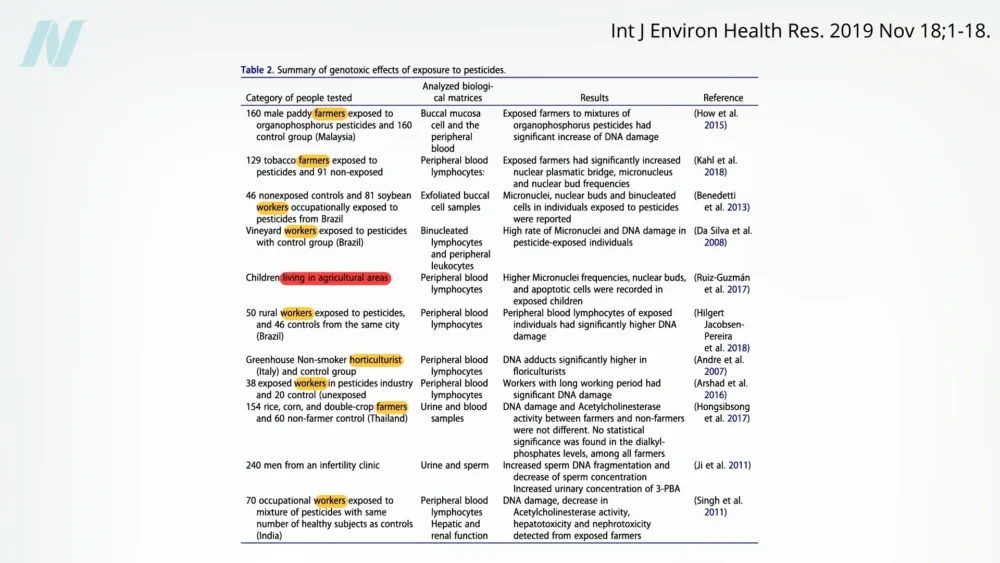

A substantial and escalating body of scientific evidence strongly suggests a significant link between pesticide exposure and an increased risk of developing cancer. This connection is so robust that experts assert its role in cancer development "cannot be doubted." While much of the foundational research highlighting the DNA-damaging effects of pesticides has focused on occupational settings – encompassing farmers, agricultural workers, and individuals residing in high-spray areas – emerging studies are beginning to shed light on the potential risks associated with non-occupational exposure, including dietary intake. This evolving understanding has propelled questions about the protective benefits of choosing organic over conventionally grown foods for cancer prevention and the overall impact of pesticides on human health.
Unpacking the Pesticide-Cancer Nexus
The scientific consensus on the detrimental effects of pesticides on human health, particularly concerning cancer, has solidified over decades of research. A comprehensive review that updated the evidence on human exposure and toxicity of pesticides underscored the magnitude of this link. This review concluded that the evidence implicating pesticide exposure in cancer development is so overwhelming that it is beyond reasonable doubt.
Historically, the most direct evidence linking pesticides to cellular damage and cancer has originated from studies involving individuals with high levels of occupational exposure. These studies have consistently documented DNA damage, a critical precursor to cancer, in agricultural workers and those directly involved in pesticide manufacturing and application. For instance, research has shown DNA fragmentation in the sperm of men with elevated pesticide levels in their bloodstream. While this evidence is compelling, it primarily represents an extreme end of the exposure spectrum.
Beyond the Fields: Non-Occupational Exposure and Emerging Concerns
The question then arises: what about the general population, whose exposure is primarily through diet and environmental contact? While direct causal links for the general populace are more complex to establish due to lower exposure levels and confounding lifestyle factors, research is beginning to bridge this gap. A study conducted in China, where average pesticide concentrations were found to be significantly higher than in many other regions, provided evidence linking non-occupational pesticide exposure to DNA damage. This study observed single- and double-stranded DNA fragmentation in the sperm of men with elevated pesticide levels, even when their exposure was not directly occupational.
Furthermore, the mechanisms by which pesticides might contribute to cancer are not limited to direct DNA damage. Emerging research suggests that pesticides can interfere with the body’s natural defense mechanisms against cancer. Specifically, pesticides have been shown to negatively impact the function of Natural Killer (NK) cells, a crucial component of the innate immune system. NK cells are the body’s first responders to threats, identifying and neutralizing cancer cells and virus-infected cells.

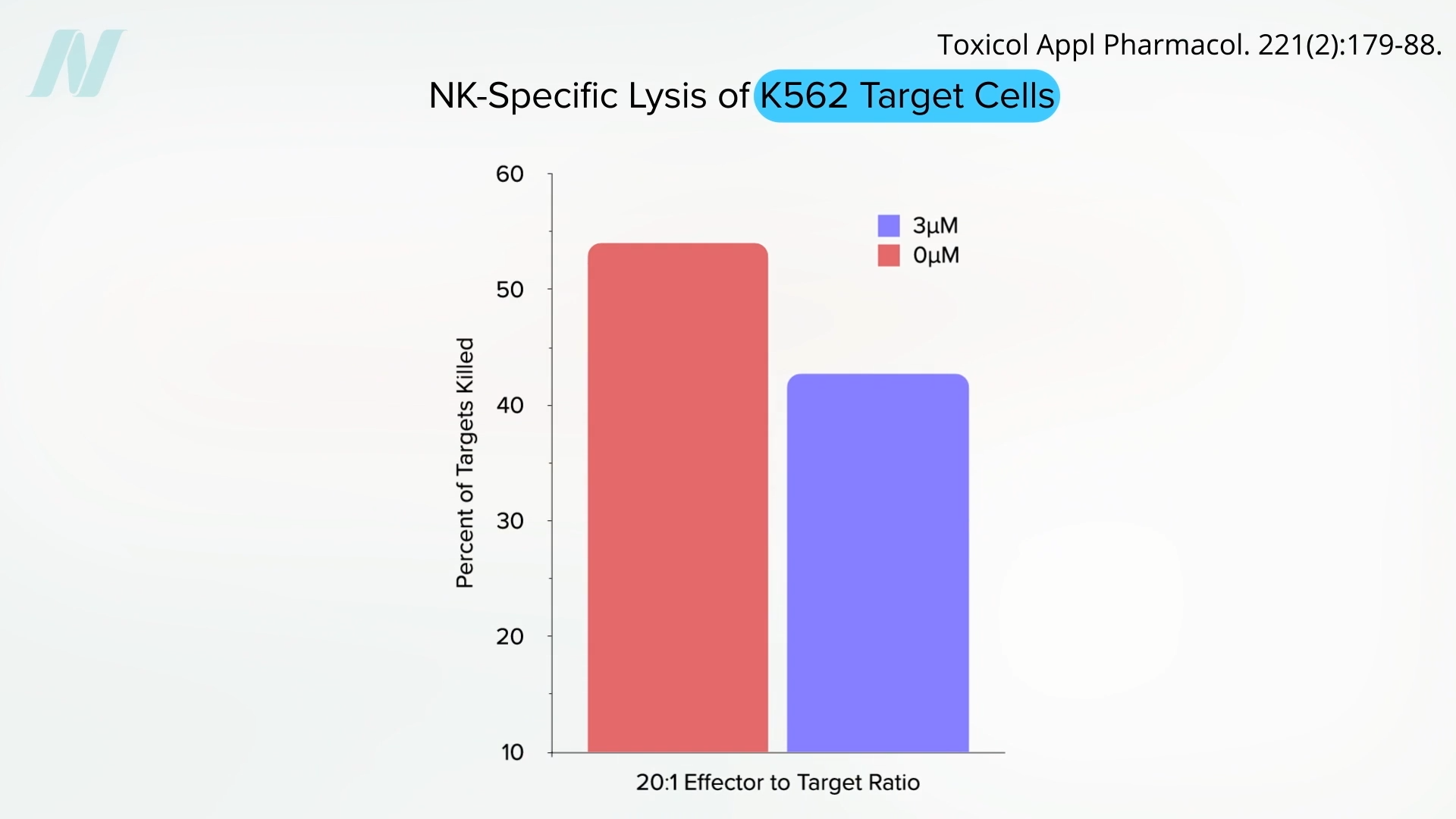
Studies have demonstrated that exposure to pesticides can significantly impair the cytotoxic activity of NK cells. In laboratory settings, NK cells, when exposed to human leukemia cells without any pesticide interference, can effectively eliminate a substantial portion of the cancerous cells. However, the introduction of even small amounts of pesticides can severely disable these immune cells, allowing cancer cells to proliferate unchecked. This impairment of anticancer immunity represents another significant pathway through which pesticides could potentially facilitate tumor growth and progression.
Quantifying the Risk: From Occupational to Dietary Exposure
The critical question for the general public revolves around the levels of pesticide exposure encountered through daily life, particularly from consuming conventionally grown produce. The high levels of pesticides used in the laboratory studies that demonstrate significant cellular damage are often comparable to those experienced by individuals actively spraying pesticides. This raises a crucial point: what are the implications of the residual pesticides found on conventionally grown fruits and vegetables?
It is widely acknowledged that pesticide residues are detectable in the blood and urine of a vast majority of the U.S. population, irrespective of their occupation or geographic location. Studies employing crossover trials, where participants switch between consuming conventionally grown and organically produced foods, have provided compelling evidence of the dietary source of this exposure. These trials show that urinary concentrations of pesticide metabolites can be rapidly reduced, akin to "turning on and off a light switch," by eliminating conventionally grown foods from the diet.
However, the direct health consequences of ingesting these residual pesticides remain a subject of ongoing investigation. While the presence of pesticides in the body is confirmed, the threshold at which they become harmful to human health, particularly concerning chronic diseases like cancer, is not definitively established for the general population.
The Organic Advantage: Examining the Evidence
In light of these concerns, the choice to opt for organic foods as a cancer prevention strategy has garnered significant attention. While the benefits of organic foods are often discussed in terms of reduced pesticide exposure, the scientific evidence directly linking organic food consumption to cancer risk reduction has been building, albeit with some nuances.
A landmark study provided the first comprehensive evaluation of the association between the frequency of organic food consumption and cancer risk, meticulously controlling for a wide array of potential confounding factors. This study found that individuals who self-reported the highest frequency of organic food consumption exhibited approximately a 25% lower risk of developing cancer overall.

The researchers rigorously addressed potential biases that might influence such findings. They accounted for factors such as age, socioeconomic status, education level, body mass index (BMI), physical activity, meat consumption, and smoking habits, all of which could independently affect cancer risk. Even after controlling for these variables, the association between higher organic food consumption and reduced cancer risk remained statistically significant.
Furthermore, the study explored whether differences in overall dietary patterns, beyond the organic versus conventional distinction, could explain the observed results. This included controlling for factors like higher overall intake of fruits and vegetables or lower consumption of processed foods. Despite these adjustments, the protective association persisted. The researchers concluded that their findings "indicate that higher organic food consumption is associated with a reduction in the risk of overall cancer."
A Deeper Dive into Cancer Subtypes and Mortality
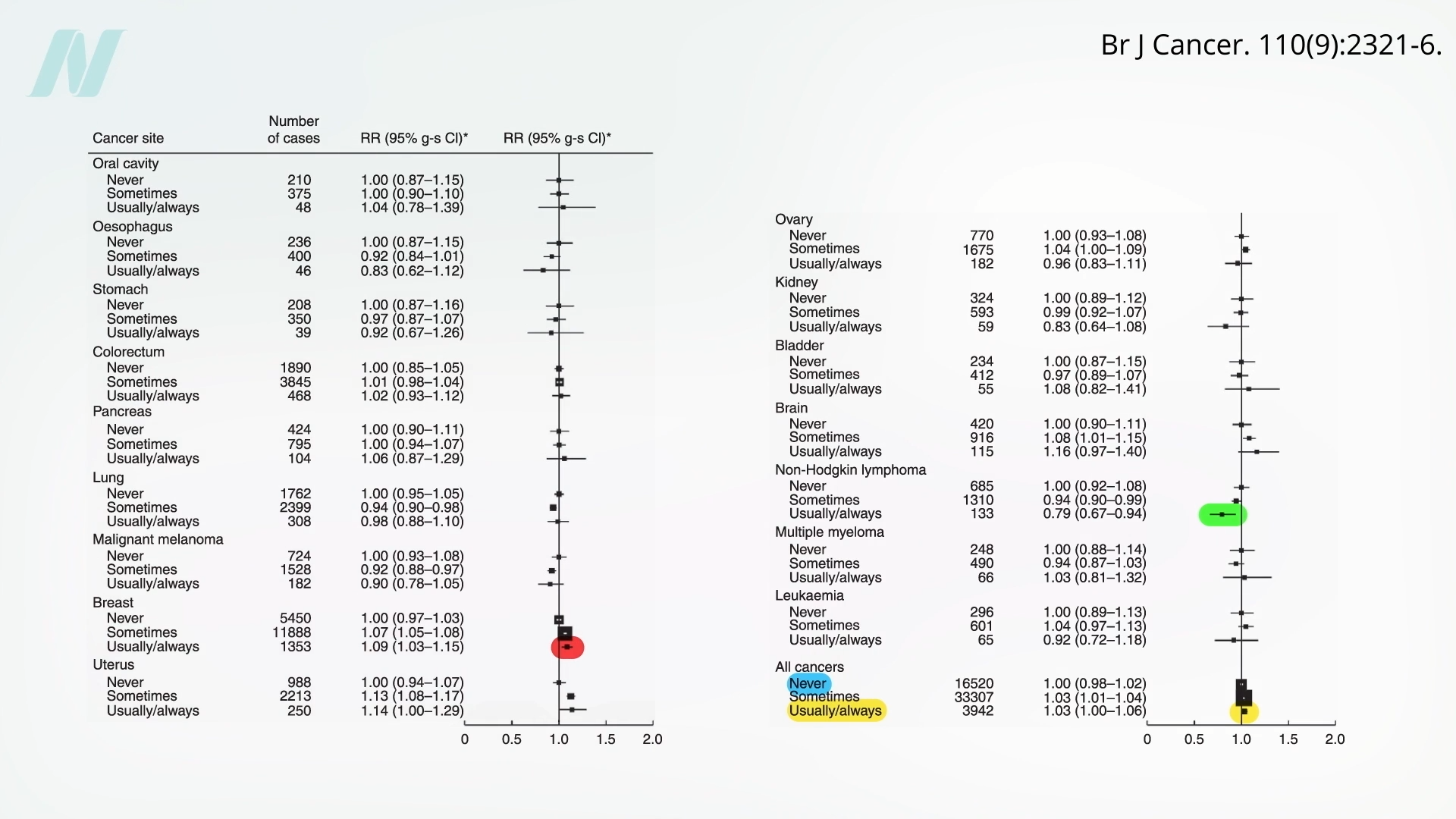
While the aforementioned study offered robust evidence for a general reduction in cancer risk, earlier, larger-scale investigations have yielded more specific findings. One such extensive study found little evidence for a decrease in the incidence of most cancers among organic food consumers, with the exception of a potential reduction in a specific type of blood cancer: non-Hodgkin lymphoma.
This earlier study’s data indicated no significant difference in the overall incidence of cancer between individuals who never consumed organic foods and those who regularly did. However, it did highlight a statistically significant lower risk of non-Hodgkin lymphoma. Intriguingly, this study also noted an increased risk of breast cancer among those who frequently consumed organic foods. The researchers acknowledged the possibility that this observed increase might be influenced by behavioral factors, such as a greater conscientiousness among organic consumers to undergo regular breast cancer screenings, leading to earlier detection and diagnosis. However, definitive conclusions regarding this potential confounding factor remain elusive.
Beyond cancer incidence, concerns about the long-term health impacts of pesticide exposure extend to all-cause mortality – the risk of dying prematurely from any cause. Research has indicated a correlation between elevated blood levels of certain persistent pesticides and a shortened lifespan. For instance, higher blood levels of beta-hexachlorocyclohexane, a persistent organic pollutant, have been associated with a significantly reduced life expectancy.
Dietary Choices and Pesticide Accumulation
Understanding how dietary choices influence the body’s pesticide burden is crucial. Chlorinated pesticides, like beta-hexachlorocyclohexane, are lipophilic, meaning they are fat-soluble and tend to accumulate in fatty tissues. Consequently, they are found more frequently in foods of animal origin, such as meat, dairy products, and eggs.
Historical studies have illustrated this phenomenon. One such study found that the breast milk of vegetarian mothers contained significantly lower levels of beta-hexachlorocyclohexane compared to their non-vegetarian sisters who were also breastfeeding. The vegetarian mothers exhibited approximately one-third lower levels of this pesticide in their milk, suggesting a direct link between dietary patterns and the accumulation of fat-soluble pesticides.
More contemporary research has explored the presence of other persistent organic pollutants, such as polychlorinated biphenyls (PCBs), which are structurally similar to some pesticides and are also fat-soluble. A recent study examining PCBs found them to be linked to increased mortality risk. Similar to beta-hexachlorocyclohexane, these toxins were predominantly found in foods of animal origin, including eggs, dairy, and animal fats.
This body of evidence aligns with findings that the blood of individuals following a vegan diet is "significantly less polluted" than that of omnivores in terms of a range of PCBs associated with increased mortality. While vegans in these studies did not consistently show lower levels of beta-hexachlorocyclohexane, the overall trend points towards a reduction in certain pesticide-type compounds by limiting the intake of animal products.
Navigating the Nuances: The Verdict on Conventional Produce
The complex interplay between pesticide exposure, dietary choices, and health outcomes necessitates a balanced perspective. When it comes to fruits and vegetables, the overwhelming consensus among public health experts is that the nutritional benefits of consuming them, even if conventionally grown, likely outweigh the potential risks associated with pesticide residues.
The benefits of a diet rich in fruits and vegetables – including essential vitamins, minerals, fiber, and antioxidants – are profound and well-documented, contributing significantly to overall health and disease prevention. While concerns about pesticide exposure are valid, the estimated impact of these residues on lifespan is minimal. One analysis suggested that the potential lifelong damage from pesticides on produce might only shave off a few minutes from a person’s life, on average. This minuscule risk pales in comparison to the substantial health advantages gained from consuming a diet abundant in fruits and vegetables.
Therefore, public health messaging consistently encourages individuals not to let concerns about pesticide residues deter them from increasing their intake of fruits and vegetables. The emphasis remains on maximizing the consumption of these nutrient-dense foods, while simultaneously advocating for sustainable agricultural practices and reduced pesticide use.

Broader Implications and Future Directions
The ongoing research into the health effects of pesticides and the comparative benefits of organic foods has significant implications for public health policy, agricultural practices, and individual consumer choices. The consistent findings of reduced cancer risk and potentially lower all-cause mortality associated with higher organic food consumption, particularly when controlling for numerous lifestyle factors, warrant continued investigation.
The evidence suggesting a link between pesticide exposure and impaired immune function highlights a critical area for further research, particularly concerning vulnerable populations and long-term, low-level exposures. Understanding the precise mechanisms of immune system modulation by pesticides could lead to targeted interventions and preventative strategies.
Moreover, the disparity in pesticide levels observed between different dietary patterns underscores the importance of dietary choices in mitigating exposure to environmental toxins. Continued public education about the potential benefits of reducing intake of animal products for those concerned about pesticide accumulation is warranted, alongside a broader understanding of the complex nutritional and toxicological profiles of various food sources.
Ultimately, the pursuit of a healthier future hinges on a multifaceted approach that includes supporting sustainable agricultural methods, promoting informed consumer choices, and fostering continued scientific inquiry into the intricate relationship between our environment, our diet, and our long-term health. The conversation around organic versus conventional foods is not simply about pesticide residues; it is an integral part of a larger dialogue on food safety, environmental stewardship, and the proactive pursuit of well-being.






