The landscape of bariatric weight-loss surgery, while offering a powerful tool for individuals struggling with severe obesity, is not without its inherent risks. Emerging research and clinical observations underscore a critical factor that significantly influences patient outcomes: the skill and experience of the performing surgeon. Beyond the well-documented risks associated with any major surgical procedure, a growing body of evidence suggests that the technical proficiency of the bariatric surgeon plays a pivotal role in determining the likelihood of complications, reoperations, and even mortality.
The Shadow of Reoperation: A Common Consequence
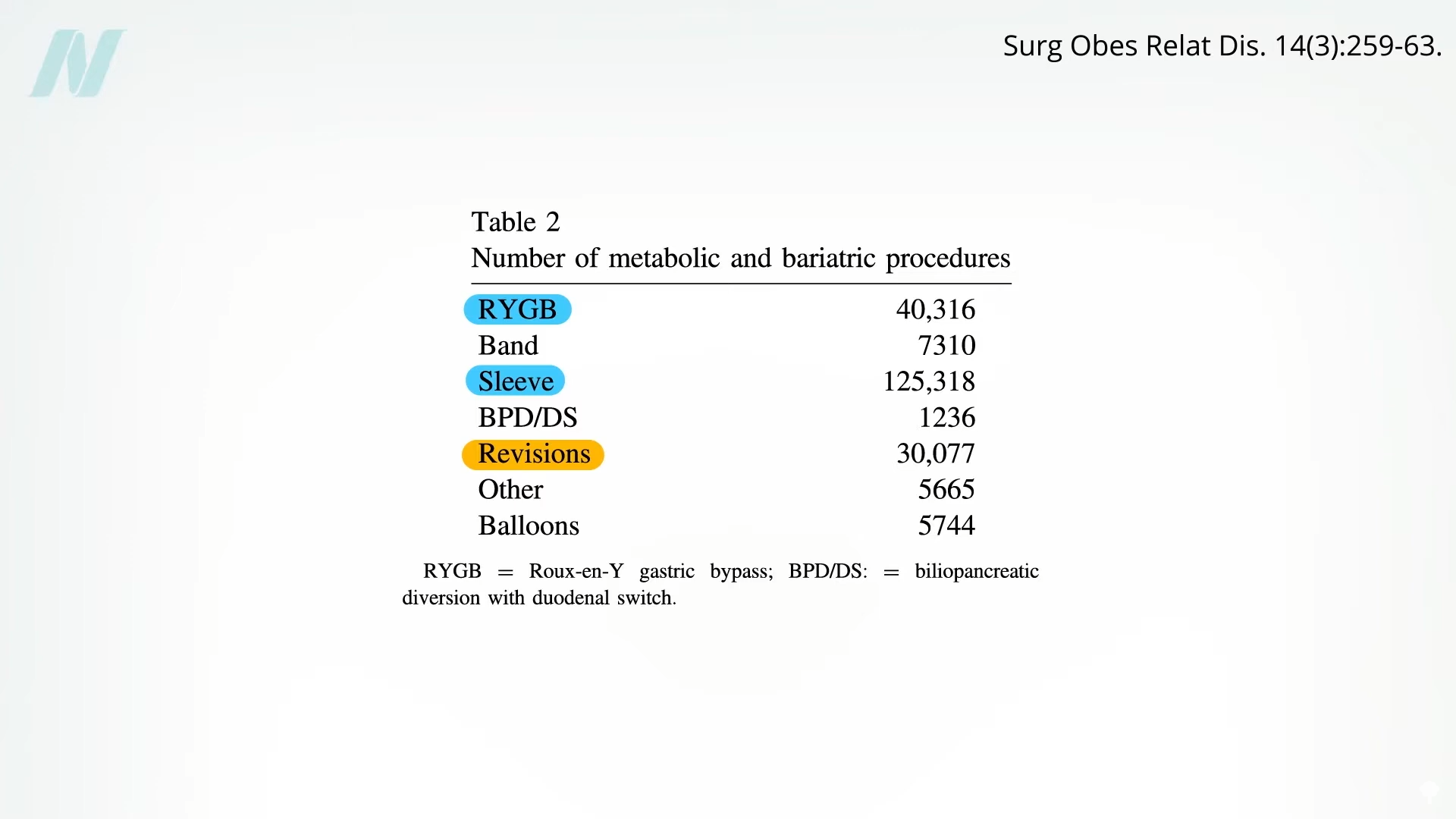
The complexity of bariatric procedures means that complications are an unfortunate reality for a significant portion of patients. Following the most common bariatric interventions, sleeve gastrectomy and Roux-en-Y gastric bypass, the third most frequent surgical procedure undertaken is a revision to address issues arising from a prior bariatric operation. This statistic, highlighted by a review of surgical data, points to a substantial subset of patients who require further surgical intervention.
Data indicates that up to 25% of individuals who undergo bariatric surgery may need to return to the operating room due to complications stemming from their initial procedure. The implications of these subsequent surgeries are particularly concerning. Reoperations carry a significantly higher risk profile, with mortality rates potentially as much as ten times greater than those of primary bariatric surgeries. Furthermore, there is "no guarantee of success" in these revision procedures, meaning that even after enduring the risks of a second surgery, positive outcomes are not assured.
The spectrum of complications that necessitate these reoperations is broad and can include life-threatening issues such as leaks from surgical staple lines, the formation of abnormal connections between organs (fistulas), the development of internal sores (ulcers), narrowing of the digestive tract (strictures), erosion of surgical materials, blockages in the digestive system (obstructions), and severe acid reflux. These complications can lead to prolonged hospital stays, significant pain and suffering, and a substantial impact on a patient’s quality of life.
Surgeon Skill: A Decisive Variable in Patient Safety
The critical role of surgeon expertise in mitigating these risks has become increasingly apparent. A landmark study, published in the prestigious New England Journal of Medicine, provided compelling evidence of this correlation. In this study, bariatric surgeons voluntarily submitted video recordings of their surgical procedures for blind evaluation by a panel of their peers. The objective was to assess technical proficiency.
The findings were stark. The study revealed a wide variation in the technical skills demonstrated by the participating surgeons. Crucially, this variability in skill was directly linked to patient outcomes. Surgeons with lower technical proficiency were associated with significantly higher rates of complications, hospital readmissions, the need for reoperations, and even mortality. Patients treated by less competent surgeons experienced nearly three times the rate of complications and five times the rate of death compared to those operated on by more skilled surgeons.

This suggests that, much like in other performance-based professions such as music or athletics, some surgeons may possess a natural aptitude for surgical precision and dexterity. However, the study also emphasizes the importance of practice and experience in refining surgical technique.
The Learning Curve: Mastering the Art of Bariatric Surgery
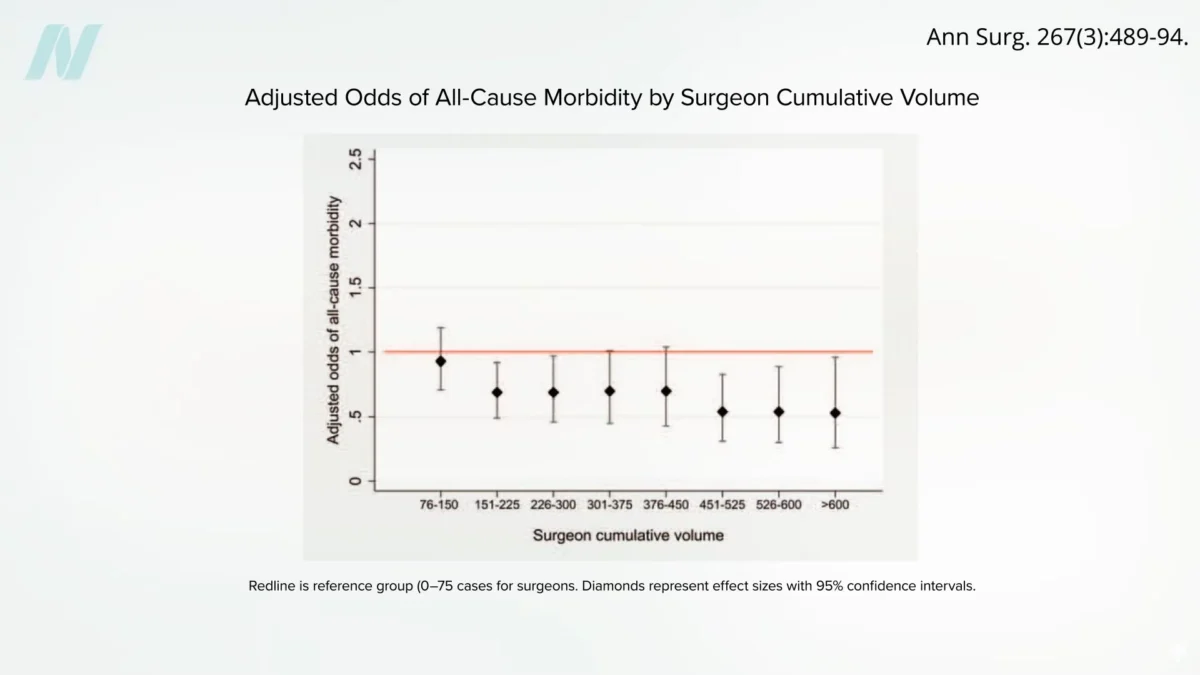
The complexity of bariatric procedures, particularly the gastric bypass, means that a substantial learning curve is inherent in developing surgical mastery. It is estimated that a surgeon may need to perform approximately 500 cases to achieve a proficient understanding and execution of the procedure. The risk of complications appears to stabilize and begin to decrease after a surgeon has completed around 500 procedures.
Further analysis of surgical data indicates that surgeons who have performed more than 600 gastric bypass procedures exhibit the lowest rates of complications. This contrasts sharply with the outcomes seen in less experienced surgeons. The data suggests that the odds of a fatal outcome may be double for patients operated on by surgeons who have performed fewer than 75 procedures compared to those who have performed more than 450. This statistical disparity underscores the profound impact of accumulated experience on patient safety.
Navigating the Surgical Landscape: Recommendations for Patients
Given the significant influence of surgeon skill on patient outcomes, individuals considering bariatric surgery are strongly advised to undertake thorough due diligence. A crucial step is to inquire directly with potential surgeons about the volume of bariatric procedures they have performed. Understanding a surgeon’s experience level can provide valuable insight into their potential proficiency.
Furthermore, choosing an accredited bariatric "Center of Excellence" is highly recommended. These centers typically adhere to rigorous standards of care, patient safety protocols, and surgeon credentialing. Studies have indicated that surgical mortality rates at accredited Centers of Excellence are two to three times lower than those at non-accredited institutions. This accreditation signifies a commitment to high-quality surgical care and a track record of positive patient outcomes.
Beyond the Surgeon’s Hand: Patient Responsibility and Long-Term Care
While surgeon skill is a paramount factor, it is important to acknowledge that not all complications are solely attributable to surgical technique. Patient behavior and adherence to post-operative guidelines also play a significant role in successful recovery.
One illustrative case, described in a report titled "The Dangers of Broccoli," highlights the importance of diligent post-operative care. A surgeon recounted the experience of a woman who, three months after a gastric bypass, attended an all-you-can-eat buffet. While she consumed healthy foods, she reportedly neglected to chew them adequately. The undigested food caused her surgical staples to rupture, leading to an emergency room visit and a subsequent operation. Upon examination, her abdominal cavity contained "full chunks of broccoli, whole lima beans, and other green leafy vegetables." This cautionary tale, while extreme, underscores the critical need for patients to meticulously follow dietary instructions, particularly regarding the thorough mastication of food, to prevent potentially catastrophic complications.

The Lifelong Commitment: Nutritional Deficiencies and Malabsorption
Even in cases where the surgical procedure itself is performed flawlessly, bariatric surgery necessitates a lifelong commitment to nutritional replacement and vigilant monitoring. The altered anatomy of the digestive system, particularly after procedures like gastric bypass, leads to malabsorption of essential vitamins and minerals. This is an intentional consequence of procedures designed to reduce calorie absorption by bypassing segments of the intestines.
The consequences of these deficiencies extend far beyond common ailments like anemia, osteoporosis, or hair loss. Severe deficiencies can manifest as life-threatening conditions such as beriberi (thiamine deficiency), pellagra (niacin deficiency), kwashiorkor (protein deficiency), and debilitating nerve damage. Copper deficiency, for instance, can lead to vision loss years or even decades after surgery. Tragically, in reported cases of severe thiamine deficiency, nearly one in three patients have experienced permanent brain damage before the condition was identified and treated.
Even restrictive procedures, such as stomach stapling, can put patients at risk for severe nutrient deficiencies due to persistent vomiting. This vomiting, reported by up to 60% of patients after bariatric surgery, is often attributed to "inappropriate eating behaviors" – essentially, attempting to eat in a manner that the altered digestive system cannot tolerate. While vomiting contributes to weight loss, it can also exacerbate malabsorptive issues.
Dumping Syndrome: A Designed Deterrent
Another common post-operative phenomenon is "dumping syndrome." This occurs when food, particularly calorie-rich items, bypasses the stomach and moves too quickly into the intestines, triggering a range of uncomfortable symptoms. These can include abdominal pain, diarrhea, nausea, bloating, fatigue, and palpitations. Surgeons often view dumping syndrome not as a complication, but as an intentional feature of gastric bypass surgery. It serves as a powerful behavioral modification tool, deterring patients from consuming energy-dense foods by making them physically ill. This mechanism is conceptually similar to how certain medications are used to create an aversive response to substance use.
Broader Implications and Future Directions
The findings regarding surgeon skill and experience highlight a critical area for ongoing research and clinical practice improvement. As bariatric surgery continues to be a significant intervention for obesity management, ensuring patient safety must remain the highest priority. This includes developing standardized methods for assessing surgical skill, implementing robust training programs that emphasize the learning curve, and promoting transparency in reporting surgeon and institutional outcomes.
The series of articles, of which this is the second installment, aims to provide a comprehensive overview of bariatric surgery. The preceding article, "The Mortality Rate of Bariatric Weight-Loss Surgery," likely delved into the general risks associated with these procedures. Future discussions are slated to explore the efficacy of bariatric surgery in reversing diabetes and the long-term sustainability of weight loss achieved through these interventions.
For individuals seeking to achieve sustainable weight loss without surgical intervention, comprehensive resources like the book "How Not to Diet" offer evidence-based strategies. The emphasis on understanding the multifaceted aspects of weight management, including the physiological and psychological components, is crucial for long-term health and well-being. The ongoing dialogue surrounding bariatric surgery must continue to balance the potential benefits against the inherent risks, with a steadfast focus on patient education, surgeon accountability, and continuous improvement in surgical standards of care.






