Sham surgery trials, once a controversial yet essential tool for rigorously evaluating medical procedures, have exposed a disquieting truth: some of the most widely adopted surgical interventions may offer little to no genuine benefit, and in some cases, can even pose significant risks. This revelation casts a long shadow over established medical practices, prompting a critical re-examination of how surgical devices and procedures are vetted and implemented in clinical settings.
The Rise and Fall of the Intragastric Balloon: A Cautionary Tale
The 1980s heralded the arrival of intragastric balloons with considerable fanfare. These devices, designed to be inserted into the stomach and inflated with air or water, promised to create a sense of fullness, thereby aiding in weight loss. The allure of a less invasive approach to combating obesity was undeniable, and the medical community embraced the concept with optimism. However, the history of medical devices is unfortunately replete with instances where innovation outpaced evidence, with products reaching the market before robust data on their efficacy and safety could be established. The intragastric balloon proved to be no exception.
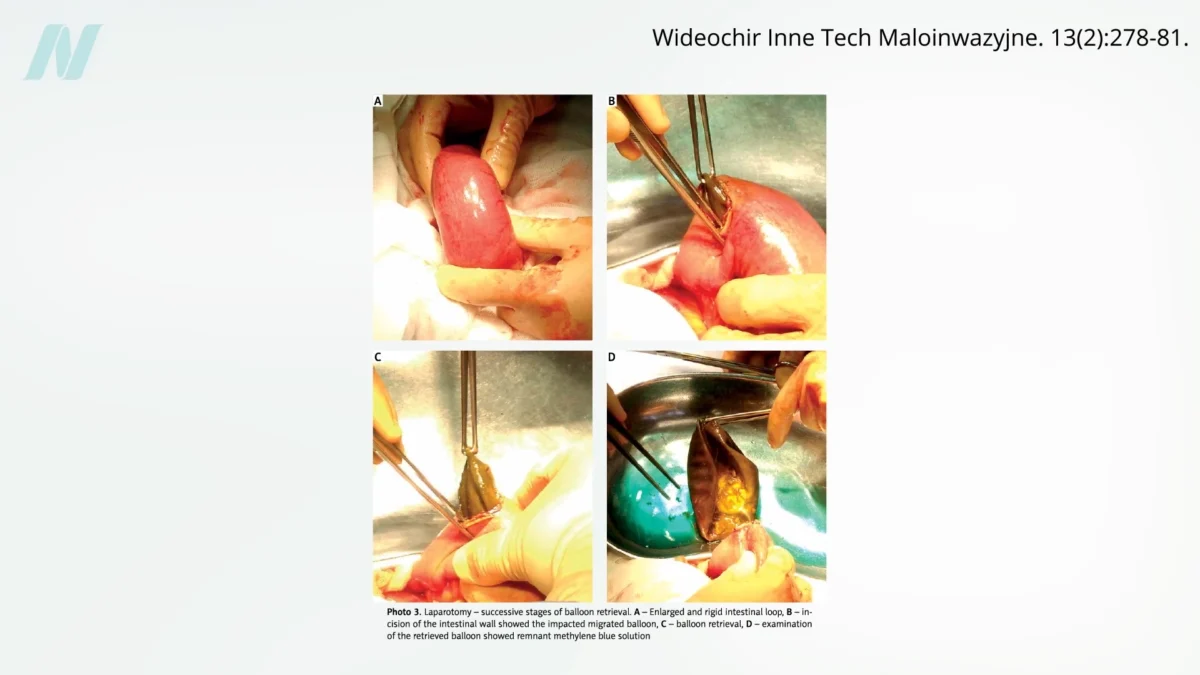
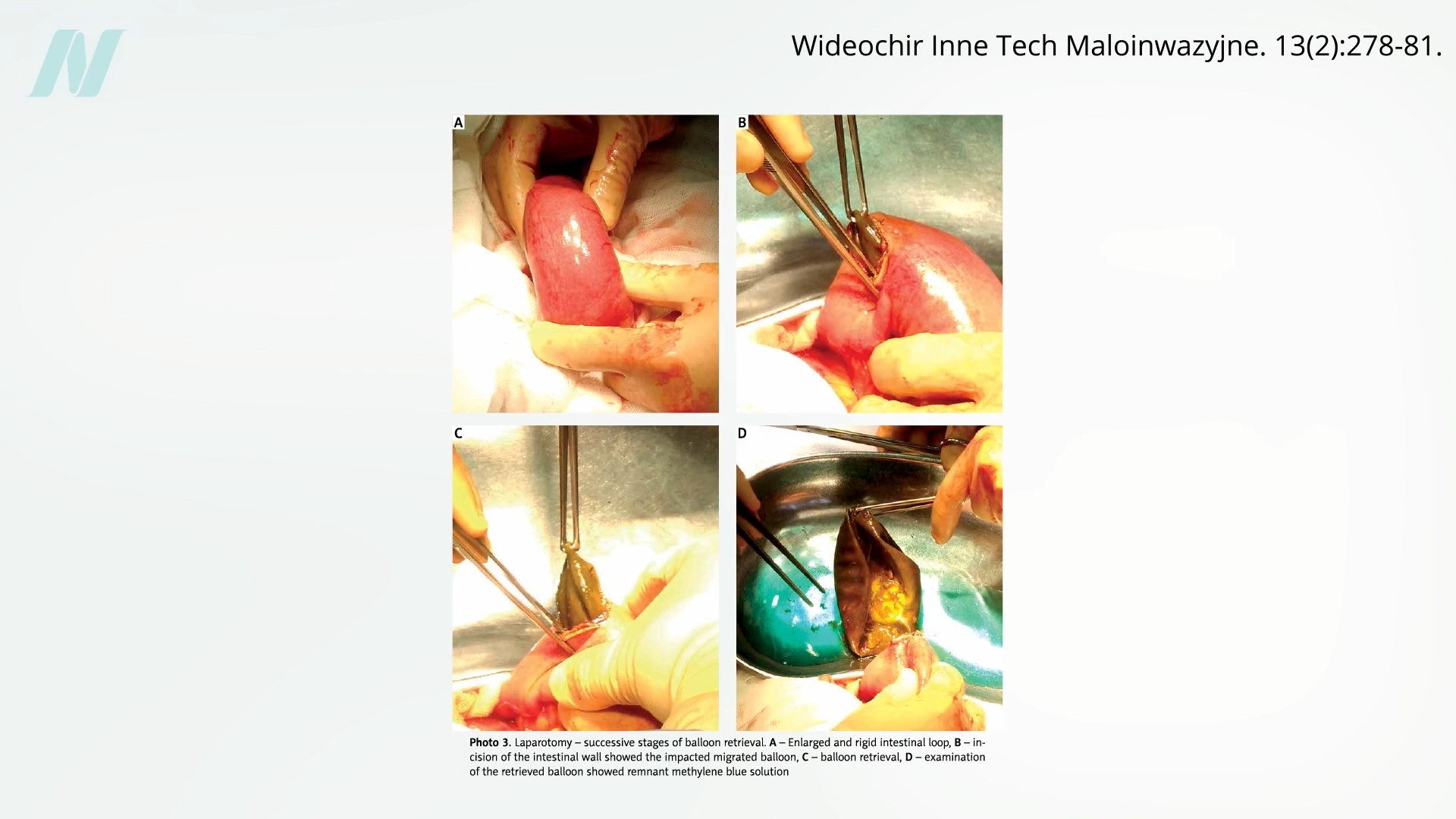
Early investigations into the effectiveness of these devices quickly began to surface. A pivotal study conducted at the Mayo Clinic delivered a significant blow to the burgeoning “gastric bubble” trend. The findings revealed a startlingly high failure rate, with a staggering 8 out of 10 balloons spontaneously deflating. This spontaneous deflation presented a grave danger: the deflated balloon could migrate into the intestines, leading to a potentially life-threatening bowel obstruction. Visual evidence, often presented in accompanying medical literature and video demonstrations, starkly illustrated the physical consequences of such blockages.
Beyond the risk of obstruction, the intragastric balloons were also implicated in causing significant gastric distress even before any deflation occurred. In approximately half of the patients studied, the balloons led to gastric erosions, damaging the delicate lining of the stomach. More critically, when compared to conservative weight management strategies such as dietary changes and behavioral modification, the balloons failed to demonstrate superior efficacy in inducing sustainable weight loss. The cumulative evidence of risks and limited benefits ultimately led to the withdrawal of these early intragastric balloon systems from the market.

The Return of the Balloon: New Devices, Enduring Concerns
Following a hiatus of over three decades, intragastric balloons made a resurgence in the United States. In 2015, the U.S. Food and Drug Administration (FDA) began approving a new generation of these devices. Within a short period, more than 5,000 of these newer models were implanted in patients. This reintroduction coincided with the passage of the Sunshine Act, a landmark piece of legislation designed to bring transparency to financial relationships between the healthcare industry and medical professionals. The Act mandates the disclosure of payments made by pharmaceutical companies and medical device manufacturers to physicians, aiming to illuminate potential conflicts of interest.
While public awareness has grown regarding the financial ties between doctors and "Big Pharma," the extent to which surgeons benefit financially from the sale and use of medical devices may be less widely understood. Data has emerged showing substantial financial flows from device companies to physicians. In one notable period, the top 100 physician recipients of industry payments received an astounding $12 million from device manufacturers in a single year. Alarmingly, a significant minority of these physicians, when publishing research related to these devices, failed to disclose these clear financial conflicts of interest, raising serious questions about the impartiality of their findings.
While intragastric balloons offer a theoretical advantage over more permanent bariatric surgeries in that they are reversible, this reversibility does not render them benign. The FDA has issued a series of advisories highlighting the potential risks associated with these devices, some of which can be fatal. The mechanism of stomach perforation, for instance, can be indirect. A smooth, rounded object within the stomach can trigger severe and persistent vomiting, leading to a rupture of the stomach wall, a catastrophic complication. Nausea and vomiting are indeed very common side effects, affecting a majority of patients who have these balloons implanted. The persistent nature of this vomiting can also contribute to life-threatening nutrient deficiencies following balloon placement.
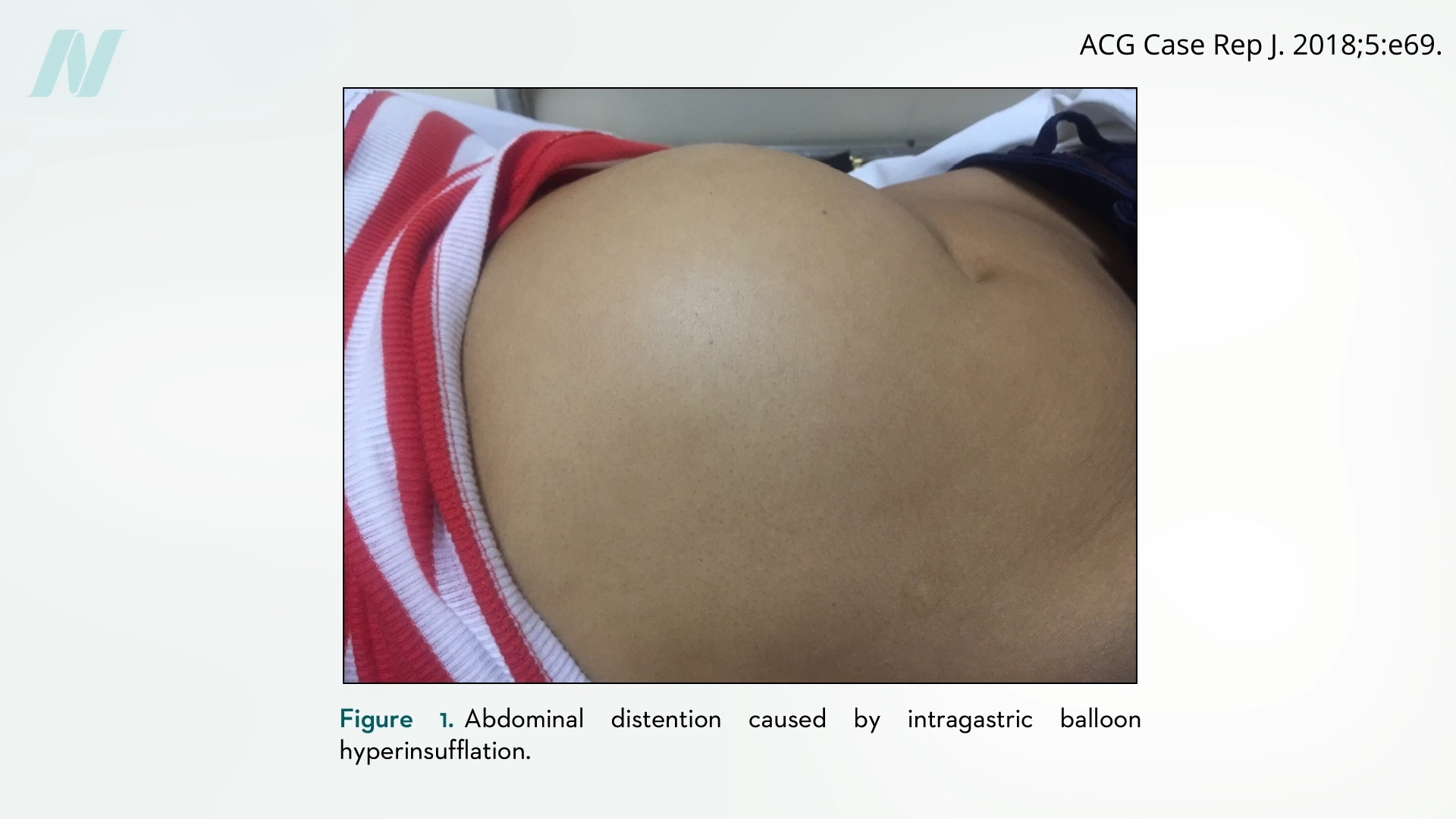
Complications can arise from various mechanisms. Some, like bowel obstruction, are directly linked to the deflation of the balloon. Others, however, stem from unexpected overinflation. In these instances, the balloon can expand excessively, leading to intense pain, vomiting, and significant abdominal distention. This phenomenon of spontaneous overinflation bears a striking resemblance to issues previously observed with other implantable medical devices.
Parallels with Breast Implants: A Pattern of Unforeseen Complications
The phenomenon of medical implants unexpectedly increasing in size or volume was first documented in the context of breast implants. Reports detailed cases of "spontaneous autoinflation," where implants would inexplicably grow, leading to an average increase in breast volume exceeding 50%. This remains an underreported and poorly understood phenomenon within the medical community. Intriguingly, early experimental intragastric balloons were themselves developed using materials and designs initially tested for breast implants, suggesting a shared history of unforeseen complications.
The Role of Sham Surgery in Unveiling Truths
The core of the debate surrounding the efficacy of any medical intervention, including surgical procedures, lies in balancing risks against benefits. Industry-sponsored trials often highlight "notable weight loss," but it can be challenging to isolate the specific contribution of the device itself from the concurrent "supervised diet and lifestyle changes" that are integral to these studies. In pharmaceutical trials, the use of placebo pills allows for a clear comparison. However, in surgical trials, the psychological impact of undergoing a procedure, known as the placebo effect, complicates direct comparisons. This is where the controversial yet powerful methodology of sham surgery becomes indispensable.
In 2002, a groundbreaking and ethically charged study was published in The New England Journal of Medicine. This research subjected arthroscopic surgery of the knee, the most common orthopedic procedure, to rigorous scrutiny. Billions of dollars are invested annually in arthroscopic interventions for osteoarthritis and knee injuries, involving the insertion of scopes and removal of damaged tissue. However, the effectiveness of these procedures had largely gone unchallenged by direct comparison to non-interventional controls.
The study’s design involved randomizing patients suffering from knee pain into two groups: one receiving the actual arthroscopic surgery, and the other undergoing a sham procedure. In the sham surgery, surgeons would make incisions in the patients’ knees and simulate the surgical steps, including splashing saline, without actually performing any therapeutic intervention on the joint.
This study ignited a firestorm of controversy within the medical profession. Ethical questions were raised regarding the morality of subjecting patients to incisions for a fake surgery. Professional medical associations publicly questioned the ethics of the surgeons involved and the perceived "sanity" of patients who consented to participate. The results, however, were illuminating. While patients who received the actual surgery experienced improvement, an equivalent number of patients in the sham surgery group also reported significant relief from their knee pain. This stark finding suggested that a substantial portion of the perceived benefit from arthroscopic knee surgery might be attributable to the placebo effect and the natural course of healing, rather than the surgical intervention itself. The implications were profound: for many patients, the surgery had no demonstrable therapeutic effect.
This crisis of confidence has since extended to other common surgical procedures. Rotator cuff shoulder surgery, for instance, is currently facing similar questions regarding its true effectiveness beyond the placebo response.
Re-evaluating Weight-Loss Devices: Evidence vs. Industry Claims
When intragastric balloons were subjected to sham-controlled trials, the results mirrored the earlier findings. Both older and newer iterations of the devices often failed to demonstrate any significant weight-loss benefit when compared to sham procedures. Even in cases where some weight loss was observed, it was frequently temporary. This transience is partly explained by the prescribed duration of balloon placement, typically limited to six months, after which the risk of deflation becomes unacceptably high. Attempts to extend the use of balloons or to replace them with new ones have not yielded improved long-term weight outcomes. Sham-controlled trials have indicated that any initial effects of balloons on appetite and satiety may diminish over time as the body adapts.
The Broader Implications: A Call for Scientific Integrity
The insights gleaned from sham surgery trials underscore a critical issue: the potential for popular surgical procedures to be ineffective, or even detrimental. While the medical community rightly champions scientific rigor and decries the spread of misinformation, such as the anti-vaccination movement, the findings from these surgical studies suggest that the healthcare system itself is not immune to the proliferation of "fake news" and "alternative facts." When well-established and frequently performed surgeries are found to be largely ineffective, or worse, to increase the risk of needing more invasive interventions (such as progressing to total knee replacement after ineffective arthroscopic surgery), it calls into question the very foundations of evidence-based practice.
The implications of these findings are far-reaching. They necessitate a renewed commitment to independent, rigorous research that prioritizes patient well-being over commercial interests. Transparency in reporting financial conflicts of interest is paramount, as is the ethical imperative for physicians to critically evaluate the evidence supporting the procedures they perform. Patients, in turn, deserve clear, unbiased information to make informed decisions about their healthcare, free from the influence of potentially misleading marketing or undisclosed financial incentives. The lessons from sham surgery trials serve as a vital reminder that scientific inquiry must remain a constant, self-correcting process, even when it challenges deeply entrenched practices and beliefs.
Doctor’s Note:
This exploration of questionable medical interventions is part of a larger discussion on effective health strategies. The subsequent article in this series, "Extreme Weight-Loss Devices," will delve further into the landscape of weight management technologies. For a comprehensive understanding of bariatric surgery and its alternatives, readers are encouraged to explore related posts and consult additional resources. My book, How Not to Diet, offers a detailed approach to sustainable weight loss, available through libraries and booksellers, with all proceeds dedicated to charitable causes.






