A groundbreaking examination of surgical efficacy, employing the controversial yet revealing methodology of sham surgery trials, has cast a stark light on some of the most widely adopted medical interventions. The findings suggest that a significant number of these procedures, long considered standard practice, may offer little to no genuine therapeutic benefit, raising profound questions about patient care, medical industry influence, and the very definition of medical progress.
The Rise and Fall of the Intragastric Balloon: A Cautionary Tale
One of the most striking examples of this phenomenon centers on intragastric balloons, devices that first entered the medical landscape with considerable fanfare in the 1980s. Marketed as a less invasive alternative for weight management, these balloons were designed to be inserted into the stomach and inflated, ostensibly to induce satiety by occupying a significant portion of the stomach’s volume. The initial promise was substantial: a non-surgical method to aid individuals struggling with obesity.
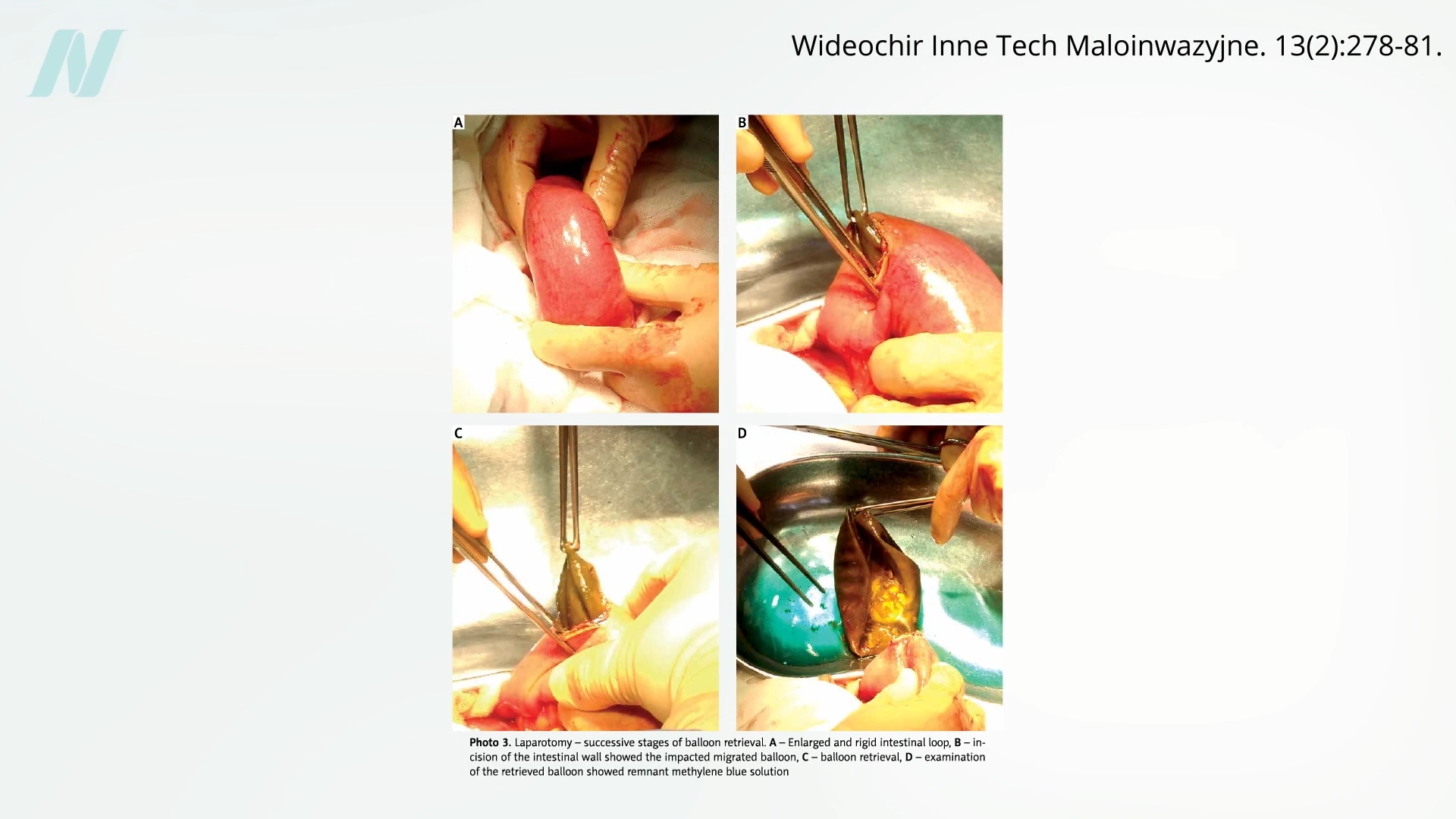
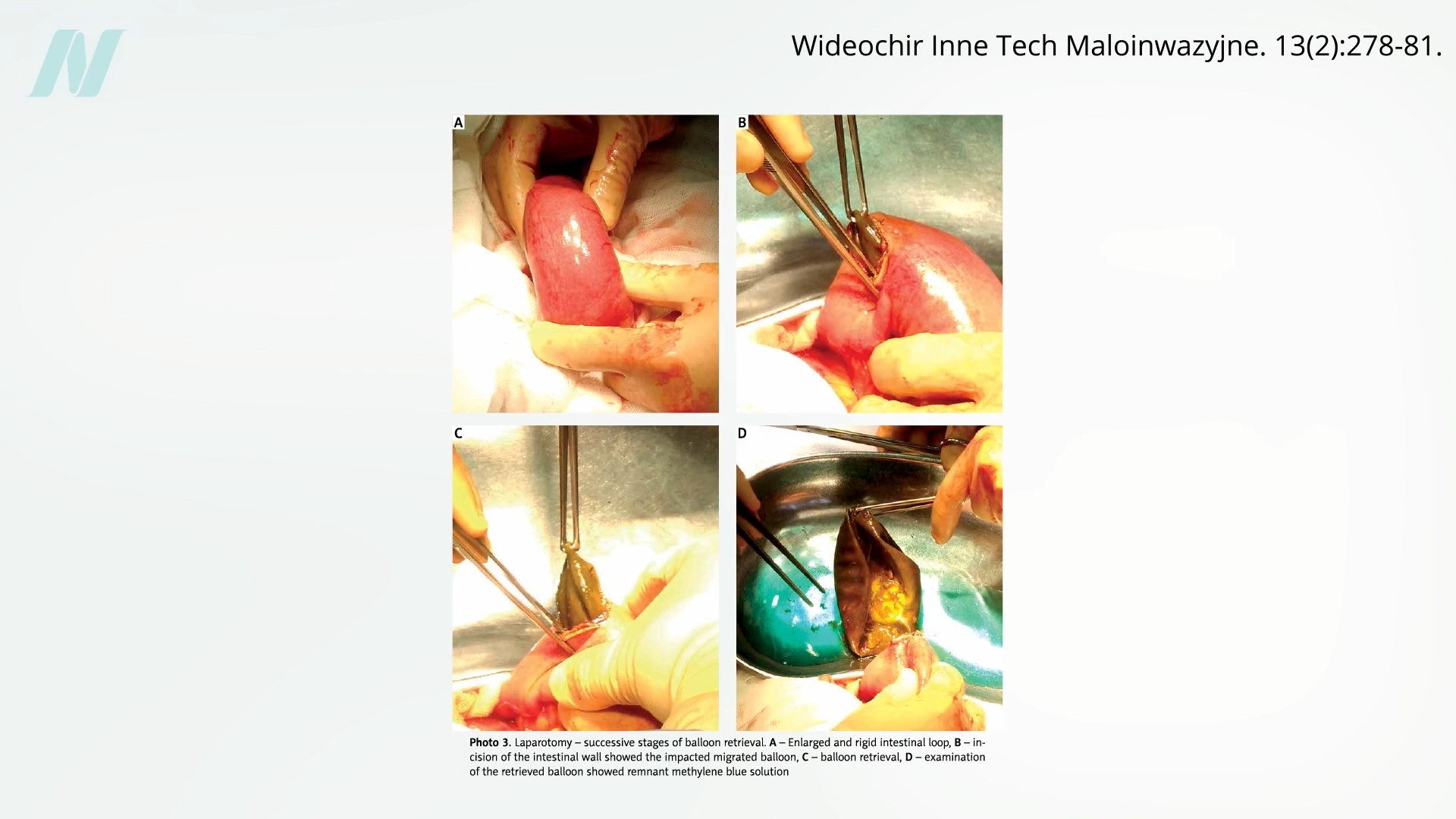
However, the history of medical devices, as the original reporting highlights, is often punctuated by their premature introduction to the market, frequently outpacing rigorous scientific validation of their safety and effectiveness. Intragastric balloons proved to be no exception. Early enthusiasm was soon tempered by concerning clinical observations. A pivotal study conducted at the Mayo Clinic revealed a disturbing failure rate: eight out of every ten intragastric balloons spontaneously deflated. This inherent unreliability presented not only a lack of efficacy but also a tangible risk of serious complications. When a deflated balloon passed into the intestines, it could cause a potentially life-threatening bowel obstruction. The visual evidence accompanying such reports, often depicting the physical consequences of such blockages, underscored the gravity of these risks.
Beyond the mechanical failures, the balloons also exacted a physiological toll. Even before spontaneous deflation, a significant percentage of patients – approximately half – experienced gastric erosions, indicating damage to the stomach lining. This damage could manifest as pain, discomfort, and, in severe cases, bleeding. The cumulative evidence began to paint a troubling picture: these devices were not only prone to failure but also carried a considerable risk of harm.
Perhaps the most damning indictment of the early intragastric balloons came from their comparative effectiveness. When pitted against established non-surgical approaches such as dietary changes and behavioral modification strategies, the balloons failed to demonstrate a statistically significant advantage in inducing sustainable weight loss. This finding was particularly concerning, as it suggested that the risks and potential harms associated with the devices were not offset by a commensurate benefit. Consequently, intragastric balloons were eventually withdrawn from the market, a testament to their insufficient efficacy and unacceptable risk profile.

The Return of the Balloon: A New Era, Familiar Concerns
After a hiatus of more than three decades, intragastric balloons made a resurgence in the United States. In 2015, the U.S. Food and Drug Administration (FDA) began approving a new generation of these devices. This reintroduction coincided with the implementation of the Sunshine Act, a piece of legislation designed to foster transparency in financial relationships between healthcare providers and the medical industry. The Act mandated the disclosure of payments made by drug and device companies to physicians, aiming to shed light on potential conflicts of interest.
The renewed availability of intragastric balloons saw a rapid uptake, with over 5,000 devices implanted within a relatively short period. This period also saw the medical community grappling with a growing awareness of the financial ties between physicians and pharmaceutical and device manufacturers. While the "cozy" relationships between doctors and "Big Pharma" became more widely recognized, the financial entanglements between surgeons and medical device companies remained a less understood, yet equally significant, issue. Publicly available data, such as reports detailing the substantial payments – an astonishing $12 million in a single year for the top 100 physician recipients – from device companies to physicians, highlighted the scale of these financial incentives. Disturbingly, many surgeons receiving these payments failed to disclose these conflicts of interest in their published research, undermining the objectivity of their findings.
While intragastric balloons are presented as reversible, a key advantage over more permanent bariatric surgical procedures, this reversibility does not equate to safety. The FDA has issued multiple advisories detailing the potential risks associated with these devices, including the ultimate risk of death. The mechanism of such a severe outcome can be indirect but devastating. The presence of the balloon can trigger persistent nausea and vomiting, conditions that are remarkably common, affecting the majority of patients. In extreme cases, forceful and prolonged vomiting can lead to a rupture of the stomach, a catastrophic event with a high mortality rate. Furthermore, persistent vomiting can contribute to life-threatening nutrient deficiencies, underscoring the systemic impact these devices can have.
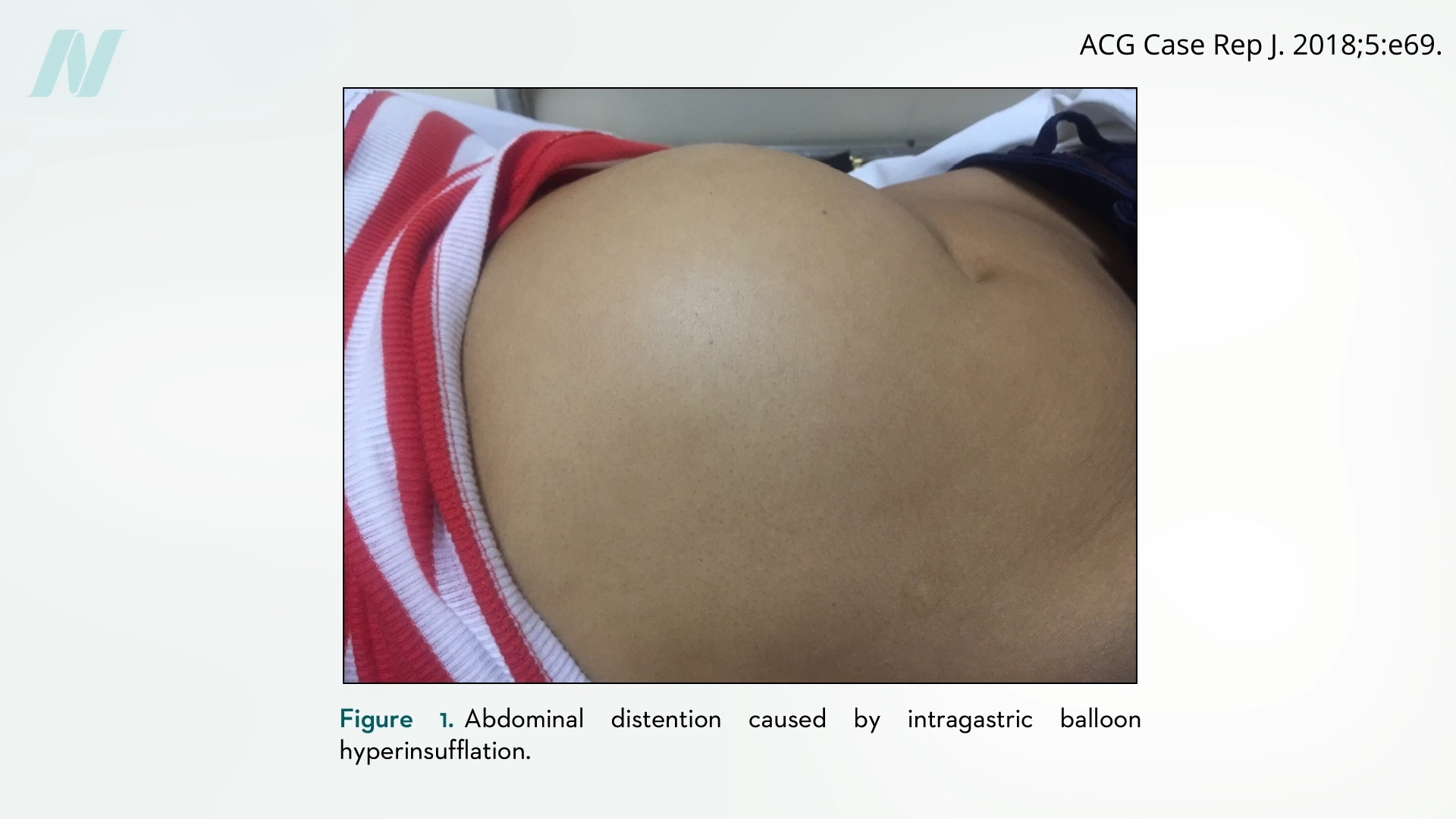
The complications associated with intragastric balloons are not limited to deflation. Some adverse events stem from the opposite problem: spontaneous overinflation. This phenomenon, where the balloon unexpectedly expands beyond its intended capacity, can lead to intense pain, vomiting, and severe abdominal distension. This issue first gained attention in the context of breast implants, where reports documented "spontaneously autoinflating breast implants" that could increase breast volume significantly. This poorly understood and underreported phenomenon also had a historical link to intragastric balloons, as early experimental versions of these weight-loss devices were, in some instances, derived from breast implant technology.
The Unsettling Truth of Sham Surgery Trials
The concept of "sham surgery" emerged as a critical tool for discerning the true efficacy of surgical interventions. In clinical trials, particularly those involving interventions where a placebo effect is significant, it becomes crucial to isolate the specific therapeutic effect of the procedure from the psychological impact of undergoing surgery. While drug trials can utilize inert sugar pills as a placebo, the equivalent for surgery is far more complex and ethically challenging.
The Knee Arthroscopy Revelation
A landmark study published in The New England Journal of Medicine in 2002 fundamentally challenged the established efficacy of one of the most frequently performed orthopedic surgeries: arthroscopic knee surgery. Billions of dollars are expended annually on procedures involving the insertion of arthroscopes into knee joints and the removal of damaged tissue, primarily for osteoarthritis and knee injuries. The study aimed to determine whether these interventions truly offered a benefit beyond the placebo effect.
Researchers recruited patients suffering from knee pain and randomly assigned them to one of three groups: those who received the actual arthroscopic surgery, those who underwent a sham surgery, and those who received only a placebo (a superficial incision without any manipulation of the joint). In the sham surgery group, surgeons made incisions and mimicked the procedural steps, even splashing saline into the joint, but crucially, they did not perform the actual debridement or repair.
The publication of these findings generated considerable controversy and outcry within the medical community. Professional medical associations questioned the ethics of subjecting patients to fake surgeries and the rationale of patients who consented to such trials. However, the results were undeniable: patients who received the actual surgery experienced improvements in their knee pain, but so did the patients in the sham surgery group. The graph depicting the outcomes clearly illustrated that the improvement in the placebo group was comparable to that in the surgical group. This indicated that the perceived benefits of arthroscopic knee surgery were largely attributable to the placebo effect, with the surgical intervention itself offering no additional therapeutic advantage.
This study had profound implications. It suggested that the billions of dollars spent on arthroscopic knee surgery might be largely misallocated, and that patients were potentially undergoing invasive procedures with significant recovery times and risks for no discernible clinical gain. The impact of this research has been far-reaching, leading to a reevaluation of surgical indications and a greater emphasis on evidence-based practice in orthopedics.
Rotator Cuff Surgery and the Crisis of Confidence
The revelations from the knee arthroscopy trial have reverberated across other surgical specialties. Currently, rotator cuff shoulder surgery is facing a similar "crisis of confidence." Emerging research and re-examinations of existing data suggest that the effectiveness of these procedures may also be subject to the pervasive influence of the placebo effect. This ongoing scrutiny highlights a broader trend: a critical reassessment of surgical interventions that have long been considered standard of care, driven by a demand for more robust evidence of efficacy.
Intragastric Balloons Re-Examined Through the Lens of Sham Trials
When intragastric balloons were subjected to sham-controlled trials, the results mirrored the findings in orthopedic surgery. These sham trials demonstrated that both older and newer iterations of these devices frequently failed to provide any significant weight-loss benefit. Even in instances where some weight loss was observed, it was often temporary. This was partly due to the prescribed six-month limit for balloon placement, a duration dictated by the increasing risk of deflation and subsequent complications. Attempts to prolong the use of balloons or to replace them with new ones did not yield improved long-term weight outcomes. Sham-controlled trials further revealed that any initial effects on appetite and satiety tended to diminish over time, suggesting that the body adapted to the presence of the balloon, rendering its impact negligible.
The Broader Implications: A Medical "Fake News" Phenomenon?
The insights gleaned from sham surgery trials present a sobering reflection on the medical field. Doctors often pride themselves on their adherence to scientific principles, and the medical community rightly condemns the anti-vaccination movement and the trend of individuals "choosing their own facts." However, when evidence emerges that popular surgical procedures are not only ineffective but may even exacerbate patient conditions – for instance, increasing the likelihood of requiring a total knee replacement – it becomes difficult to dismiss the possibility of a parallel to "fake news" and "alternative facts" within medicine itself.
The implications of these findings are multifaceted and far-reaching:
- Patient Welfare: The primary concern is the welfare of patients who undergo procedures that offer no tangible benefit, expose them to unnecessary risks, and incur significant financial costs.
- Healthcare Spending: The widespread adoption of ineffective surgeries contributes to the escalating costs of healthcare, diverting resources that could be allocated to treatments with proven efficacy.
- Medical Industry Influence: The financial incentives within the medical device industry, as highlighted by the Sunshine Act disclosures, raise serious questions about the objectivity of research and the drivers behind the promotion of certain procedures.
- Ethical Considerations: The use of sham surgeries, while ethically contentious, has proven indispensable in revealing truths that might otherwise remain hidden. This necessitates a continuous dialogue about ethical research methodologies and patient consent.
- The Future of Surgery: The findings underscore the urgent need for rigorous, independent, and sham-controlled trials for a wide range of surgical interventions to ensure that medical practice is grounded in robust scientific evidence.
Conclusion: Towards Evidence-Based Medicine
The evidence emerging from sham surgery trials serves as a critical reminder that the practice of medicine must constantly evolve, guided by scientific inquiry and a commitment to patient well-being. As the medical field continues to advance, a vigilant approach, characterized by critical evaluation, transparency, and an unwavering dedication to evidence-based practice, is paramount. The journey towards truly effective and safe medical interventions requires confronting uncomfortable truths and embracing the rigorous scrutiny that ultimately benefits us all.
Doctor’s Note: This article is part of a two-part series. The subsequent installment, "Extreme Weight-Loss Devices," will delve further into related topics. For comprehensive information on bariatric surgery and sustainable weight management, readers are encouraged to consult related posts and resources. The book How Not to Diet offers in-depth strategies for sustainable weight loss and is available through libraries and booksellers, with all proceeds donated to charity.