gut leakiness. This finding is particularly concerning for the general population, suggesting that even healthy individuals who occasionally use aspirin for common ailments could be inadvertently compromising their gastrointestinal health. The potential for even short-term use to induce gastrointestinal barrier dysfunction warrants a cautious approach to NSAID consumption.
The notion that buffered aspirin, formulated with antacids to ostensibly mitigate gastrointestinal irritation, might offer protection has been challenged by scientific inquiry. Research indicates that buffered aspirin, such as Bufferin, does not significantly alter the damaging effects of aspirin. In fact, studies utilizing endoscopic examinations have revealed that both regular aspirin and buffered formulations can cause multiple erosions and significant redness within the inner lining of the stomach and intestine. Astonishingly, these detrimental effects can manifest within a remarkably short timeframe, with visible damage occurring as quickly as five minutes after administration at recommended doses. This rapid onset of damage underscores the inherent sensitivity of the gastrointestinal lining to these medications.
In contrast to aspirin, acetaminophen, widely known as Tylenol in the United States, appears to present a lower risk of direct gastrointestinal damage. However, it is crucial to note that acetaminophen is primarily metabolized by the liver, and individuals with pre-existing liver conditions should exercise extreme caution or avoid its use altogether. Interestingly, some dietary supplements, such as vitamin C, have been observed to potentially exacerbate aspirin-induced gut leakiness, suggesting a complex interplay between ingested substances and gut barrier function.
The implications of NSAID-induced gut leakiness extend beyond simple digestive discomfort. Emerging research suggests a significant link between NSAID use and food-induced anaphylaxis, a severe and potentially life-threatening allergic reaction. It is estimated that NSAIDs are implicated in up to 25% of food-induced anaphylaxis cases. This association is hypothesized to stem from the increased intestinal permeability caused by these drugs. When the gut barrier is compromised, undigested food particles, which would normally be broken down and absorbed, can "leak" into the bloodstream. This passage of larger food molecules can trigger an exaggerated immune response, leading to severe allergic reactions, including anaphylaxis. The 10-fold higher odds of these life-threatening events in individuals taking NSAIDs highlight the critical need for awareness regarding this potential side effect.
Beyond Medications: Lifestyle Factors and Gut Health
The impact of lifestyle choices on intestinal permeability is also a subject of intense scientific scrutiny. Even strenuous physical activity, while generally beneficial for overall health, can temporarily affect gut barrier integrity. An hour of exercise at 70% of maximum capacity, for instance, can divert significant blood flow away from internal organs, including the intestines, towards working muscles. This transient reduction in blood supply can induce mild injury to the intestinal lining, leading to a temporary increase in gut leakiness. This effect can be further exacerbated if athletes consume NSAIDs, a practice that remains unfortunately common in sports medicine.

Alcohol consumption has also been identified as a contributing factor to increased gut leakiness, sharing a similar mechanism with NSAIDs in potentially increasing the risk of food allergy attacks. The proposed pathway involves alcohol’s impact on the intestinal barrier, allowing for greater passage of substances into the bloodstream. Conversely, abstaining from alcohol may offer a pathway for the gut to heal and restore its barrier function.
Dietary Habits and the Gut Microbiome
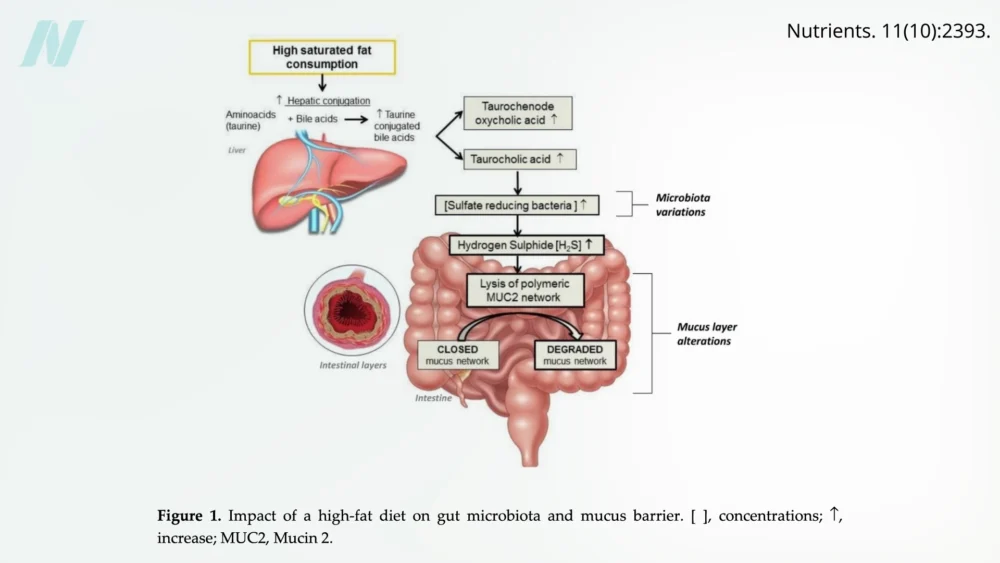
Dietary patterns play a pivotal role in maintaining a healthy intestinal environment. Elevated consumption of saturated fats, commonly found in red meat, dairy products, and processed "junk" foods, has been linked to detrimental changes in the gut. Saturated fats can promote the growth of specific types of gut bacteria that produce hydrogen sulfide, a gas with a distinct rotten-egg odor. This gas can degrade the protective mucus layer that lines the intestinal wall, further compromising the barrier’s integrity.
The broader impact of high-fat diets on intestinal health has been a significant area of research. While many studies have been conducted on laboratory animals or in vitro settings, the findings consistently point towards a negative influence on the intestinal barrier system through various mechanisms. The increasing global prevalence of obesity and cardiometabolic disorders, coinciding with a widespread shift from traditional lower-fat diets to higher-fat Westernized diets, provides a compelling epidemiological context for these findings.
A disturbance in the delicate balance of gut flora, the trillions of microorganisms residing in the digestive tract, has been strongly associated with an elevated risk of many of these chronic diseases. Rodent studies have suggested that high-fat diets can unbalance the gut microbiome and impair the gut barrier, ultimately contributing to disease development.
To bridge the gap between animal studies and human health, a randomized controlled feeding trial was conducted to specifically investigate the effects of dietary fat on the gut microbiota and barrier function in humans. This six-month trial revealed that higher fat consumption was indeed associated with unfavorable alterations in the gut microbiome and increased levels of proinflammatory factors in the blood. Notably, this study demonstrated that even replacing refined carbohydrates with refined fats, such as swapping white rice and wheat flour for soybean oil, could induce these negative changes. These findings have significant implications for public health recommendations, suggesting that countries undergoing dietary transitions towards Westernized patterns should counsel against increasing dietary fat intake, while those already consuming high-fat diets should consider strategies for reduction.
Understanding and Addressing Leaky Gut
The concept of intestinal permeability as a therapeutic target is gaining traction within the medical community. While the exact mechanisms by which various factors contribute to gut leakiness are complex and multifaceted, the evidence is mounting that addressing this issue could be key to preventing and managing a range of chronic conditions.
Implications for Public Health and Future Research
The widespread influence of common medications and dietary choices on intestinal health necessitates a public health dialogue focused on informed consumption. Greater awareness of the potential for NSAIDs to compromise gut integrity, particularly for individuals with pre-existing digestive issues or those at risk of food allergies, is crucial. Similarly, the growing body of evidence linking high-fat diets to gut dysbiosis and barrier dysfunction underscores the importance of promoting balanced, nutrient-rich eating patterns.
Future research will likely focus on developing more precise diagnostic tools to identify and quantify intestinal permeability in clinical settings. Furthermore, continued investigation into the specific mechanisms by which different foods and substances impact the gut barrier will pave the way for targeted therapeutic interventions. The potential for dietary modifications and lifestyle changes to not only alleviate symptoms but also to prevent the onset and progression of chronic diseases is a promising frontier in modern medicine.
As scientific understanding evolves, the "leaky gut" is moving from a fringe concept to a recognized factor in a spectrum of health challenges. By understanding the triggers and embracing strategies to fortify our intestinal barrier, individuals can take proactive steps towards safeguarding their long-term health and well-being.
Doctor’s Notes and Further Resources:
For those seeking to delve deeper into the intricacies of leaky gut syndrome and its relationship with inflammation and dietary interventions, further resources are available:
- The Leaky Gut Theory of Why Animal Products Cause Inflammation: This resource explores the potential mechanisms by which animal-derived products might contribute to intestinal inflammation and barrier dysfunction.
- How to Heal a Leaky Gut with Diet: This provides practical, evidence-based dietary strategies aimed at restoring and maintaining a healthy intestinal barrier.
- Friday Favorites: Tests, Fiber, and Low FODMAP for Small Intestinal Bacterial Overgrowth (SIBO): While focused on SIBO, this discussion may touch upon gut permeability as a related factor in digestive health and the role of dietary fiber and specific dietary approaches.






