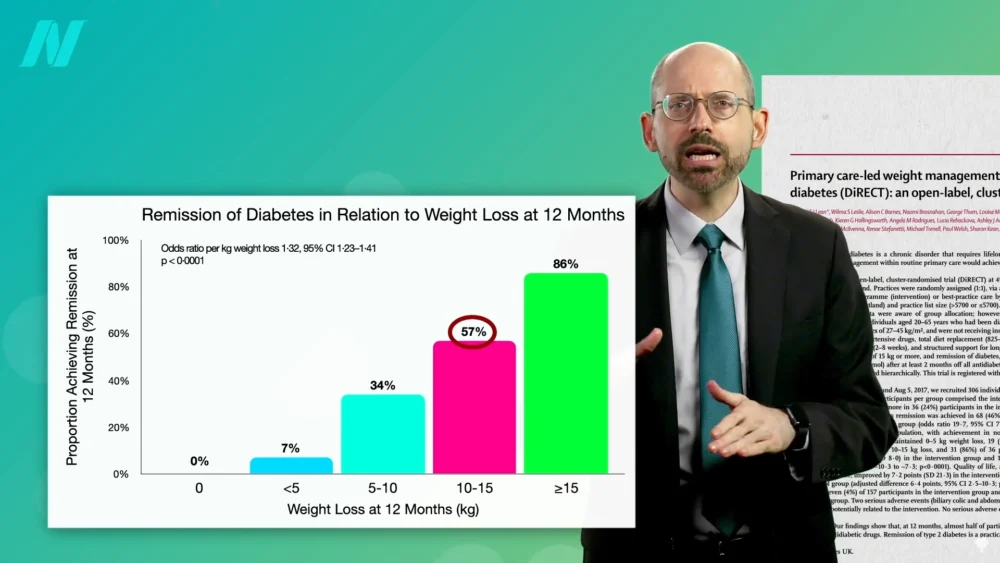
The global landscape of adult health is increasingly shaped by the pervasive presence of diabetes, with current estimates indicating that over half a billion adults worldwide are living with the condition. Projections suggest a concerning rise, with an approximate 50% increase anticipated within the next generation. This escalating health crisis has spurred extensive research into effective management and, critically, potential remission strategies. Emerging evidence and historical analysis suggest that significant weight loss, particularly in the early stages of type 2 diabetes, may offer a pathway to remission for a substantial proportion of affected individuals. Research indicates that losing just 15% of body weight can lead to remission in nearly 90% of individuals diagnosed with type 2 diabetes for less than four years. This finding is particularly impactful when contrasted with the outcomes of bariatric surgery, which, despite greater weight loss, has shown lower remission rates.
Historical Roots of Dietary Intervention in Diabetes
The concept of utilizing dietary restriction to combat diabetes is not a recent development. Over a century ago, fasting was recognized for its potential to halt the progression of diabetes and, in some instances, eliminate its symptoms within weeks. While extreme fasting, or starvation, is clearly detrimental to overall health and survival, these early observations laid the groundwork for understanding the link between caloric intake and diabetes management.
The historical understanding of type 2 diabetes often framed it as a disease of affluence and overconsumption. As far back as the early 20th century, it was recognized as a condition that disproportionately affected individuals whose lifestyles did not demand significant physical exertion and who had the means to consume more food than necessary. This perspective inherently suggested that the condition might be both preventable and treatable through a reduction in food intake.
This notion of "undereating" as a therapeutic approach can be traced back millennia. An ancient Ayurvedic text, dating back approximately 2,000 years, proposed a regimen for individuals with diabetes that included severe dietary restriction and extensive physical activity. While the methods described, such as living solely on cow dung and cow urine, are not medically viable by modern standards, they reflect a fundamental understanding of the need to reduce the body’s caloric load.
The Era of Extreme Dietary Regimens
In more recent historical contexts, albeit still predating the discovery of insulin, extreme dietary interventions were employed with varying degrees of success and significant discomfort for patients. The Rollo diet, proposed in 1797, exemplifies this. It was characterized by the consumption of rancid meat and the use of emetic drugs to induce vomiting, effectively reducing food intake through severe illness. While such methods did lead to a temporary reduction in diabetic symptoms, this was primarily due to the drastic decrease in food consumption rather than any inherent therapeutic quality of the prescribed substances. Rollo’s diet, which included unappetizing items like congealed blood and spoiled meat, certainly achieved its goal of limiting intake.
A more formalized approach emerged during the siege of Paris in the Franco-Prussian War. The period of scarcity and hardship led to observations that individuals with diabetes experienced improvements in their condition. This experience contributed to the widespread advice of "mangez le moins possible," or "eat as little as possible." This principle was further developed into the Allen starvation treatment, developed by Dr. Frederick M. Allen. The Allen treatment was considered a significant advancement in diabetes care before the advent of insulin, marking what is often referred to as "The Allen Era."
Dr. Allen’s work was influenced by clinical reports that noted the remission of severe diabetes in patients experiencing "wasting conditions" such as tuberculosis or cancer. He hypothesized that the severe caloric restriction associated with these illnesses might be the underlying factor. Through his research, Dr. Allen demonstrated that even in severe cases of diabetes, it was possible to clear sugar from the urine within ten days by severely restricting caloric intake. However, maintaining this remission proved challenging once patients resumed eating. His management strategy for diabetic patients centered on two core principles: maintaining an underweight status and restricting dietary fat. He observed that even moderate amounts of fat, such as butter or olive oil, could trigger a resurgence of diabetic symptoms in patients who had achieved temporary symptom relief.

Understanding Type 2 Diabetes as Fat Toxicity
Modern scientific understanding corroborates the historical emphasis on fat intake in the context of diabetes. Type 2 diabetes is increasingly understood as a condition stemming from "fat toxicity." Research has provided direct evidence of this phenomenon. When fat is infused intravenously into individuals, high-resolution MRI scans can visualize the rapid accumulation of fat within muscle cells within hours. This buildup is accompanied by a significant increase in insulin resistance. Similar effects have been observed in studies where individuals are placed on high-fat diets for just three days, and in some cases, even a single day or a single meal can acutely increase insulin resistance.
The physiological cascade is concerning: elevated dietary fat intake leads to increased insulin resistance in muscle tissue. When coupled with excessive calorie consumption, this can result in a buildup of fat in the liver. This hepatic fat accumulation, in turn, can lead to fat accumulation in the pancreas, the organ responsible for insulin production. Ultimately, this process can culminate in the development of full-blown type 2 diabetes.
Scientific consensus now suggests that type 2 diabetes can be understood as a state characterized by an excess of fat within the liver and pancreas. Crucially, for a significant period, at least up to 10 years from diagnosis, this condition is considered reversible in most individuals.
The Impact of Very Low-Calorie Diets
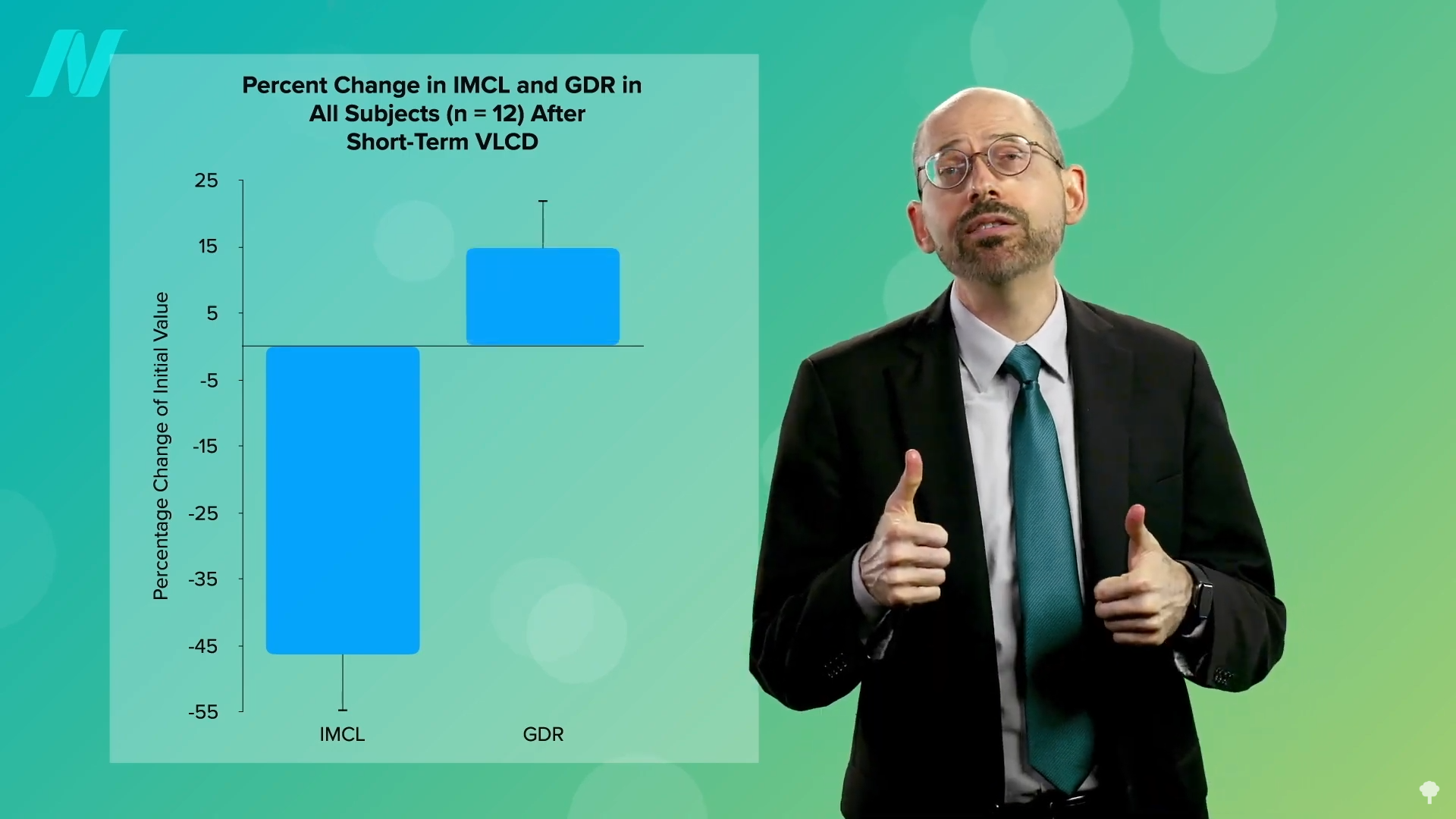
The effectiveness of severe caloric restriction in reversing insulin resistance and improving metabolic health has been demonstrated in clinical studies. When individuals are placed on very low-calorie diets, typically around 700 calories per day, a reduction in fat content within muscle cells is observed. This depletion of intramuscular fat is directly correlated with a corresponding improvement in insulin sensitivity.
This process also impacts fat accumulation in other organs. Studies have shown a substantial decrease in fat buildup within the liver of individuals adhering to such diets. If the dietary intervention is sustained, the excess fat in the pancreas also begins to reduce. This suggests that early intervention, particularly through significant weight loss, can lead to the reversal of type 2 diabetes, resulting in sustained healthy blood sugar levels through the adoption of a healthier long-term diet.
Weight Loss as a Primary Driver of Remission
The magnitude of weight loss appears to be a critical factor in achieving diabetes remission. As previously noted, losing 15% of body weight can lead to non-diabetic blood sugar levels in nearly 90% of individuals diagnosed with type 2 diabetes for less than four years. This remission rate significantly decreases in individuals who have lived with the disease for longer periods, with only about 50% achieving remission if the duration exceeds eight years.
This effectiveness of weight loss through dietary intervention is noteworthy when compared to surgical approaches. Bariatric surgery, which often results in more substantial weight loss, has demonstrated lower remission rates: 62% for those losing significant weight in the early stages and 26% for those with longer-standing diabetes. This data underscores the potential of dietary strategies, often referred to as "forks," to be more effective than surgical interventions, or "knives," in certain contexts.
Further research highlights that individuals diagnosed with type 2 diabetes for an average of three years can often reverse their condition after losing approximately 30 pounds. This significant weight loss is achievable through various dietary approaches, including structured fasting protocols.
Sustaining Remission: The Importance of Maintenance
While extended periods of physician-supervised, water-only fasting can induce remission, the long-term success hinges on sustained weight management. A critical understanding in diabetes management is that weight regain is directly associated with the recurrence of the disease. Therefore, achieving remission through initial weight loss is only the first step; maintaining a healthy weight through ongoing lifestyle changes is paramount.
The Evolution of Diabetes Treatment: From Insulin to Lifestyle
The discovery of insulin in 1921 was a monumental breakthrough, hailed as "medicine’s greatest miracle." For individuals with type 1 diabetes, insulin therapy proved to be life-saving, enabling them to manage their condition and prevent immediate fatal complications. However, the initial euphoria surrounding insulin gradually gave way to a more nuanced understanding of its limitations, particularly for type 2 diabetes.
While insulin could prevent immediate complications, it did not fully address the underlying issues that lead to long-term complications such as blindness, kidney failure, stroke, and amputations in people with type 2 diabetes. This realization led pioneers in diabetes care, such as Elliott Joslin, to advocate for the continued importance of non-pharmacological interventions. Joslin argued that self-discipline in diet and exercise, as emphasized in the pre-insulin era, should remain central to the management of type 2 diabetes.
Broader Implications and Future Directions
The growing body of evidence supporting the role of weight loss and dietary intervention in achieving type 2 diabetes remission has profound implications for public health. It suggests a paradigm shift in how the disease is approached, moving beyond solely managing symptoms with medication to addressing the root causes.
Key implications include:
- Preventive Strategies: Understanding type 2 diabetes as a condition exacerbated by lifestyle choices reinforces the importance of public health initiatives focused on promoting healthy eating and physical activity to prevent its onset.
- Treatment Protocols: The data supports the integration of comprehensive weight management programs, including dietary counseling and potentially structured fasting protocols under medical supervision, as first-line treatment options for early-stage type 2 diabetes.
- Patient Empowerment: Highlighting the reversibility of type 2 diabetes empowers individuals to take an active role in their health, fostering greater adherence to lifestyle changes.
- Economic Impact: Effective remission strategies could potentially reduce the long-term healthcare burden associated with managing chronic diabetes complications, including hospitalizations, medications, and treatments for associated conditions.
While fasting can be a powerful tool for initiating significant weight loss and improving metabolic markers, it is crucial to emphasize that it is not universally the optimal method for long-term weight management. Sustainable weight loss and the prevention of diabetes recurrence are best achieved through balanced, healthy dietary patterns and regular physical activity. Research into the "best diet for weight loss and disease prevention" continues to evolve, but the core principles of whole foods, balanced macronutrients, and portion control remain central.
The journey from understanding diabetes as an unyielding chronic disease to recognizing its potential for remission through lifestyle interventions has been long and marked by both historical trial and error and rigorous scientific inquiry. The current understanding, strongly supported by evidence, points towards significant weight loss as a cornerstone of achieving and maintaining remission for type 2 diabetes, offering a hopeful outlook for millions worldwide.






