The growing global epidemic of type 2 diabetes, affecting over half a billion adults worldwide with projections indicating a 50% increase within a generation, is increasingly being viewed through the lens of metabolic health and weight management. Emerging research and historical observations suggest that significant weight loss, particularly for individuals diagnosed with type 2 diabetes for less than four years, can lead to remission in a substantial majority of cases. This paradigm shift moves beyond solely relying on medication, highlighting the profound impact of lifestyle interventions on reversing the disease.
The Historical Context of Dietary Intervention in Diabetes
The concept of using dietary restriction to manage diabetes is not new; it dates back centuries. Ancient Ayurvedic texts, as far back as 2,000 years ago, proposed stringent measures for individuals with diabetes, including prolonged fasting, arduous physical activity, or even extreme dietary limitations. These historical approaches, while perhaps lacking in modern scientific rigor, underscored a fundamental understanding that excess intake was linked to the condition.
In 1797, Dr. John Rollo proposed a diet for diabetes that, while historically significant, employed methods that would be considered harsh and potentially dangerous by today’s medical standards. His regimen included rancid meat and the use of emetic drugs to induce vomiting, primarily aiming to reduce food intake. The underlying principle, however, was that severe caloric restriction could temporarily alleviate symptoms.
A more formalized, albeit still severe, approach emerged during the siege of Paris in the Franco-Prussian War. The scarcity of food during this period led to observed improvements in diabetic patients, prompting the advice "mangez le moins possible" – eat as little as possible. This observation was later codified into the Allen starvation treatment by Dr. Frederick M. Allen. Before the discovery of insulin, the Allen treatment was considered a groundbreaking advance in diabetes management.
Dr. Allen’s work was informed by clinical reports that indicated diabetes symptoms could improve in individuals experiencing "wasting conditions" such as tuberculosis or cancer. He hypothesized that severe caloric restriction, similar to the effects of these illnesses, could be therapeutically beneficial. His studies demonstrated that even in severe diabetes cases, urinary sugar could be eliminated within ten days through drastic dietary limitations. However, maintaining this remission proved challenging once patients resumed normal eating patterns. Allen’s core principles for managing diabetes were to maintain an underweight status and severely restrict dietary fat. He observed that even moderate fat intake, such as butter or olive oil, could trigger a relapse of diabetes symptoms.
Understanding Type 2 Diabetes as a Disease of Fat Toxicity
Contemporary scientific understanding increasingly supports the idea that type 2 diabetes is fundamentally a disease linked to excess fat accumulation within the body, particularly in key metabolic organs. This "fat toxicity" model suggests that the body’s ability to process glucose efficiently is compromised by an overload of fat.
Research utilizing advanced imaging techniques, such as high-field MRI, has provided compelling evidence for this. Infusing fat intravenously into individuals has been shown to cause fat to accumulate in muscle cells within hours, leading to a rapid increase in insulin resistance. Similarly, studies involving high-fat diets have demonstrated that even a three-day regimen can induce significant insulin resistance. Alarmingly, some research indicates that even a single high-fat meal can increase insulin resistance within six hours, and acute dietary fat intake can rapidly exacerbate this condition.
The implications of this are profound. Insulin resistance in muscle tissue, when coupled with excess caloric intake, can lead to a cascade of metabolic dysfunction. This often begins with fat accumulation in the liver, a condition known as non-alcoholic fatty liver disease (NAFLD). The progression continues with fat accumulation in the pancreas, the organ responsible for insulin production. This pancreatic fat infiltration can impair beta-cell function, leading to insufficient insulin production and ultimately manifesting as full-blown type 2 diabetes.

As noted by researchers, "Type 2 diabetes can now be understood as a state of excess fat in the liver and pancreas, and remains reversible for at least 10 years in most individuals." This understanding shifts the focus from simply managing blood sugar levels to addressing the underlying metabolic derangements.
The Efficacy of Weight Loss in Achieving Diabetes Remission
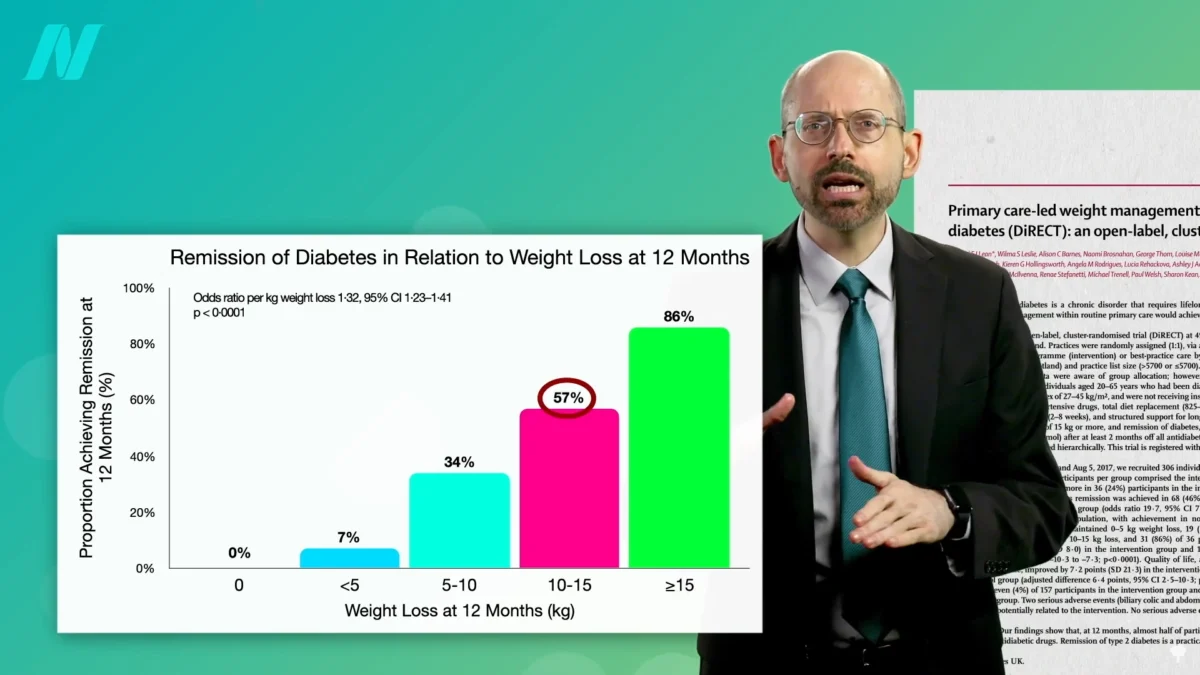
The compelling link between excess body fat and type 2 diabetes has led to a renewed focus on weight loss as a primary therapeutic strategy. Recent studies have provided robust data on the efficacy of achieving specific weight loss milestones for diabetes remission.
A significant finding indicates that individuals who have had type 2 diabetes for less than four years can achieve non-diabetic blood sugar levels in nearly 90% of cases by losing just 15% of their body weight. This is a remarkable success rate, particularly when contrasted with the outcomes of bariatric surgery. While bariatric surgery also leads to significant weight loss and can induce remission, studies have shown lower remission rates, approximately 62% for those losing more weight in the surgical group, compared to the 90% achieved with a 15% body weight loss through other means. For individuals who have lived with type 2 diabetes for longer than eight years, the remission rate with a 15% weight loss drops to around 50%.
Furthermore, research suggests that the average duration of diagnosis for individuals who can reverse their type 2 diabetes is approximately three years, often achieved through a weight loss of around 30 pounds. This data underscores the importance of early intervention and the potential for sustained remission when weight loss is achieved relatively soon after diagnosis.
Mechanisms of Action: How Weight Loss Reverses Diabetes
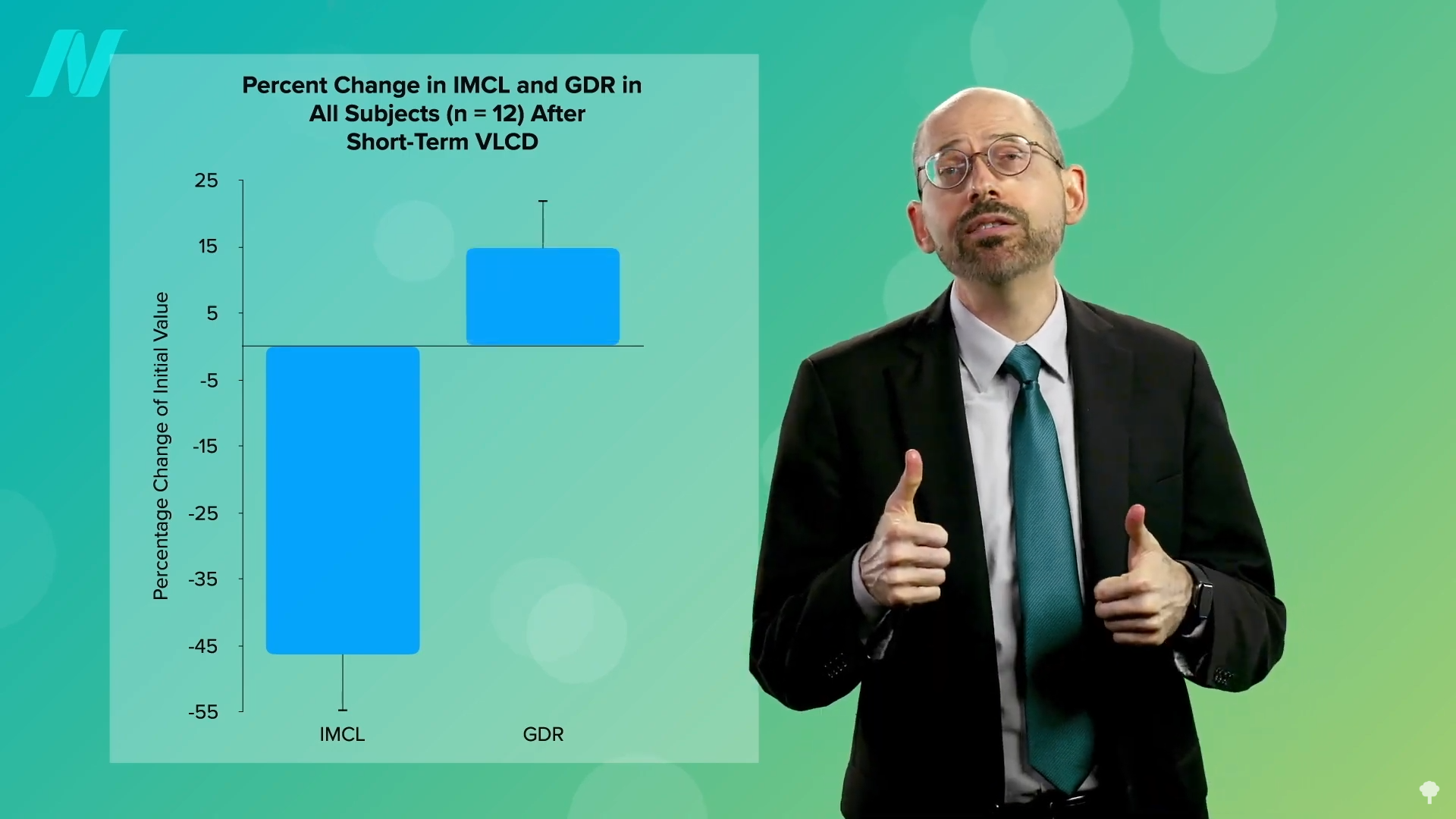
The reversal of type 2 diabetes through weight loss is directly linked to the reduction of ectopic fat – fat stored in organs where it doesn’t normally reside, such as the liver and pancreas. When individuals undertake a very low-calorie diet, typically around 700 calories per day, the body begins to mobilize stored fat. This process leads to a significant reduction in fat within muscle cells, which in turn enhances insulin sensitivity. Improved insulin sensitivity means that the body’s cells can more effectively respond to insulin, allowing glucose to enter the cells for energy and lowering blood sugar levels.
As the dietary intervention continues, the excess fat stored in the liver begins to decrease substantially. If the diet is maintained, this reduction extends to the pancreas, alleviating the fat infiltration that impairs insulin production and function. This reduction in pancreatic fat can restore beta-cell function, allowing the body to produce and utilize insulin effectively, thereby reversing the diabetic state.
The Role of Fasting and Very Low-Calorie Diets
While the term "fasting" has historical connotations of starvation, modern medical approaches utilize medically supervised fasting and very low-calorie diets (VLCDs) as powerful tools for initiating significant weight loss and metabolic reset. These interventions are designed to be short-term and are conducted under strict medical supervision to ensure safety and effectiveness.
The goal of these VLCDs is to rapidly deplete the body’s fat stores, particularly the ectopic fat contributing to insulin resistance. Studies have shown that such interventions can lead to substantial improvements in insulin sensitivity and glucose control within a matter of weeks. For instance, a VLCD of 700 calories per day has been demonstrated to effectively pull fat out of muscle cells, leading to a corresponding boost in insulin sensitivity.
However, the long-term success of diabetes reversal hinges on sustained lifestyle changes. While an extended period of physician-supervised water-only fasting can achieve remission, maintaining that weight loss is crucial. Evidence suggests that weight regain is directly correlated with the return of diabetes. This highlights the necessity of transitioning from an acute intervention like VLCDs or fasting to a sustainable, healthy dietary pattern and regular physical activity.
Beyond Weight Loss: The Importance of Diet Quality and Exercise
While weight loss is a critical component, the quality of the diet adopted post-intervention plays a pivotal role in maintaining remission. The historical emphasis on restricting fat, as noted by Dr. Allen, remains relevant. Modern nutritional science emphasizes whole, unprocessed foods, with a focus on plant-based diets that are rich in fiber, vitamins, and minerals, and low in saturated and trans fats, as well as refined carbohydrates and added sugars.
Elliott Joslin, a prominent pioneer in diabetes care, recognized the enduring importance of self-discipline in diet and exercise, even after the advent of insulin. He argued that these lifestyle factors should remain central to diabetes management. This perspective is increasingly validated, as sustainable remission requires a long-term commitment to healthy eating habits and regular physical activity. Exercise not only aids in weight management but also directly improves insulin sensitivity, further contributing to metabolic health.
Implications and Future Directions
The growing body of evidence supporting the reversibility of type 2 diabetes through weight loss has significant implications for public health policy, clinical practice, and individual patient care.
Clinical Practice: Healthcare providers are increasingly encouraged to assess patients’ weight and discuss the potential for diabetes remission through structured weight loss programs. This may involve referral to dietitians, endocrinologists specializing in metabolic disorders, or participation in medically supervised weight loss programs.
Public Health: A greater emphasis on preventative strategies, including promoting healthy eating habits and regular physical activity from an early age, is crucial to curb the rising tide of diabetes. Public health campaigns can educate the population about the link between obesity, metabolic health, and type 2 diabetes, empowering individuals to make informed choices.
Patient Empowerment: Understanding that type 2 diabetes can be a reversible condition can empower patients to take a more proactive role in their health. This shift in perspective can foster greater motivation and adherence to lifestyle changes, leading to better long-term outcomes.
Economic Impact: The successful reversal of type 2 diabetes can lead to substantial reductions in healthcare costs associated with managing the disease and its numerous complications, such as cardiovascular disease, kidney failure, blindness, and amputations.
While the discovery of insulin in 1921 was a life-saving breakthrough, particularly for type 1 diabetes, it became evident that it was not a cure for type 2 diabetes, nor did it prevent its debilitating long-term complications when used alone. The focus has now evolved to recognize that addressing the root causes of type 2 diabetes, primarily excess body fat and associated metabolic dysregulation, offers a pathway to not just manage but potentially reverse the condition. The "forks" of dietary change, in this context, are proving to be more potent than the "knives" of surgical intervention for many individuals seeking to reclaim their health from type 2 diabetes. The journey towards remission is challenging but achievable, underscoring the profound impact of weight loss and sustained healthy lifestyle choices on metabolic health.






