Sham surgery trials have revealed a disturbing truth: some of the most commonly performed surgical procedures may offer little to no genuine benefit and, in some cases, carry significant risks. This revelation challenges long-held assumptions about surgical efficacy and raises critical questions about patient safety and the influence of the medical device industry.
The Rise and Fall, and Return, of the Intragastric Balloon
The intragastric balloon, a device designed to induce weight loss by occupying space in the stomach, first emerged in the 1980s. Marketed as a less invasive alternative to traditional bariatric surgery, these balloons were implanted into the stomach and then inflated with air or water. The premise was simple: by creating a feeling of fullness, the balloons would encourage reduced food intake and subsequent weight loss.
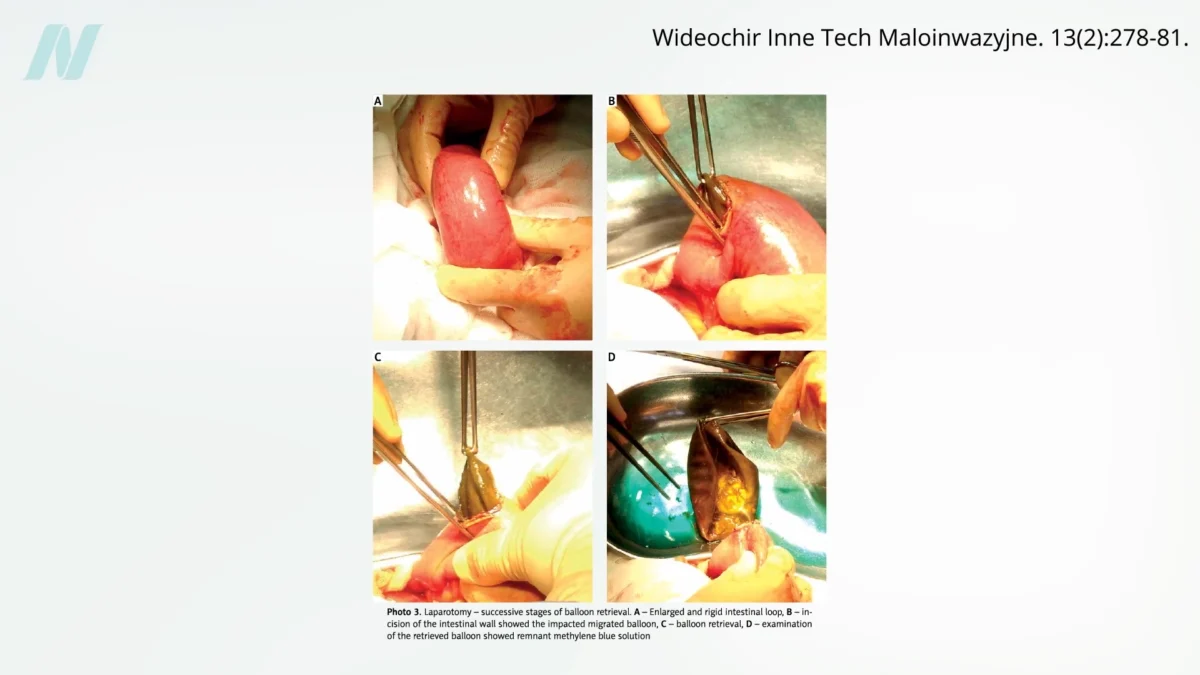
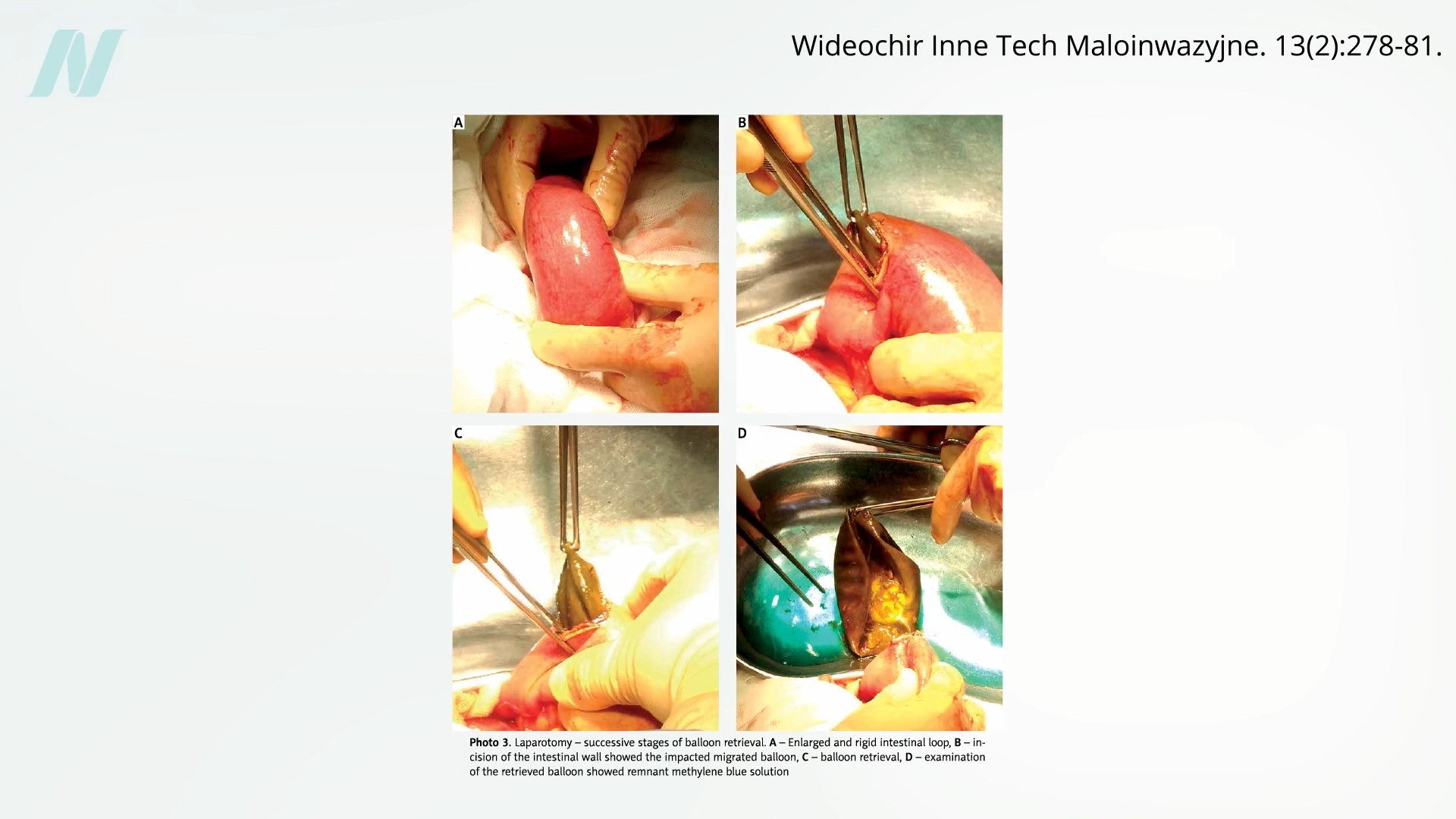
However, the introduction of medical devices into the market often outpaces rigorous evidence of their effectiveness and safety. The intragastric balloon was no exception. Early studies, including a significant investigation conducted at the Mayo Clinic, cast a shadow over the device’s promise. This research found that a staggering eight out of ten balloons spontaneously deflated. The implications of such deflation were dire, as a deflated balloon could migrate into the intestines, leading to potentially life-threatening bowel obstructions. Visual evidence, such as that presented in related video analyses, starkly illustrates the danger of a deflated balloon lodging within the digestive tract.
Even before deflation, the balloons posed considerable risks. The same Mayo Clinic study reported that half of the patients experienced gastric erosions, indicating damage to the stomach lining. More critically, when compared to simpler interventions like dietary changes and behavioral modification strategies, intragastric balloons failed to demonstrate superior weight-loss results. This lack of proven efficacy, coupled with the identified risks, ultimately led to the withdrawal of these early intragastric balloons from the market.
A Second Coming: New Balloons and Lingering Concerns
Despite the earlier setbacks, intragastric balloons made a comeback. After a hiatus of 33 years, the U.S. Food and Drug Administration (FDA) began approving a new generation of these devices in 2015. This renewed approval paved the way for the placement of over 5,000 devices in a relatively short period.
This resurgence coincided with the passage of the Sunshine Act, legislation designed to increase transparency in financial relationships between the healthcare industry and medical professionals. The act mandates the disclosure of payments made by drug companies and medical device manufacturers to physicians. While public awareness has grown regarding the financial ties between doctors and pharmaceutical giants, the extent to which surgeons receive payments from device companies for the implants they use has remained less understood. Reports have surfaced indicating that top physician recipients of industry payments can receive millions of dollars annually from device companies. Alarmingly, many of these physicians have historically failed to disclose these significant financial conflicts of interest when publishing research related to the devices they use.

While intragastric balloons offer the advantage of being reversible, unlike many forms of bariatric surgery, this reversibility does not equate to a lack of danger. The FDA has issued a series of advisories detailing the serious risks associated with these devices, including the potential for death. The mechanism of harm can be counterintuitive: a smooth, rounded object in the stomach can trigger severe nausea and vomiting. In extreme cases, persistent vomiting can lead to a rupture of the stomach, a potentially fatal complication. Indeed, nausea and vomiting are reported as "very common side effects," affecting the majority of patients. This persistent emesis can also contribute to life-threatening nutrient deficiencies, further underscoring the device’s adverse effects.
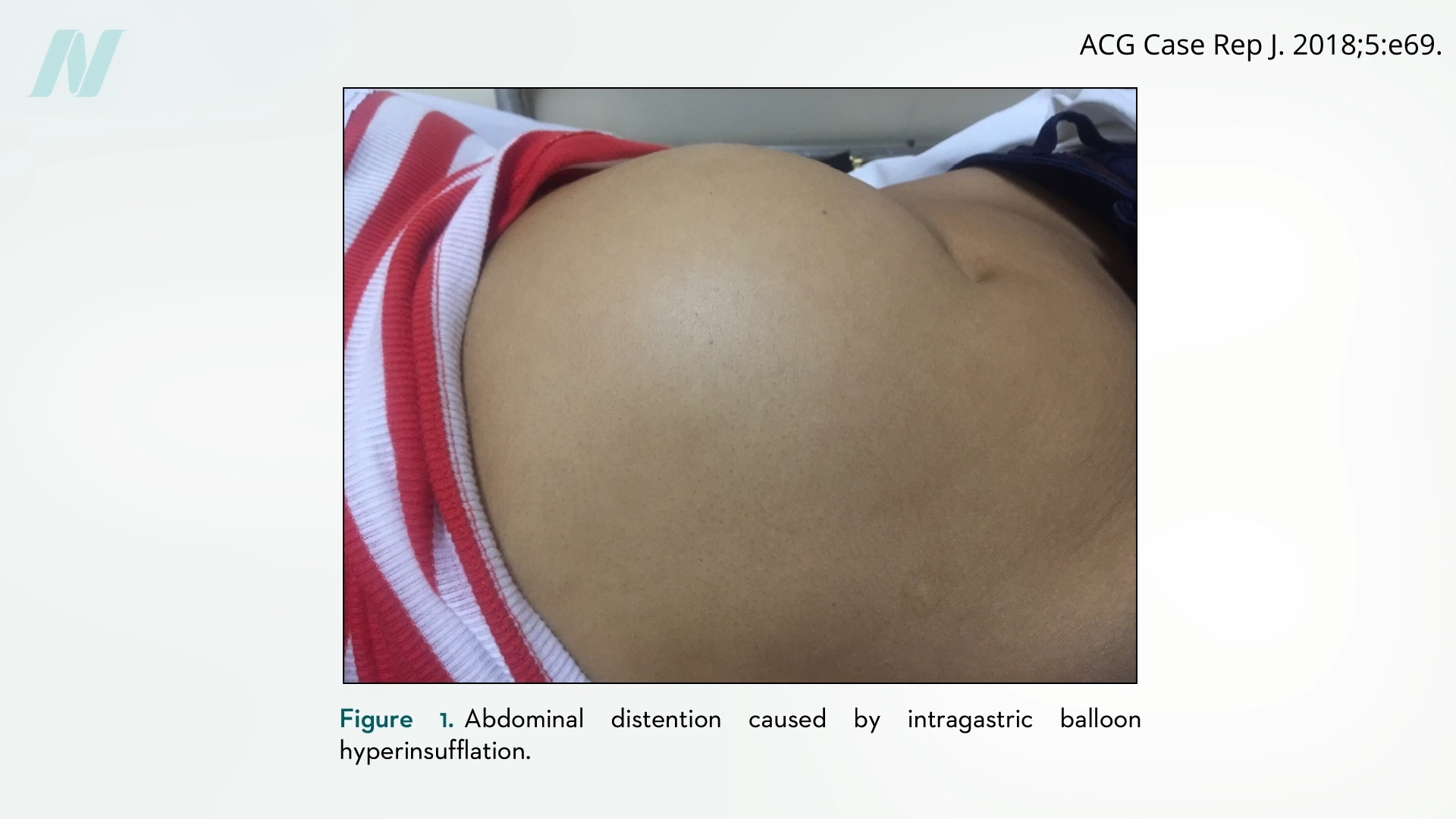
Complications are not solely limited to deflation. While bowel obstructions can occur due to deflation, other serious issues arise from the balloons inexplicably overinflating. This sudden overexpansion can lead to severe pain, vomiting, and abdominal distention, creating a perilous situation for the patient.
Echoes of Other Medical Devices: The Breast Implant Parallel
The phenomenon of unexpected device behavior, such as spontaneous overinflation, has parallels in other medical implants. Breast implants, for instance, have been documented to undergo "spontaneous autoinflation," leading to an average increase in breast volume of over 50%. This poorly understood and underreported occurrence highlights a broader challenge in medical device safety: the unpredictability of implanted materials within the human body. Intriguingly, early experimental intragastric balloons were reportedly developed using technology originally intended for breast implants, suggesting a cross-pollination of concepts that may have overlooked critical safety considerations.
The Power of the Placebo: Sham Surgery as a Gold Standard
The ethical debate surrounding the effectiveness of medical interventions, particularly surgical procedures, is often complicated by the placebo effect. In drug trials, it is standard practice to compare the active medication against a placebo (like a sugar pill) to isolate the drug’s true impact. However, replicating this in surgery presents a unique challenge. How does one ethically control for the powerful psychological and physiological effects of undergoing a procedure, even one that is ostensibly ineffective?
The answer, as demonstrated in groundbreaking research, lies in sham surgery. This methodology involves performing a surgical procedure that mimics the actual surgery in every way, including incisions and the manipulation of tissues, but without performing the therapeutic intervention itself. Patients are then randomized to receive either the actual surgery or the sham procedure.
The Knee Surgery Revelation: A Landmark Study
In 2002, The New England Journal of Medicine published a seminal study that subjected arthroscopic knee surgery, one of the most frequently performed orthopedic procedures, to the rigor of sham surgery. Billions of dollars are spent annually on arthroscopic interventions for osteoarthritis and knee injuries, involving the insertion of scopes into knee joints and the removal of damaged tissue. The study sought to determine if these procedures offered a genuine benefit beyond the placebo effect.
Knee pain patients were randomly assigned to undergo either actual arthroscopic surgery or a sham procedure. In the sham group, surgeons made incisions and simulated the surgical steps, even splashing saline onto the joint, but did not perform any actual tissue debridement or repair. The findings of this trial ignited a firestorm of controversy within the medical community.
The results were stark: while patients who received the actual surgery did experience improvement, so did the control group who underwent the sham procedure. This indicated that the perceived benefits of arthroscopic knee surgery were largely attributable to the placebo effect, with the surgical intervention itself offering no additional therapeutic value. The study’s methodology drew sharp criticism from professional medical associations, who questioned the ethics of subjecting patients to fake surgery and the judgment of patients who consented to participate. Despite the ethical outcry, the data from the knee surgery trial provided compelling evidence that a significant portion of commonly performed surgeries might be ineffective.
A Crisis of Confidence in Rotator Cuff Surgery
The implications of the sham surgery findings extend beyond knee procedures. Currently, rotator cuff shoulder surgery is facing a similar crisis of confidence, with researchers investigating its efficacy through sham-controlled trials. The results of these trials are anticipated to shed further light on whether the perceived benefits of these interventions are truly rooted in surgical intervention or are primarily driven by the placebo response.
Re-evaluating the Intragastric Balloon: Sham Trials and Weight Loss
When intragastric balloons were subjected to sham-controlled trials, the results mirrored the findings in orthopedic surgery. These trials revealed that both older and newer iterations of the devices frequently failed to provide any meaningful weight-loss benefit. Even in instances where some weight loss was observed, it was often temporary. This is partly because balloons are typically recommended for use only for six months, after which the risk of deflation increases significantly. Attempts to extend the duration of balloon use or to repeatedly insert new balloons have also failed to demonstrate improved long-term weight outcomes. Sham-controlled trials have indicated that any initial effects on appetite and satiety may dissipate over time as the body adapts.
The Broader Implications: "Fake News" in Medicine
The findings from sham surgery trials compel a critical re-evaluation of established medical practices. The medical profession often prides itself on its scientific rigor, rightfully condemning movements that reject established scientific consensus, such as the anti-vaccination movement. However, when confronted with evidence that some widely performed and accepted surgical procedures are not only ineffective but may even exacerbate patient conditions – for example, by increasing the likelihood of needing a total knee replacement – it becomes difficult to deny that the medical field is susceptible to its own forms of "fake news" and "alternative facts."
The implications are profound. Patients undergoing surgery are often making significant decisions based on the assumption of proven efficacy. The financial stakes are also enormous, with billions of dollars invested annually in surgical devices and procedures. The continued promotion and performance of procedures that lack robust evidence of benefit, and may even carry risks, raises serious questions about accountability, transparency, and the prioritization of patient well-being over financial interests.
The Path Forward: Rigorous Evidence and Patient Empowerment
The insights gleaned from sham surgery trials underscore the paramount importance of evidence-based medicine. It is imperative that all medical interventions, particularly surgical ones, undergo rigorous testing through well-designed, independent trials, including sham-controlled studies where ethically feasible. This includes a critical examination of the role of the medical device industry and its potential influence on research and clinical practice.
The Sunshine Act represents a crucial step towards greater transparency, but its implementation and enforcement must be robust. Patients, too, have a vital role to play in this process. By becoming informed consumers of healthcare, understanding the evidence behind recommended treatments, and engaging in open dialogue with their physicians about risks and benefits, patients can empower themselves to make the best possible decisions for their health.
The future of surgical practice must be built on a foundation of irrefutable evidence, ensuring that procedures offered to patients are not merely traditions or market-driven offerings, but are demonstrably safe and effective interventions that genuinely improve health outcomes. The lessons learned from sham surgery trials serve as a critical reminder that in medicine, as in all scientific endeavors, a commitment to truth, however uncomfortable, is essential.
Doctor’s Note
This article is part of a two-part series. The subsequent installment, "Extreme Weight-Loss Devices," will delve further into the efficacy and safety of other popular weight-loss interventions. For comprehensive information on bariatric surgery and related topics, readers are encouraged to explore further resources and relevant posts.
The book "How Not to Diet" by Dr. Michael Greger focuses on sustainable weight loss strategies and is available through libraries and booksellers. All proceeds from his books are donated to charity.






