The pursuit of significant weight loss has, throughout history, spurred the development and exploration of a wide array of methods, some conventional and evidence-based, others bordering on the extreme and ethically questionable. This article delves into the safety and efficacy of various weight-loss interventions, ranging from invasive surgical procedures and novel device-based therapies to historically discussed but ultimately ineffective or dangerous practices like corsetry and tapeworm ingestion. The landscape of weight management is often characterized by a desperate search for quick fixes, leading individuals to consider methods that carry substantial risks and questionable scientific backing.
The Caloric Equation: Exercise vs. Consumption
Understanding the fundamental principles of weight management is crucial when evaluating extreme methods. The energy balance equation—calories consumed versus calories expended—remains the cornerstone of weight regulation. For instance, a moderately obese individual engaging in moderately intense physical activity, such as cycling or brisk walking, can expect to burn approximately 350 calories per hour. However, the ease with which high-calorie, processed foods and beverages are consumed presents a significant challenge. These items can contain around 70 calories (293 kJ) per minute. This stark disparity means that a mere five minutes of consuming such calorie-dense items can negate an entire hour of dedicated exercise. This imbalance underscores why many individuals struggle to achieve sustainable weight loss through diet and exercise alone, paving the way for the exploration of more drastic interventions.
The AspireAssist Siphon System: A Mechanized Approach to Calorie Elimination
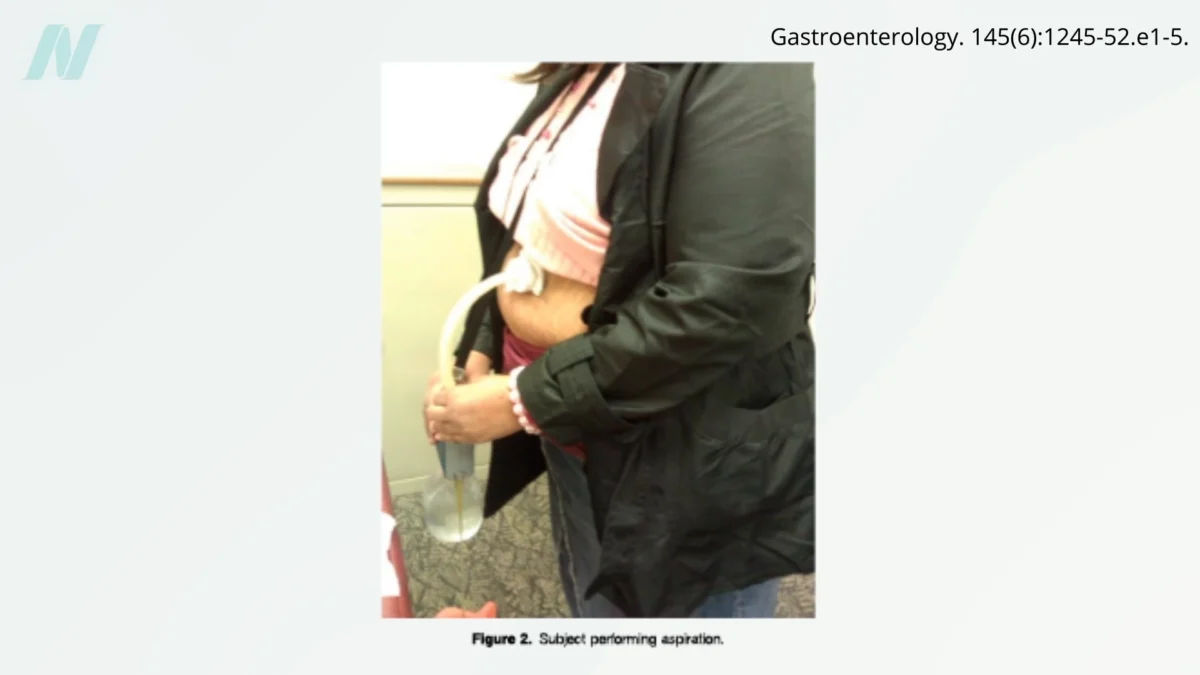
One of the more startling innovations in weight management is the AspireAssist siphon assembly. This device represents a technologically advanced, albeit invasive, approach to calorie reduction. The system involves a percutaneous gastrostomy, a procedure where surgeons create a surgical opening in the stomach and establish a fistula, or tunnel, through the abdominal wall. Once in place, the patient can attach a suction device to this opening after meals. This allows for the direct drainage of stomach contents, effectively removing a significant portion of ingested calories before they can be absorbed by the body.
The clinical implications of such a device are profound. It theoretically allows individuals to consume food, and then subsequently remove a substantial percentage of it, a concept colloquially described as "having your cake and eating it too." While patients utilizing the AspireAssist have demonstrated weight loss, the mechanisms are multifaceted. Beyond the direct caloric removal, the presence of the fistula may influence the stomach’s ability to relax during meals, potentially leading to earlier feelings of fullness. Furthermore, the protocol associated with the AspireAssist often necessitates the consumption of substantial amounts of water and thorough chewing of food. These practices, independently, can contribute to weight loss by promoting hydration and slowing the rate of food intake. A notable behavioral aspect observed in patients is a conscious effort to make healthier food choices, motivated by the visually unappealing nature of aspirating less healthy foods. Reports indicate that fried foods, in particular, present a visually unappealing substance when siphoned.
However, the AspireAssist is not without its medical considerations. Patients are required to supplement their diet with potassium, as it is lost through the gastric juices. Failure to do so can lead to potassium deficiency, a complication also seen in conditions like bulimia. While serious adverse events, such as abdominal abscesses, are reported as rare, minor wound complications are more common. A key selling point of the device is that it does not alter the fundamental anatomy of the gastrointestinal tract, a feature that, in the context of the evolving landscape of weight-loss procedures, is presented as a positive attribute.
The Duodenal-Jejunal Bypass Liner: A Less Invasive, Yet Risky, Alternative
Another intervention that seeks to limit calorie absorption without extensive surgical alteration is the duodenal-jejunal bypass liner, commonly known as EndoBarrier. This device, essentially a flexible plastic tube, is designed to line a portion of the intestinal walls. In concept, it mimics the effect of gastric bypass surgery, which typically involves removing or bypassing a section of the small intestine to reduce calorie absorption. The EndoBarrier is intended to be inserted non-surgically, but its anchoring mechanism presents significant challenges. The device is secured using ten barbed hooks, which can cause lacerations within the digestive tract. These lacerations are attributed to the majority of the adverse effects reported in studies, with a significant percentage of patients experiencing complications. Severe complications, including esophageal perforation and liver abscesses, though rarer, are still a notable concern, occurring in approximately 1 in 27 patients.
Intestinal "Resurfacing" and Other Invasive Procedures
The drive for novel weight-loss solutions has led to even more radical concepts, such as intestinal "resurfacing." This procedure involves thermally ablating the superficial duodenal mucosa, essentially burning off the intestinal lining. The rationale is to prevent nutrient absorption, but the invasive nature and potential for damage raise serious safety concerns.
Botulinum Toxin (Botox) Injections: An Unfulfilled Promise
In a less invasive, but ultimately unsuccessful, attempt to manage obesity, researchers have explored the use of Botulinum Toxin (Botox) injections into the stomach walls. The theory was that these injections would partially paralyze gastric muscles, thereby slowing stomach emptying and promoting a prolonged sense of fullness, leading to weight loss. However, clinical trials have shown this method to be ineffective in achieving significant and sustainable weight reduction.

Corsets and Tapeworms: Historical Remedies with Questionable Efficacy and Safety
The history of weight-loss strategies is replete with methods that, in retrospect, appear misguided or even dangerous. Corsets, once a staple of fashion, were also explored as a weight-loss tool. A study conducted in Sweden randomized individuals to wear corsets for extended periods daily over nine months. The results were largely negative, with participants finding the corsets uncomfortable and consequently failing to adhere to the protocol. This highlights a recurring theme: interventions that impose significant discomfort or require extreme lifestyle changes often fail due to poor compliance.
Even more concerning are the historical advertisements for "sanitized tapeworms" as a weight-loss remedy, dating back to the early 1900s. The idea was that ingesting a tapeworm would allow it to inhabit the digestive tract and consume food, thereby reducing the host’s calorie intake. The reality, however, is far more perilous. The discovery of living tapeworms during bariatric surgery procedures suggests that infesting oneself with parasites is not only ineffective but also poses serious health risks, potentially leading to malnutrition, organ damage, and other severe medical complications.
Psychological Approaches: Harnessing Disgust and Brain Stimulation
In a more contemporary and psychologically oriented approach, researchers have investigated the use of disgust as a mechanism to reduce the appeal of high-calorie foods. A study titled "Harnessing the Power of Disgust: A Randomized Trial to Reduce High-Calorie Food Appeal Through Implicit Priming" explored the impact of subliminal messaging. Participants were exposed to brief, positive images before viewing healthy food options and negative, unsettling imagery (such as cockroaches or vomit) before viewing high-calorie foods. The hypothesis was that these subliminal associations would create an aversion to unhealthy foods. While direct testing of food consumption was not conducted, subjects reported a reduced desire for high-calorie options, leading researchers to conclude that subliminal aversion could be a viable tactic against pervasive unhealthy food cues.
More extreme interventions have also delved into the realm of brain stimulation. Studies have explored the effects of repetitive electric brain stimulation on food intake. This involved drilling holes into the skulls of obese individuals and inserting electrodes into specific brain regions to observe their impact on hunger responses. The goal was to identify areas where stimulation could reduce appetite. While such techniques showed some promise in animal models (cats and monkeys), attempts to induce weight loss in obese humans through electrocoagulatory lesions in the brain proved unsuccessful and carried significant risks associated with invasive brain surgery.
The Global Perspective: International Observations of U.S. Weight-Loss Innovations
The unique and often unconventional approaches to weight management emerging from the United States have not gone unnoticed by the international medical community. Commentaries and academic papers have, at times, expressed bemusement at the array of American interventions. For example, a paper published in Obesity Surgery titled "What Are the Yanks Doing?" reviewed the U.S. experience with implantable gastric stimulation, a method involving electrodes placed in the stomach wall. When this proved ineffective, the focus shifted to colon electrical stimulation. These international observations highlight a broader, ongoing dialogue about the safety and efficacy of novel weight-loss strategies.
The Importance of Sustainable and Evidence-Based Approaches
The exploration of these diverse weight-loss methods, from the technologically advanced AspireAssist to the ethically dubious tapeworm ingestion, underscores a persistent human desire for rapid and effective solutions to obesity. However, the vast majority of these extreme interventions carry significant risks, ranging from surgical complications and nutrient deficiencies to severe psychological distress and potentially fatal outcomes.
The scientific consensus, as articulated in numerous public health guidelines and medical literature, emphasizes that sustainable and healthy weight loss is best achieved through a comprehensive approach that integrates a balanced, nutrient-dense diet, regular physical activity, and behavioral modifications. As highlighted in Dr. Greger’s book, How Not to Diet, the focus should be on long-term lifestyle changes rather than quick fixes. Borrowing from libraries or purchasing reputable books on nutrition and healthy living can provide individuals with the evidence-based knowledge needed to navigate the complex landscape of weight management.
Doctor’s Notes and Further Resources
For individuals seeking to understand the safety and efficacy of other weight-loss interventions, further information is available. The safety and effectiveness of gastric balloon surgery have been a subject of extensive research. Similarly, the efficacy and potential risks associated with weight-loss pills warrant careful consideration. Consulting with qualified healthcare professionals remains paramount for developing personalized and safe weight-loss strategies.
The journey towards a healthier weight is often challenging, but it is crucial to prioritize methods that are supported by robust scientific evidence and uphold the highest standards of patient safety. The allure of quick fixes and extreme interventions, while understandable, can often lead to detrimental health consequences, reinforcing the importance of evidence-based, sustainable approaches to weight management.






