The landscape of bariatric weight-loss surgery, while offering a path to significant health improvements for many, is underscored by inherent risks that appear to be directly correlated with the proficiency of the surgical practitioner. Data emerging from comprehensive studies and clinical observations reveals a complex interplay between surgical technique, patient outcomes, and the potential for severe complications. This analysis delves into the critical role of surgeon expertise in mitigating these risks and ensuring patient safety.
The Growing Prevalence and Complexities of Bariatric Procedures
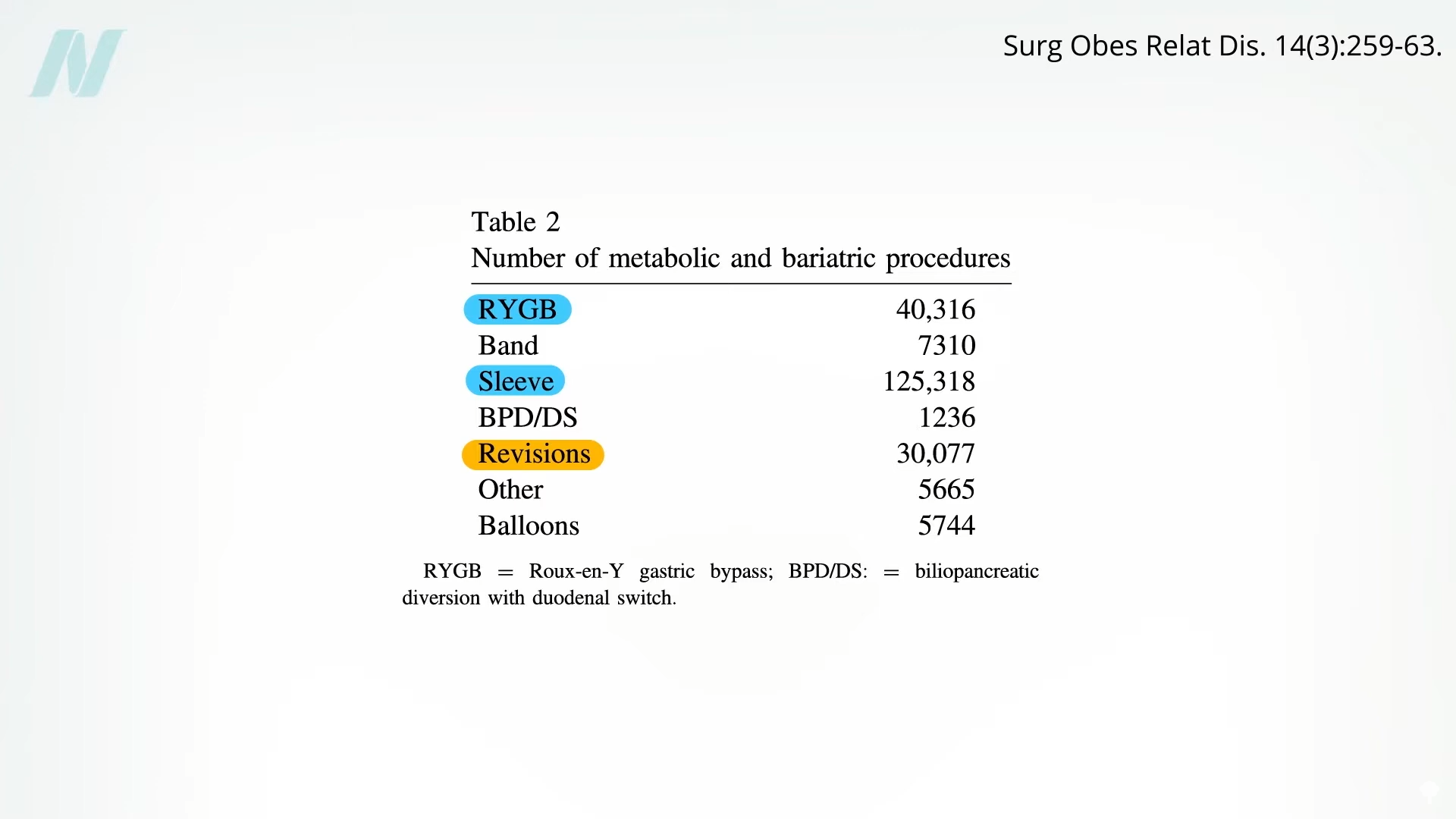
Bariatric surgery has become a cornerstone in the management of severe obesity, with procedures like sleeve gastrectomy and Roux-en-Y gastric bypass leading the charge. However, a notable trend within the field is the significant number of patients requiring revisional surgery. In fact, interventions to correct or manage complications arising from a previous bariatric procedure rank as the third most common type of bariatric operation. This statistic alone highlights the intricate nature of these surgeries and the potential for unforeseen challenges.
The need for reoperation underscores a crucial point: initial bariatric procedures, while intended to be definitive solutions, can sometimes lead to a cascade of issues. These subsequent surgeries are not only more complex but also carry a substantially higher risk profile. Reports indicate that reoperations can have a mortality rate up to ten times that of primary procedures, and success is far from guaranteed. The spectrum of complications that necessitate such interventions is broad and includes, but is not limited to, leaks at surgical sites, the formation of abnormal connections between organs (fistulas), the development of ulcers, narrowing of the digestive tract (strictures), erosion of surgical materials, blockages, and severe acid reflux.
Surgeon Skill: A Pivotal Factor in Patient Outcomes
Emerging evidence strongly suggests that the level of surgical skill is a critical determinant of patient outcomes following bariatric surgery. A groundbreaking study, published in the prestigious New England Journal of Medicine, provided compelling data to support this assertion. In this research, bariatric surgeons voluntarily submitted video recordings of their surgical procedures. These videos were then meticulously reviewed and evaluated by a panel of expert peers. The findings were stark: there was a wide variation in technical proficiency among the participating surgeons.
This variation in skill was directly linked to significant differences in patient outcomes. Surgeons exhibiting lower levels of technical competence were associated with markedly higher rates of complications, hospital readmissions, the need for reoperations, and, tragically, death. Patients operated on by less proficient surgeons experienced nearly three times the rate of complications and five times the mortality rate compared to those treated by their more skilled counterparts. This research serves as a powerful indicator that the human element – the surgeon’s dexterity, precision, and accumulated experience – plays an indispensable role in the safety and efficacy of bariatric surgery.
The Learning Curve: Mastery Through Volume and Experience
The analogy of musicians or athletes excelling through dedicated practice is fitting when considering the development of surgical expertise. While innate talent may play a role, consistent practice and a high volume of procedures are crucial for refining surgical skills. For bariatric procedures, particularly complex ones like gastric bypass, the learning curve can be substantial. Studies suggest that a surgeon may need to perform as many as 500 cases to achieve a high level of mastery.
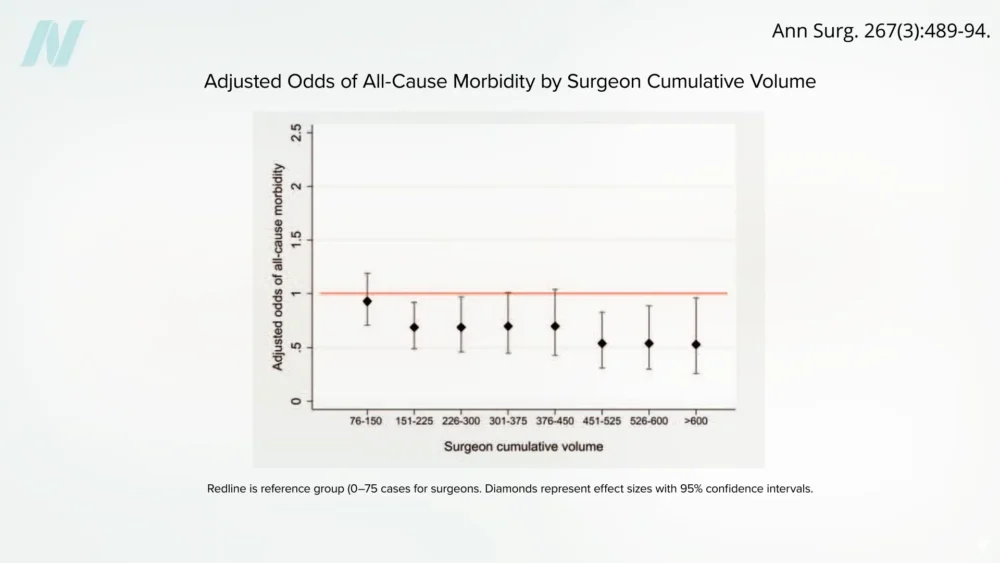
The data indicates a discernible plateau in the risk of complications after a surgeon has performed approximately 500 cases. The lowest complication rates were observed among surgeons who had completed more than 600 bypass procedures. Conversely, the risk of mortality appears to be significantly higher for surgeons with less experience. For instance, individuals undergoing surgery performed by surgeons with fewer than 75 cases had double the odds of not surviving compared to those operated on by surgeons with over 450 cases. This suggests that a threshold of experience is vital for minimizing the inherent dangers associated with these life-altering operations.

Navigating the Surgical Landscape: Recommendations for Patients
Given the profound impact of surgeon skill, prospective patients are strongly advised to approach their bariatric surgery decisions with diligence. A key recommendation is to inquire directly with potential surgeons about the number of bariatric procedures they have performed. Understanding a surgeon’s experience level can provide valuable insight into their proficiency.
Furthermore, choosing an accredited bariatric "Center of Excellence" is a prudent step. These centers are recognized for meeting rigorous standards of care and expertise. Research indicates that surgical mortality rates at accredited institutions are two to three times lower than at non-accredited facilities. This suggests a systemic advantage in patient safety and care quality at designated Centers of Excellence.
Beyond the Operating Room: Patient Responsibility and Long-Term Care
While surgeon skill is paramount, it is crucial to acknowledge that patient factors and adherence to post-operative guidelines also significantly influence outcomes. A cautionary tale illustrates this point: a surgeon described a case where a patient, three months after a gastric bypass, consumed large quantities of food at an all-you-can-eat buffet without adequate chewing. The undigested food, including large chunks of vegetables, led to a rupture of surgical staples and required emergency surgery.
This incident, though perhaps extreme, highlights the importance of post-operative dietary discipline. While the patient chose seemingly healthy foods, the failure to properly masticate them led to severe complications. This scenario serves as a reminder that successful bariatric surgery involves a lifelong commitment to mindful eating and appropriate food preparation, even when consuming nutritious options. The underlying message is that a healthy diet before surgery can also contribute to long-term well-being and potentially reduce the risk of complications.
The Lifelong Commitment to Nutritional Health
Even in cases where the surgical procedure itself is technically flawless, the journey does not end in the operating room. Bariatric surgery, particularly procedures involving malabsorption, necessitates lifelong nutritional replacement and vigilant monitoring. The alteration of the digestive system inherently impairs the body’s ability to absorb essential vitamins and minerals, leading to a heightened risk of deficiencies.
These deficiencies can manifest in a range of health problems, extending far beyond common issues like anemia, osteoporosis, or hair loss. In severe cases, patients can develop life-threatening conditions such as beriberi, pellagra, kwashiorkor, and significant nerve damage. For example, copper deficiency can lead to vision loss years or even decades after surgery. Tragically, deficiencies in thiamine, a crucial B vitamin, have been reported to cause permanent brain damage in nearly one-third of patients before the condition is identified and treated.
Understanding Malabsorption and Its Consequences
Procedures like gastric bypass are intentionally designed to induce malabsorption. By surgically altering or bypassing segments of the intestines, the body’s capacity to absorb calories is deliberately reduced. While this aids in weight loss, it comes at the significant cost of impeding the absorption of vital nutrients.

Even restrictive procedures, such as stomach stapling, can place patients at risk for life-threatening nutrient deficiencies. Persistent vomiting, which can occur in up to 60% of patients post-bariatric surgery due to "inappropriate eating behaviors" (i.e., attempting to eat normally), can exacerbate these risks. The vomiting acts as a mechanism for weight loss, similar to the disulfiram-based medications used to deter alcohol consumption by inducing severe illness.
The Role of Dumping Syndrome in Behavior Modification
Another common post-operative phenomenon is "dumping syndrome." A substantial percentage of gastric bypass patients experience symptoms such as abdominal pain, diarrhea, nausea, bloating, fatigue, or palpitations after consuming calorie-dense foods. This occurs because the food bypasses the stomach and rapidly enters the intestines.
Surgeons often describe dumping syndrome not as a complication, but as an intended feature of the surgery. It is considered a mechanism to modify patient behavior by creating an unpleasant physical response to consuming energy-dense foods, thereby deterring such consumption and contributing to weight loss.
Broader Implications for Public Health and Patient Education
The insights gained from research into bariatric surgery risks carry significant implications for public health strategies and patient education. The undeniable benefits of bariatric surgery for individuals struggling with obesity must be weighed against the potential for serious complications, particularly when surgical expertise is suboptimal.
This evolving understanding necessitates a multi-faceted approach:
- Enhanced Surgeon Training and Certification: Continued emphasis on rigorous training, competency assessment, and ongoing professional development for bariatric surgeons is crucial. The establishment and enforcement of clear standards for surgical proficiency can help ensure that patients receive care from highly qualified practitioners.
- Robust Patient Counseling and Informed Consent: Comprehensive pre-operative counseling should thoroughly address the potential risks, including those related to surgeon experience and the need for lifelong lifestyle changes. Patients must be empowered with the knowledge to make informed decisions about their care.
- Development of Patient Support Networks: Creating accessible support systems for patients undergoing and recovering from bariatric surgery can provide invaluable emotional and practical assistance, helping them navigate the challenges of post-operative life and adhere to necessary dietary and lifestyle modifications.
- Ongoing Research and Data Collection: Continued research into surgical techniques, complication rates, and long-term outcomes is vital for refining best practices and identifying emerging trends or challenges within the field of bariatric surgery.
The journey toward sustainable weight loss and improved health through bariatric surgery is a complex one. While the procedures themselves represent remarkable medical advancements, a deep understanding of the factors influencing their success, particularly the critical role of surgeon expertise and the patient’s lifelong commitment to health, is essential for navigating this path safely and effectively.






