The landscape of bariatric weight-loss surgery, while offering a potential pathway to improved health for individuals struggling with severe obesity, is accompanied by a complex array of risks. Emerging evidence suggests that a critical determinant of patient outcomes is not solely the procedure itself, but the technical proficiency and experience of the surgeon performing it. This realization comes as revision surgeries, often necessitated by complications from initial bariatric procedures, are becoming increasingly common, highlighting the need for meticulous surgical execution from the outset.
The Rising Tide of Revision Surgeries
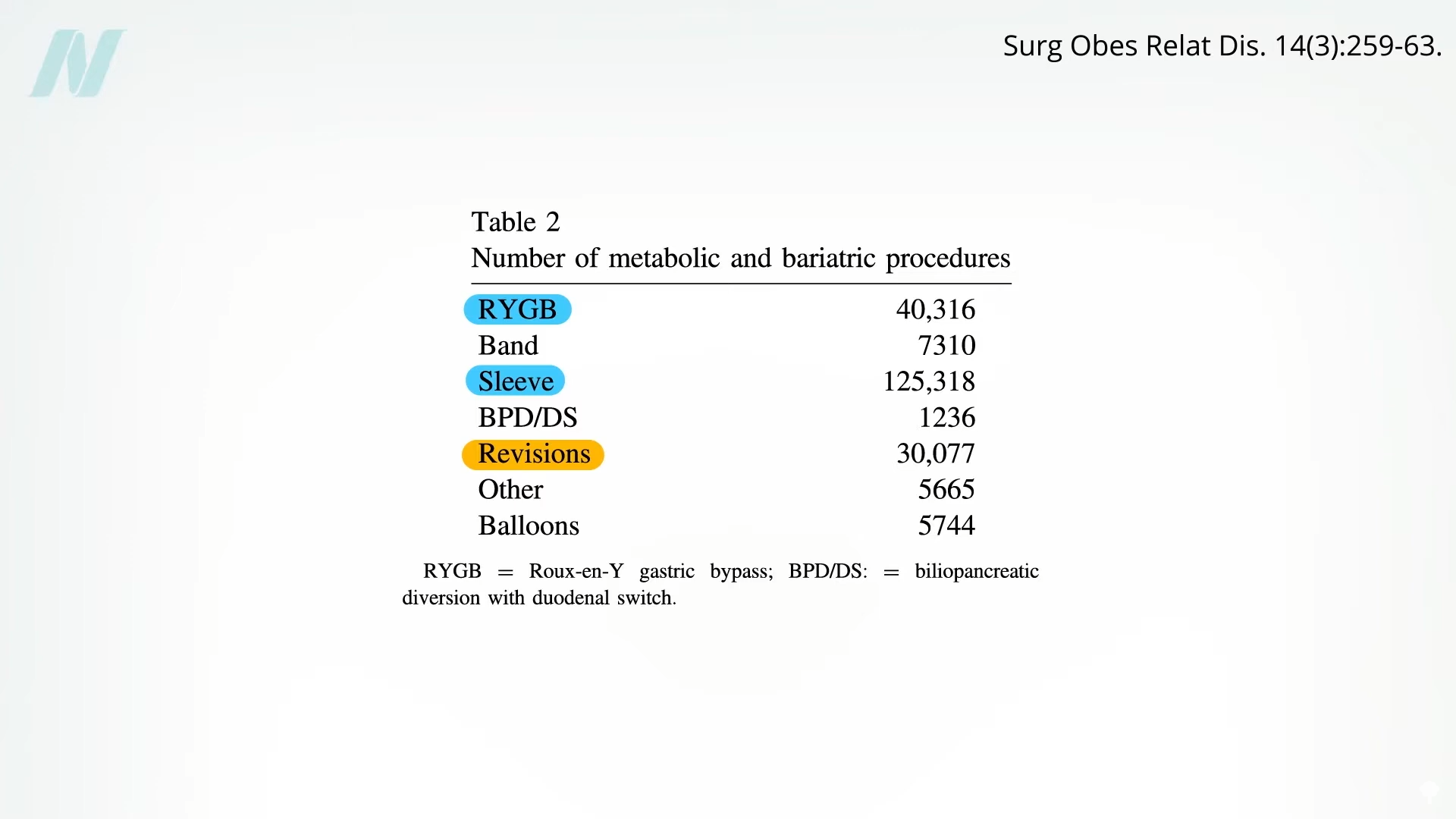
Following the two most prevalent bariatric procedures, namely sleeve gastrectomy and Roux-en-Y gastric bypass, the third most frequent operation in this field is a revision to correct issues arising from a prior bariatric intervention. This trend underscores a significant concern within the surgical community and among patients considering these life-altering operations. Data indicates that a substantial percentage of bariatric patients, potentially up to 25%, may require a return to the operating room to address complications stemming from their initial surgery.
These subsequent reoperations carry a disproportionately higher risk profile. Mortality rates for revision surgeries can be as much as ten times greater than those for primary procedures, and the assurance of a successful outcome is notably absent. The spectrum of potential complications is broad, encompassing leaks at surgical sites, the formation of abnormal connections between organs (fistulas), the development of internal sores (ulcers), narrowing of surgical passages (strictures), tissue breakdown (erosions), blockages in the digestive tract (obstructions), and severe gastroesophageal reflux.
Surgeon Proficiency: A Key Differentiator in Patient Safety
The variability in these complication rates has led researchers to investigate factors that might explain such disparities. A pivotal study, published in the esteemed New England Journal of Medicine, shed light on the direct correlation between surgeon skill and patient outcomes. In this groundbreaking research, bariatric surgeons voluntarily submitted video recordings of their surgical procedures to a panel of their peers for rigorous evaluation. The assessment focused on technical proficiency, and the findings were stark: a wide range in skill levels was observed, and this variation was demonstrably linked to differing rates of complications, hospital readmissions, the necessity for reoperations, and even mortality.
The study revealed that patients who underwent surgery performed by less experienced or less technically adept surgeons experienced nearly three times the rate of complications and a five-fold increase in the likelihood of death compared to those treated by highly proficient surgeons. This research suggests that, much like in highly skilled professions such as music or athletics, innate talent may play a role, but extensive practice and dedicated training are indispensable for achieving surgical mastery.
The Learning Curve: Quantifying Experience and Its Impact
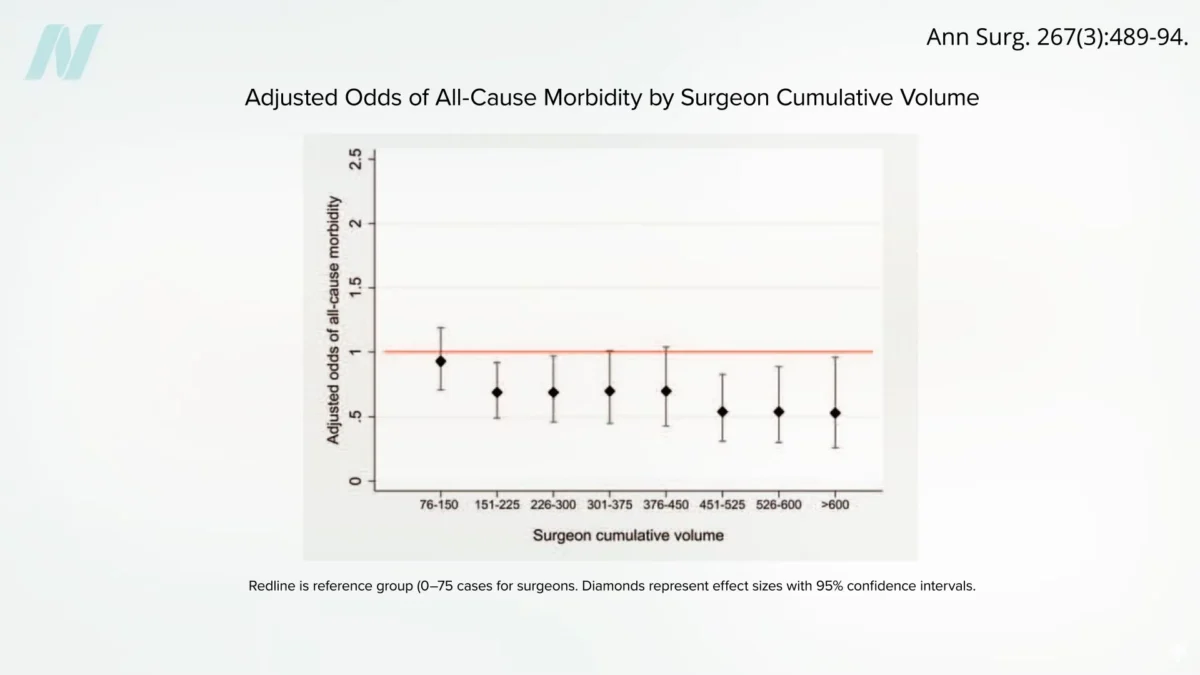
The intricate nature of bariatric procedures, particularly the gastric bypass, necessitates a substantial learning curve for surgeons. Estimates suggest that a surgeon may need to perform approximately 500 cases before achieving a level of mastery that significantly plateaus the risk of complications. Data indicates that the lowest risk profiles are observed among surgeons who have successfully completed more than 600 bypass procedures.

Further analysis from this research highlights the dramatic difference in risk based on surgical volume. Patients operated on by surgeons who have performed fewer than 75 procedures face approximately double the odds of mortality compared to those treated by surgeons with experience exceeding 450 cases. This data provides a critical metric for patients to consider when selecting a surgeon.
Navigating the Choice: Patient Empowerment Through Information
The implications of these findings are profound for patients contemplating bariatric surgery. The advice from experts is clear: prospective patients should not hesitate to inquire about the number of bariatric procedures a surgeon has performed. This straightforward question can provide invaluable insight into their level of experience.
Beyond individual surgeon experience, choosing a bariatric surgery facility that has been designated a "Center of Excellence" is also strongly recommended. These accredited institutions adhere to stringent quality standards and have demonstrated a commitment to patient safety and optimal outcomes. Studies indicate that surgical mortality rates at accredited Centers of Excellence are two to three times lower than those at non-accredited facilities, further underscoring the importance of institutional accreditation.
Beyond the Scalpel: Patient Adherence and Dietary Pitfalls
While surgeon skill is a critical factor, it is not the sole determinant of surgical success or patient safety. The adherence to post-operative dietary guidelines and lifestyle changes by patients also plays a vital role in preventing complications. A cautionary anecdote illustrates this point: a surgeon recounted a case where a patient, three months after a gastric bypass, consumed an excessive amount of food at an all-you-can-eat buffet without adequate chewing. This oversight led to the rupture of surgical staples and an emergency reoperation. The patient’s abdominal cavity was found to contain undigested chunks of broccoli, whole lima beans, and other fibrous vegetables.
While this incident serves as a vivid reminder of the importance of proper chewing and food preparation, it also prompts a broader reflection. The emphasis should not solely be on post-operative chewing habits, but critically on the fundamental dietary choices made before and after surgery. A diet rich in whole, unprocessed foods that are well-chewed and properly digested is paramount for maintaining the integrity of internal organs and ensuring long-term health.
The Lifelong Commitment: Nutritional Replenishment and Monitoring
Even in cases where the surgical procedure itself is technically flawless, bariatric surgery necessitates a lifelong commitment to nutritional replacement and vigilant monitoring. This is due to the inherent malabsorptive nature of many bariatric procedures, particularly gastric bypass. By intentionally altering segments of the digestive tract, these operations can significantly impair the absorption of calories, but at the significant cost of hindering the uptake of essential vitamins and minerals.
The consequences of these persistent nutritional deficits can be severe and extend far beyond common issues like anemia, osteoporosis, or hair loss. Patients are at risk of developing life-threatening deficiencies, including beriberi (a thiamine deficiency), pellagra (a niacin deficiency), kwashiorkor (a severe protein deficiency), and irreversible nerve damage. For instance, copper deficiency can manifest as vision loss years or even decades after surgery. Tragically, in reported cases of severe thiamine deficiency, a B vitamin crucial for neurological function, nearly one in three patients suffered permanent brain damage before the condition was identified and treated.

Even restrictive procedures, such as stomach stapling, can pose risks for life-threatening nutrient deficiencies, often exacerbated by persistent vomiting. This vomiting, reported by up to 60% of patients following bariatric surgery, is frequently attributed to "inappropriate eating behaviors," which essentially means attempting to consume food in a manner that is incompatible with the surgically altered anatomy. While vomiting can contribute to weight loss by reducing calorie intake, its persistent nature can lead to severe nutritional depletion.
Behavioral Modification and the "Dumping Syndrome"
Another significant post-surgical phenomenon is "dumping syndrome." This condition affects a large percentage of gastric bypass patients, characterized by symptoms such as abdominal pain, diarrhea, nausea, bloating, fatigue, and palpitations that occur after consuming calorie-dense foods. The underlying mechanism involves the rapid passage of food from the stomach pouch directly into the intestines, bypassing the normal digestive process.
Surgeons often describe dumping syndrome not as an unintended complication, but as an integral and even desirable feature of the behavioral modification achieved by gastric bypass surgery. The unpleasant physiological response serves as a powerful deterrent, discouraging patients from consuming high-energy foods and thereby contributing to weight loss. This mechanism functions similarly to certain medications used in alcohol addiction treatment, where the severe adverse reaction to alcohol consumption reinforces abstinence.
Broader Context and Future Directions
This exploration of the complexities surrounding bariatric surgery is part of a larger series aimed at providing comprehensive information on the topic. The preceding installment focused on "The Mortality Rate of Bariatric Weight-Loss Surgery," laying the groundwork for understanding the inherent risks.
Future discussions will delve into critical comparative analyses, examining "Bariatric Surgery vs. Diet to Reverse Diabetes" and exploring the long-term sustainability of weight loss after these procedures in a segment titled "How Sustainable Is the Weight Loss After Bariatric Surgery?"
For individuals seeking to understand sustainable weight loss strategies, the book How Not to Diet offers an in-depth exploration of evidence-based approaches. The author emphasizes the importance of consulting local libraries or bookstores for access, with all proceeds from book sales being donated to charitable causes.
The discourse surrounding bariatric surgery is multifaceted, encompassing surgical technique, patient behavior, and long-term physiological management. As the field evolves, a continued focus on surgeon education, patient empowerment through informed decision-making, and rigorous post-operative care will be crucial in optimizing outcomes and mitigating the inherent risks associated with these powerful interventions.






