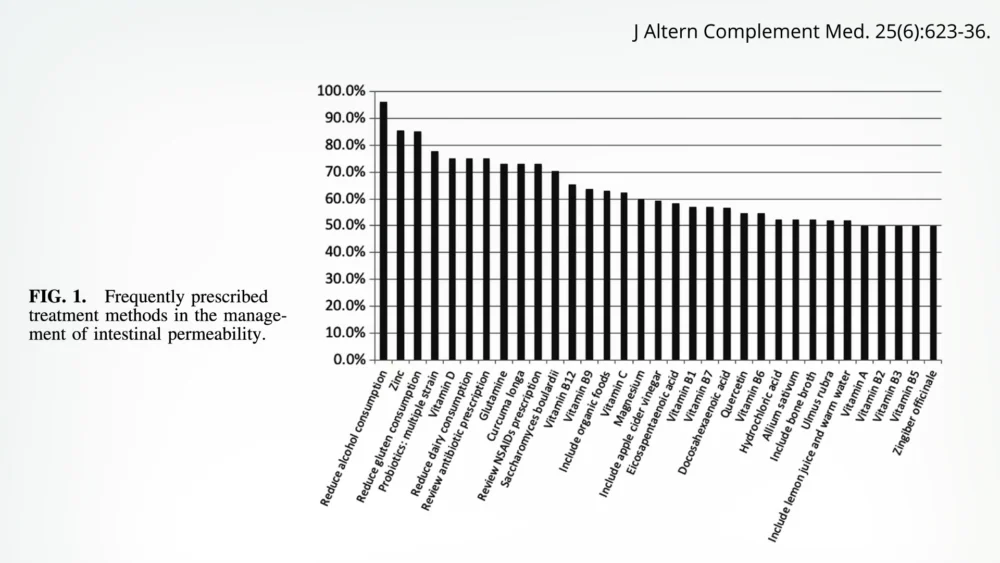
The human gastrointestinal tract stands as our primary, most expansive interface with the external environment. While we constantly interact with the world through touch and respiration, the foods and beverages we consume represent our most significant and direct exposure. Ideally, the entire digestive system functions as a highly selective barrier, meticulously controlling the passage of substances into and out of the body. However, a confluence of factors, with diet frequently taking center stage, can compromise this delicate impermeability, leading to what is commonly referred to as a "leaky gut." This condition, characterized by an impaired intestinal barrier, allows undigested food particles, microbes, and toxins to permeate the gut lining and enter the bloodstream, potentially triggering widespread chronic inflammation throughout the body.
Understanding Gut Dysbiosis and the Western Diet
The prevalence of conditions associated with a compromised intestinal barrier has spurred significant research into its underlying causes and potential dietary interventions. A key culprit identified in numerous studies is the standard American or Western diet. This dietary pattern, often rich in processed foods, refined sugars, unhealthy fats, and low in fiber, has been linked to gut dysbiosis – a detrimental imbalance in the composition and function of the gut microbiome.
Gut dysbiosis can initiate a cascade of negative effects, including inflammation within the intestinal lining. When the intestinal barrier becomes "leaky," the tight junctions between the cells that form the gut wall weaken. This loosening allows molecules that should remain within the digestive tract to cross into the bloodstream. The immune system, encountering these foreign substances in an inappropriate location, can mount an inflammatory response. Over time, this chronic, low-grade systemic inflammation has been implicated in a wide array of health issues, from autoimmune diseases and metabolic disorders to neurological conditions and mental health challenges.
The Plant-Powered Solution: A Vegetarian Diet’s Impact
In stark contrast to the Western diet, research consistently points towards a predominantly vegetarian diet as a cornerstone for restoring and maintaining intestinal barrier integrity. This dietary approach, essentially prioritizing the consumption of plant-based foods, fosters a healthier gut microbiome. Studies have demonstrated that individuals adhering to vegetarian diets tend to exhibit a more balanced gut microbiome, characterized by higher bacterial diversity and a stronger intestinal barrier.
The mechanisms behind this protective effect are multifaceted. Plant-based diets are naturally rich in dietary fiber, which serves as the primary fuel source for beneficial gut bacteria. These bacteria ferment fiber to produce short-chain fatty acids (SCFAs), such as butyrate, propionate, and acetate. SCFAs are vital for gut health; they provide essential nourishment to the cells lining the colon, bolstering their energy supply and promoting their proliferation and repair. Butyrate, in particular, plays a crucial role in maintaining the integrity of the intestinal epithelium and reducing inflammation.
Furthermore, vegetarian diets are typically lower in compounds that can promote gut inflammation and the production of harmful uremic toxins. For instance, vegetarians generally have lower levels of indole and p-cresol, byproducts of protein breakdown that can be detrimental to gut health when present in excess. The enhanced production of SCFAs and the reduced exposure to inflammatory compounds collectively contribute to a more robust and resilient intestinal barrier.

Evidence from Clinical Studies: Fiber’s Role in Gut Health
The pivotal role of dietary fiber in strengthening the intestinal barrier has been a subject of rigorous scientific investigation. A notable study involving individuals with non-alcoholic fatty liver disease (NAFLD) provided compelling evidence. Over a six-month period, participants were instructed to consume a diet rich in whole grains, beans, lentils, fruits, vegetables, nuts, and seeds. Following this intervention, researchers observed a significant reduction in circulating levels of zonulin.
Zonulin is a protein that plays a critical role in regulating the permeability of the intestinal barrier. It functions by loosening the tight junctions between intestinal epithelial cells, thereby increasing gut permeability. Elevated zonulin levels are widely considered a reliable biomarker for impaired intestinal barrier function, often referred to as a "leaky gut." The observed decrease in zonulin levels in the study participants strongly suggests that a diet abundant in plant-based foods, and consequently high in fiber, effectively helps to maintain the structural integrity and proper functioning of the intestinal barrier.
While this study provided significant insights, the researchers themselves acknowledged the need for more definitive proof of causality. The diet incorporated a broad spectrum of plant-based foods, making it challenging to isolate the precise contribution of fiber versus other beneficial compounds present in these foods. To address this, a more controlled study design was required.
Randomized Controlled Trials: Confirming Fiber’s Efficacy
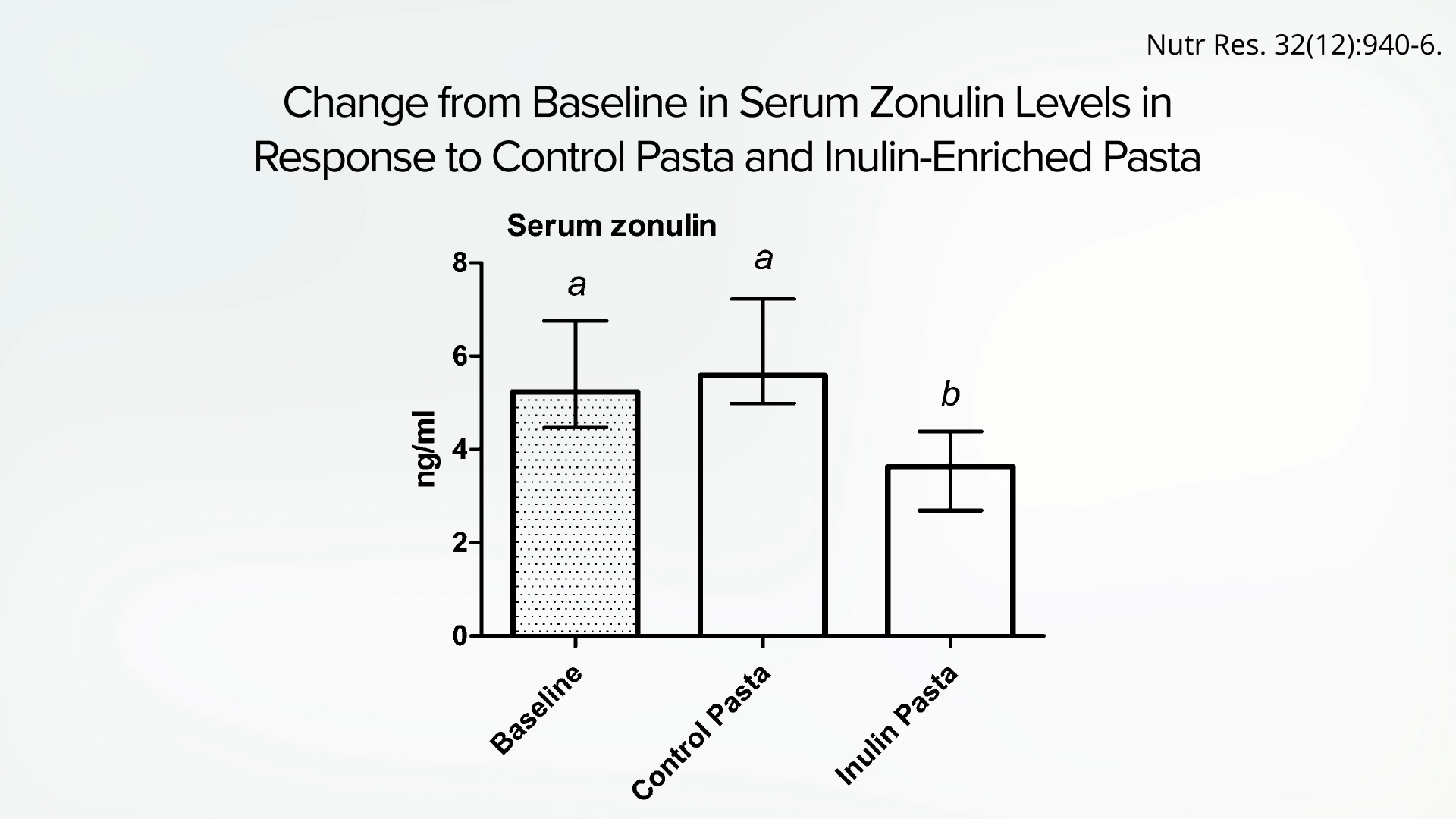
Subsequent research, employing a more rigorous randomized, double-blind, crossover study design, has further solidified the link between dietary fiber and gut health. In one such trial, healthy young men were randomly assigned to consume pasta with or without added fiber. The results were striking: the group that consumed pasta with added fiber exhibited a significant reduction in zonulin levels compared to their pre-intervention levels and to the control group that received regular pasta. This finding provides strong evidence that dietary fiber, independent of other dietary components, can actively improve gut leakiness.
This type of study design is crucial in establishing cause-and-effect relationships. By comparing the same food item with and without a specific component (in this case, fiber) and blinding participants to their treatment, researchers can confidently attribute the observed effects to that component. The consistent findings across multiple studies underscore the importance of adequate fiber intake for maintaining a healthy and impermeable intestinal barrier.
Beyond Fiber: Specific Plant Compounds and Micronutrients
While fiber stands out as a primary driver of intestinal barrier health, emerging research suggests that other components found in plant-based foods, as well as certain micronutrients, may also offer protective benefits.
Curcumin: The vibrant yellow pigment found in turmeric, curcumin, has demonstrated promising effects in preclinical studies. Research in rats has shown that curcumin can help prevent intestinal damage induced by non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen. This protective effect is thought to be mediated by curcumin’s potent anti-inflammatory and antioxidant properties, which can help mitigate the damage to the gut lining caused by these medications.
Sulforaphane: A compound found in cruciferous vegetables like broccoli, sulforaphane, has also shown similar protective capabilities in animal models. Studies in mice have indicated that sulforaphane can shield the intestinal barrier from damage. While direct human studies on sulforaphane’s impact on gut permeability are still limited, preliminary research on turmeric in humans has shown positive results. A study involving a moderate daily intake of turmeric (equivalent to about 2 to 3 teaspoons) was found to reduce markers of gastrointestinal barrier damage and exercise-induced inflammation when compared to a placebo. Further research is ongoing to determine the optimal dosages and the specific mechanisms through which these plant compounds exert their beneficial effects.
Zinc: Beyond plant compounds, the mineral zinc has long been recognized in alternative medicine circles as a key nutrient for addressing leaky gut. Clinical evidence supports this notion. Studies have shown that zinc can protect against NSAID-induced intestinal damage in rats. More importantly, a randomized trial in healthy adults demonstrated that concurrent zinc supplementation prevented the expected rise in gut permeability caused by indomethacin, a potent NSAID. This finding strongly suggests a protective role for zinc in the small intestine.
While the dose of zinc used in some of these studies was substantial, other research indicates that even lower doses can be effective. A study found significant improvements in gut leakiness with a dose of just 3 mg of zinc, suggesting that modest zinc supplementation may be sufficient. For individuals seeking to increase their dietary zinc intake, incorporating nutrient-rich foods is recommended. For instance, a single cup (200g) of cooked lentils can provide an additional 3 mg of zinc to the daily diet, contributing to improved gut barrier function.
Dietary Recommendations and Broader Implications
The cumulative evidence from scientific research strongly advocates for a dietary approach that emphasizes whole, unprocessed plant foods. This includes a wide array of fruits, vegetables, whole grains, legumes, nuts, and seeds. These foods are not only rich in fiber but also provide a spectrum of vitamins, minerals, antioxidants, and other phytochemicals that work synergistically to support gut health and reduce inflammation.
Conversely, limiting or avoiding processed foods, refined sugars, excessive saturated and trans fats, and excessive alcohol consumption is crucial for preventing and managing leaky gut. These dietary elements can disrupt the gut microbiome, promote inflammation, and directly damage the intestinal lining.
The implications of these findings extend far beyond digestive health. A compromised intestinal barrier and the resulting systemic inflammation are increasingly recognized as contributing factors to a multitude of chronic diseases, including obesity, type 2 diabetes, cardiovascular disease, autoimmune disorders, and even certain neurological and mental health conditions. By adopting a diet that prioritizes intestinal barrier integrity, individuals can potentially mitigate their risk of developing these conditions and improve their overall well-being.
Further research is continuously expanding our understanding of the intricate relationship between diet, the gut microbiome, and human health. As scientific inquiry progresses, the role of targeted dietary interventions in preventing and managing complex health issues is becoming increasingly evident, positioning nutrition as a powerful tool in the pursuit of long-term wellness.






