The pursuit of significant weight loss has, throughout history, led to the development and exploration of a wide array of methods, some bordering on the extreme and raising serious questions about safety and efficacy. While conventional approaches like balanced diets and regular exercise remain the cornerstones of healthy weight management, a segment of the population, and indeed the medical and scientific communities, have investigated more radical interventions. This article delves into some of the most unconventional and, at times, alarming weight-loss strategies, examining their underlying principles, documented outcomes, and the critical concerns they present.
The fundamental challenge in weight loss often lies in the energy imbalance between caloric intake and expenditure. For an individual of moderate obesity engaging in moderately intense physical activity, such as biking or brisk walking, the caloric burn rate is approximately 350 calories per hour. In stark contrast, many processed foods and beverages are consumed at a rate of roughly 70 calories per minute. This disparity means that a mere five minutes of consuming high-calorie items can negate an entire hour of dedicated exercise, highlighting the significant uphill battle many face in managing their weight through traditional means alone. This imbalance has, in part, fueled the search for more direct or potent interventions.
The AspireAssist Siphon System: A Controversial Approach to Caloric Management
One such intervention that has garnered significant attention, and considerable controversy, is the AspireAssist siphon assembly. This device represents a highly invasive approach to weight management, fundamentally altering the digestive process after a meal. The AspireAssist system involves a percutaneous gastrostomy, a surgical procedure where a small opening is created in the abdominal wall, leading directly into the stomach. A tube, or fistula, is then tunneled from the stomach to the exterior of the body.
Mechanism of Action and Patient Experience
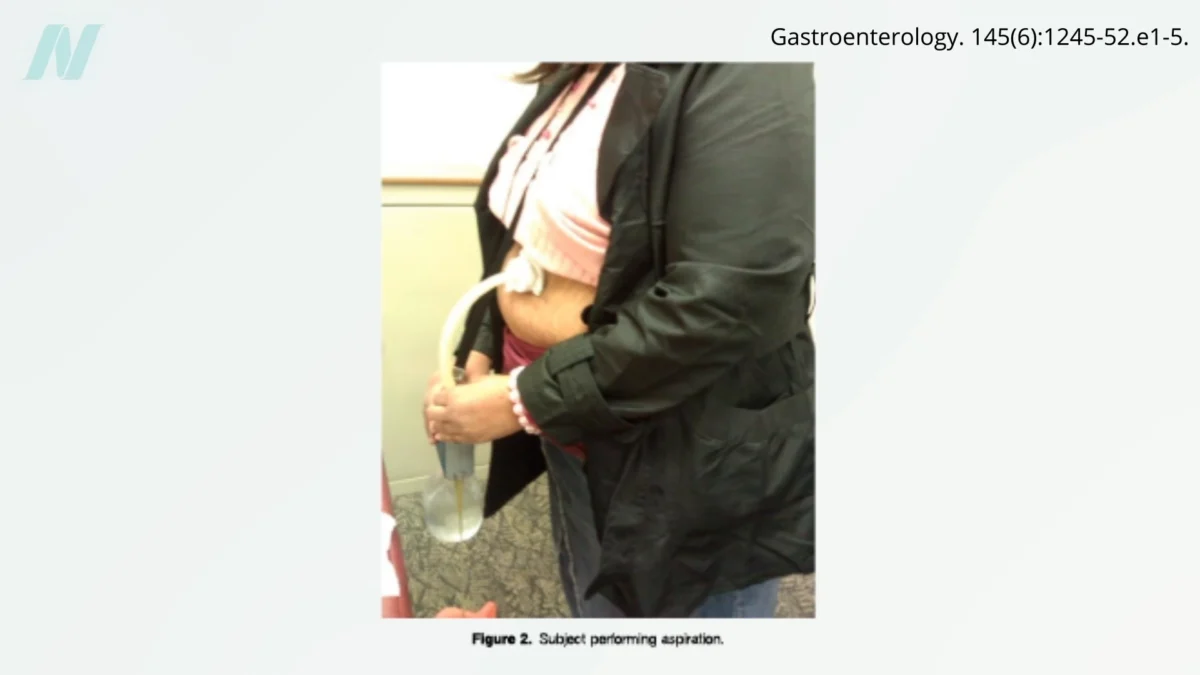
Following a meal, individuals equipped with the AspireAssist device can attach a special external apparatus to the abdominal opening. This device then allows for the siphoning of a portion of the stomach’s contents directly out of the body. This process effectively removes a significant percentage of the ingested calories before they can be fully absorbed by the digestive system. The theoretical implication is that individuals can consume food and then immediately purge a substantial amount of it, thereby creating a drastic caloric deficit.
This method has been described as allowing individuals to "gorge on donuts, spew them out through the hole in your stomach, then gorge on more donuts." The underlying principle hinges on decoupling the act of eating from nutrient absorption. While the visual and psychological implications of such a process are undeniably unsettling, the AspireAssist system has demonstrated weight loss in clinical trials.
Documented Outcomes and Contributing Factors
Studies on the AspireAssist system have indicated that patients do experience weight reduction. Several factors are believed to contribute to this outcome beyond the direct caloric removal. The presence of the gastric fistula itself may interfere with the normal relaxation of the stomach wall during a meal, potentially leading to earlier feelings of fullness and reduced food intake. Furthermore, the procedure necessitates the consumption of substantial amounts of water and requires patients to thoroughly chew their food. Both of these practices can aid in weight loss by promoting hydration and slowing the rate of eating, respectively.
An unexpected psychological benefit has also been observed. Patients using the AspireAssist system reportedly began making healthier food choices. The visual unpleasantness of aspirating gastric contents from unhealthy foods, particularly fried items which appear visibly unappetizing when siphoned, served as a powerful deterrent. This "disgust factor" appears to have motivated some individuals to opt for foods that would be less visually offensive when removed.
Safety Considerations and Adverse Effects
Despite its weight-loss efficacy, the AspireAssist system is not without its risks and requires careful medical management. A significant concern is the potential for electrolyte imbalance, specifically potassium deficiency, due to the removal of stomach juices. Patients are therefore required to supplement their intake of potassium to mitigate this risk, a complication that can also be seen in individuals with bulimia.
While serious adverse effects, such as abdominal abscesses, are reported to be rare, minor wound complications related to the gastrostomy site are more common. The AspireAssist device’s primary selling point, from a procedural perspective, is that it does not alter the fundamental anatomy of the gastrointestinal tract. This is a notable distinction in a landscape of weight-loss procedures that often involve significant surgical alterations.
The Duodenal-Jejunal Bypass Liner: A Less Invasive, Yet Risky, Alternative
Another intervention that bypasses significant portions of the digestive tract without resorting to extensive surgery is the duodenal-jejunal bypass liner. Traditional gastric bypass surgery achieves weight loss by surgically removing or excluding a section of the small intestine, thereby reducing calorie absorption. The duodenal-jejunal bypass liner, in contrast, involves the insertion of a flexible tube, typically made of plastic, that lines a portion of the intestinal walls.
Mechanism and Application
This liner effectively creates a barrier between the ingested food and the intestinal lining for a specific segment of the digestive tract. By preventing the direct contact of food with the duodenum and proximal jejunum – key sites for nutrient absorption – the device aims to reduce the number of calories absorbed by the body.
Adverse Events and Complications
The challenge with the EndoBarrier, as this type of liner is often known, lies in its anchoring mechanism. To remain in place within the dynamic environment of the digestive tract, the liner is secured using barbed hooks. These hooks, designed to embed into the intestinal wall, are responsible for a substantial number of reported adverse events. In one analysis of 1,056 patients, nearly 90% experienced adverse effects, with lacerations being the most common. More severe complications, such as penetrating trauma leading to esophageal perforation or liver abscesses, while rarer, have been documented, occurring in approximately 1 in 27 patients.
Intestinal Resurfacing: A Thermally Ablative Approach
Taking the concept of altering intestinal absorption to an even more extreme level is a procedure termed intestinal "resurfacing." While the AspireAssist pump has faced questions about its "palatability," intestinal resurfacing represents a particularly concerning development in the pursuit of weight loss.

The Procedure and Its Rationale
This method involves "thermally ablating the superficial duodenal mucosa." In simpler terms, it entails burning off, or "resurfacing," the lining of the intestine. The rationale behind such a drastic measure is to prevent nutrient absorption by damaging or removing the absorptive cells of the intestinal lining. The procedure aims to reduce the surface area available for nutrient uptake, thereby leading to a caloric deficit.
Ethical and Safety Concerns
The concept of intentionally damaging the intestinal lining raises profound ethical and safety concerns. The duodenal mucosa is a vital component of the digestive system, responsible for secreting hormones that regulate digestion and satiety, as well as playing a role in nutrient absorption. The long-term consequences of such damage, including potential impacts on overall digestive health, nutrient deficiencies, and the risk of inflammation or other complications, are significant and warrant extensive investigation.
Beyond Invasive Procedures: Exploring Less Conventional Methods
The landscape of weight-loss interventions extends beyond surgical and device-based approaches to include a variety of pharmacological, behavioral, and even biological strategies, some of which have proven to be ineffective or carry substantial risks.
Botox Injections: A Failed Pharmaceutical Intervention
In an attempt to leverage pharmaceutical agents, researchers have explored injecting Botulinum toxin (Botox) into the stomach walls of obese individuals. The hypothesis was that Botox, known for its muscle-paralyzing properties, could partially paralyze the gastric muscles, thereby slowing stomach emptying, promoting prolonged feelings of fullness, and ultimately leading to weight loss. However, clinical trials have demonstrated that this method did not work as intended, failing to achieve significant or sustainable weight loss.
Corsets: A Historical Fashion Fad with No Scientific Backing
The notion of physically constricting the body to influence weight loss has a long history. Researchers in Sweden conducted a study investigating the efficacy of wearing corsets for extended periods – 12 to 16 hours a day for nine months. The study’s findings were unequivocal: it didn’t work. Participants found the corsets to be "perceived as uncomfortable," leading to poor compliance and rendering the intervention ineffective. This highlights the disconnect between historical fads and scientifically validated weight-loss strategies.
Tapeworms: A Dangerous and Ineffective Parasitic Approach
Perhaps one of the most historically notorious and dangerous weight-loss fads involves the ingestion of "sanitized tapeworms." Advertised as a remedy since the early 1900s, the premise was that the tapeworm would reside in the digestive tract and consume ingested food, thereby reducing the host’s caloric intake. However, the reality is far more perilous. The presence of living tapeworms has been discovered during bariatric surgery operations, strongly suggesting that infesting oneself with these parasites is not only ineffective but also poses severe health risks. Tapeworm infections can lead to a range of debilitating symptoms, including abdominal pain, nausea, diarrhea, malnutrition, and even neurological complications.
Harnessing Disgust: A Psychological Intervention
In contrast to invasive or biologically risky methods, some research has explored psychological interventions. One study, titled "Harnessing the Power of Disgust: A Randomized Trial to Reduce High-Calorie Food Appeal Through Implicit Priming," investigated the use of subliminal messages to diminish the appeal of high-calorie foods. Researchers employed a priming technique where positive images (e.g., kittens) were flashed briefly before images of healthy foods, and negative images (e.g., cockroaches on pizza, vomit, burn wounds) were presented before images of high-calorie foods.
The results indicated that this method appeared to be effective, with subjects reporting a reduced desire to consume high-calorie foods. While not directly tested for actual food consumption, the researchers concluded that subliminal aversion could be a viable tactic to counteract the pervasive food cues that promote unhealthy eating habits in modern society.
International Perspectives and Evolving Scientific Inquiry
The relentless pursuit of weight-loss solutions in the United States has, at times, drawn bemused commentary from the international community. Publications have emerged with titles such as "Don’t Let Them Eat Cake! A View from Across the Pond" and "What Are the Yanks Doing?", reflecting a sense of bewilderment at some of the more unconventional American approaches.
Electrical Stimulation: A History of Unfulfilled Promises
Historically, the U.S. has seen various attempts to employ electrical stimulation for weight management. Studies have examined "The U.S. Experience with Implantable Gastric Stimulation," which involved inserting electrodes into the muscular layer of the stomach wall, and even colon electrical stimulation, neither of which yielded significant success.
More startling were investigations into "Repetitive electric brain stimulation reduces food intake in humans." Despite the inherent risks associated with deep-brain electrode placement, scientists have long pondered the possibility of modulating appetite through direct brain intervention. In some early experiments, holes were drilled into the skulls of obese individuals, and wires were inserted into their brains for "electrostimulatory exploration." The goal was to identify specific brain regions that, when stimulated, could elicit hunger responses. The researchers then applied electrical currents to create lesions in these areas, hoping to reduce appetite. While this approach showed some promise in animal models (cats and monkeys), the researchers ultimately found that burning holes in people’s brains did not result in weight loss in obese humans.
The Path Forward: Sustainable Weight Loss
The exploration of these extreme and often ethically questionable weight-loss methods underscores a critical point: healthy, sustainable weight loss is not synonymous with invasive procedures or unproven scientific endeavors. As emphasized in extensive research and publications like "How Not to Diet," effective weight management is rooted in evidence-based lifestyle changes. These typically involve a balanced dietary approach that prioritizes nutrient-dense foods, regular physical activity, and behavioral strategies that promote long-term adherence.
The medical community continues to explore safe and effective avenues for weight management, including discussions on the safety and efficacy of procedures such as gastric balloon surgery and pharmacological interventions. However, the overarching consensus remains that foundational principles of nutrition and exercise, coupled with robust psychological support, form the most reliable and health-conscious path toward achieving and maintaining a healthy weight. The multitude of extreme devices and procedures examined serves as a stark reminder of the importance of critical evaluation and adherence to scientifically validated methods.






