The quest for a slimmer physique has led individuals and medical professionals down some unconventional and, at times, ethically dubious paths. From surgically implanted devices to parasitic invasions, the landscape of weight loss interventions is fraught with methods that raise significant safety and efficacy concerns. This exploration delves into a range of these extreme approaches, dissecting their mechanisms, documented outcomes, and the underlying scientific rationale, or lack thereof.
The Calorie Conundrum: Why Quick Fixes Tempt
The fundamental principle of weight loss revolves around caloric balance: consuming fewer calories than the body expends. However, the modern food environment, characterized by highly palatable, energy-dense processed foods and sugary beverages, presents a formidable challenge to this equilibrium. For instance, a moderately obese individual engaging in moderate physical activity, such as an hour of brisk walking or cycling, might burn approximately 350 calories. In stark contrast, a seemingly innocuous snack or drink, often laden with refined sugars and fats, can deliver around 70 calories per minute. This alarming disparity means that a mere five minutes of consuming such items can negate an entire hour of dedicated exercise, underscoring the allure of more direct, albeit radical, weight loss strategies.
The AspireAssist Siphon: A Direct Drainage Approach
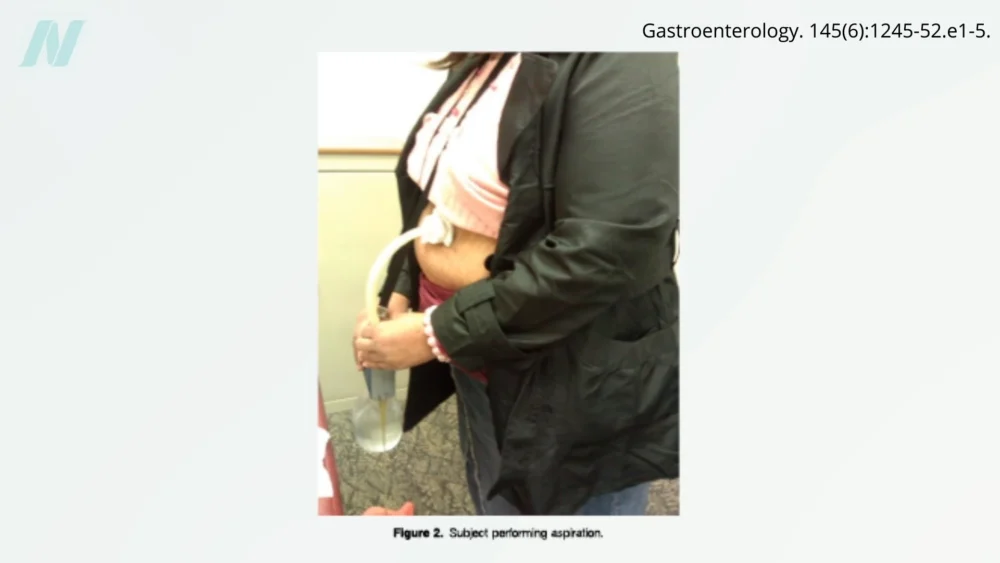
One of the more invasive interventions to emerge in this realm is the AspireAssist siphon assembly. This device involves a surgical procedure to create a percutaneous gastrostomy, where a hole is made in the stomach and a fistula is tunneled through the abdominal wall. Post-meal, individuals can attach a suction device to this opening to drain a significant portion of their stomach contents. This method, while undeniably resulting in weight loss, facilitates a direct removal of ingested calories, effectively allowing individuals to consume food and then mechanically expel it.
Mechanism and Reported Outcomes:
The AspireAssist system operates by creating a conduit between the stomach and the exterior. After a meal, a tube is inserted through the abdominal wall into the stomach, and a portable external device is used to aspirate the stomach contents. Studies have indicated that patients using the AspireAssist can experience substantial weight loss. For example, a study published in the American Journal of Surgery (referencing research that informed the original text) noted weight loss in patients utilizing this device.
Beyond the direct removal of calories, several factors may contribute to the observed weight reduction. The presence of the fistula itself might impede the normal relaxation of the stomach wall during eating, potentially leading to earlier feelings of fullness. Furthermore, the protocol often requires patients to drink considerable amounts of water and chew their food thoroughly, both of which can contribute to satiety and a slower eating pace. Anecdotal reports and some study observations suggest that patients also begin making healthier food choices to avoid the visually unappealing nature of aspirating processed or fatty foods, which tend to appear particularly unappetizing when removed.
Safety and Complications:
While the AspireAssist does not alter the fundamental anatomy of the gastrointestinal tract, it is not without risks. A significant concern is the potential for nutrient deficiencies, particularly potassium, as stomach juices are aspirated. Patients are typically advised to take potassium supplements to mitigate this risk, mirroring a complication seen in conditions like bulimia nervosa. Minor wound complications at the gastrostomy site are also reported. More serious adverse events, such as abdominal abscesses, are described as rare, according to medical literature. The "palatability" of the procedure itself, meaning the psychological and physical experience of using the device, has also been a subject of concern.
The Duodenal-Jejunal Bypass Liner: An Internal Obstruction
Another intervention that bypasses traditional surgical restructuring is the duodenal-jejunal bypass liner, such as the EndoBarrier. This device is essentially a flexible tube, several feet in length, that is inserted into the small intestine to line the duodenal and jejunal walls. The intended mechanism is to create a physical barrier that prevents the direct contact of food with the intestinal lining, thereby reducing calorie and nutrient absorption. This approach aims to mimic some of the effects of more invasive gastric bypass surgery without extensively altering the digestive tract’s anatomy.
Challenges and Adverse Effects:
The primary challenge with the EndoBarrier lies in its implantation and anchoring within the digestive tract. The device is typically secured using multiple barbed hooks, often numbering around ten. These hooks are designed to lodge into the intestinal wall to prevent migration. However, this anchoring mechanism is a significant source of adverse events. Data from clinical trials have indicated a high rate of complications. A review of studies involving a substantial number of patients (as cited in the source material) revealed that a large proportion experienced adverse effects, with lacerations caused by the barbs being a predominant issue. More severe complications, including penetrating trauma leading to esophageal perforation or liver abscesses, have also been documented, albeit at a lower frequency.
Intestinal Resurfacing: A Thermal Approach
Perhaps one of the most startling interventions discussed is the concept of "intestinal resurfacing." This involves a procedure where the superficial lining of the duodenum, the first part of the small intestine, is thermally ablated. The intention is to remove the existing mucosal layer and allow for the growth of a new one, theoretically impacting nutrient absorption. The term "resurfacing" is used to describe this process of burning off or regenerating the intestinal lining. While the specifics of long-term efficacy and safety are less widely publicized than other methods, the idea of deliberately damaging and regenerating intestinal tissue for weight loss raises profound questions about the body’s resilience and the potential for unforeseen consequences.
Botulinum Toxin (Botox) Injections: A Muscle Paralysis Attempt
In a less invasive, yet ultimately unsuccessful, attempt to influence weight, researchers explored the use of Botulinum Toxin (Botox) injections into the stomach walls of obese individuals. The hypothesis was that partially paralyzing the gastric muscles would slow down stomach emptying, leading to prolonged feelings of fullness and, consequently, reduced food intake and weight loss.
Research Findings:
Clinical trials investigating this application have generally yielded negative results. Studies, including those referenced in the source material, have indicated that Botox injections into the stomach do not lead to significant or sustainable weight loss. The rationale, while conceptually plausible in theory, did not translate into effective clinical outcomes. This highlights the complexity of the physiological processes involved in appetite regulation and satiety, which are not solely dictated by gastric muscle function.

Corsets and Tapeworms: Historical Oddities and Persistent Myths
The history of weight loss is replete with methods that, in retrospect, seem more like historical curiosities than viable medical interventions. The use of corsets, for instance, was investigated in a study where participants were instructed to wear them for extended periods. The results, predictably, were not encouraging, with participants finding the garments uncomfortable and failing to adhere to the regimen. This underscores that restrictive clothing, while potentially offering a temporary sensation of reduced intake, is not a sustainable or effective long-term weight loss strategy.
Another persistent, albeit disturbing, method that has circulated since the early 1900s is the purported use of "sanitized tapeworms." The idea was to ingest tapeworm eggs, allowing the parasites to mature in the digestive tract and consume ingested food, thus reducing calorie absorption. However, evidence suggests that the presence of living tapeworms has been discovered during bariatric surgery, indicating that this method is not only ineffective but also poses serious health risks associated with parasitic infestation. The implications of such practices range from nutrient deficiencies and digestive distress to more severe systemic infections.
Harnessing Disgust: A Psychological Intervention
In a departure from physical interventions, researchers have explored the use of psychological manipulation to curb appetite. One study, titled "Harnessing the Power of Disgust: A Randomized Trial to Reduce High-Calorie Food Appeal Through Implicit Priming," investigated the potential of subliminal messaging to influence food preferences. This research involved exposing participants to positive imagery (like kittens) before showcasing healthy food options and negative imagery (such as cockroaches or vomit) before presenting high-calorie foods.
Study Outcomes and Implications:
The study suggested that this "implicit priming" could reduce the appeal of high-calorie foods. By associating unhealthy foods with feelings of disgust through rapid, subconsciously perceived negative stimuli, researchers aimed to decrease cravings. While this approach did not directly measure actual consumption, participants reported a diminished desire for high-calorie options. The conclusion drawn was that subliminal aversion might serve as a novel tactic to counteract the pervasive environmental cues that promote unhealthy eating habits. This research opens a potential avenue for behavioral interventions that leverage psychological responses without the physical risks associated with other methods.
Electrostimulation and Brain Intervention: The Cutting Edge of Questionable Science
The pursuit of weight loss has also ventured into the realm of electrostimulation, targeting both the digestive system and the brain. Various approaches have been attempted, often met with limited success and significant ethical considerations.
Gastric and Colon Stimulation:
Research has explored implanting electrodes into the muscular layer of the stomach wall to influence its function and potentially reduce food intake. When gastric stimulation proved ineffective, investigations extended to colon electrical stimulation. These methods, however, have not yielded widespread adoption or definitive positive results in large-scale clinical settings, suggesting that electrical manipulation of the gut alone is not a robust solution for obesity.
Brain Stimulation for Appetite Control:
Perhaps the most invasive and controversial area of research involves direct brain stimulation. Studies have investigated whether electrical stimulation of specific brain regions could reduce food intake. This has involved drilling holes into the skulls of individuals to insert electrodes into their brains for "electrostimulatory exploration." While some experiments in animal models, such as cats and monkeys, showed promise in eliciting hunger responses and potentially influencing intake, human trials have largely failed to translate these findings into effective weight loss. The researchers found that while specific brain spots could be identified that influenced hunger, the subsequent "burning out" of these areas through electrocoagulation did not result in weight loss in obese human subjects. This underscores the immense complexity of the human brain and the multifaceted nature of appetite regulation, far beyond simple electrical manipulation. The risks associated with such procedures, including the inherent complications of brain surgery, are substantial.
The International Perspective: A Critical View of American Innovations
The array of extreme weight loss methods emerging from the United States has not gone unnoticed by the international medical community. Commentaries and journal articles, such as those published in Obesity Surgery, have expressed bemusement and concern regarding the unconventional nature of some American interventions. Titles like "What Are the Yanks Doing?" reflect a critical stance on these often experimental and sometimes radical approaches to tackling obesity. This global perspective highlights the diverse approaches to health and wellness and the varying tolerance for risk in medical innovation.
Towards Sustainable Solutions: A Focus on Healthy Habits
The overwhelming evidence from these explorations into extreme weight loss methods points to a consistent theme: quick fixes and invasive procedures rarely offer sustainable or safe solutions. The underlying principles of healthy weight management remain rooted in established, evidence-based practices. As articulated in comprehensive guides on healthy living and weight loss, the most effective strategies involve a balanced diet rich in whole foods, regular physical activity, and behavioral changes that foster long-term adherence. These approaches, while requiring sustained effort and commitment, offer a path to improved health and well-being without the significant risks and ethical quandaries associated with more radical interventions. The journey to a healthier weight is not about finding a shortcut but about cultivating sustainable habits that support lifelong wellness.
Doctor’s Notes on Related Topics:
For those seeking to understand the safety and efficacy of other popular weight loss procedures, further information is available on gastric balloon surgery. Additionally, a comprehensive review of weight loss pills, examining both their safety and effectiveness, can provide valuable insights into this widely used category of interventions.
The path to sustainable weight loss is best navigated through evidence-based lifestyle modifications. Resources such as dedicated books and expert-led discussions often focus exclusively on scientifically validated methods for achieving and maintaining a healthy weight. These resources emphasize the importance of a holistic approach, integrating nutrition, exercise, and behavioral strategies.






