The intricate lining of our intestines, a crucial barrier safeguarding our health, is more vulnerable than previously understood. Emerging scientific evidence indicates that common medications, dietary staples, and even everyday beverages can compromise this vital intestinal barrier, leading to a condition colloquially known as "leaky gut." This disruption of intestinal permeability, the ability of the gut lining to selectively allow nutrients to pass while blocking harmful substances, is now being recognized as a significant factor in both the prevention and treatment of a growing number of diseases.
The sheer scale of the intestinal barrier is remarkable. With its extensive surface area, characterized by countless folds and villi, it covers an area estimated to be over 4,000 square feet – a space larger than a tennis court. Maintaining this extensive and highly active surface requires a substantial commitment from the body, consuming approximately 40% of our total energy expenditure. This significant energy investment underscores the critical role the intestinal barrier plays in overall physiological function.
Recent scientific investigations are increasingly implicating a compromised intestinal barrier as a key player in the pathogenesis of various health conditions. Studies have drawn a direct link between disruptions in intestinal barrier integrity and the development of chronic inflammatory disorders, including celiac disease and inflammatory bowel disease (IBD), such as Crohn’s disease and ulcerative colitis. The mechanisms by which this barrier is breached are diverse, but the consequences can be far-reaching, potentially impacting immune responses and systemic inflammation.
A foundational method for assessing intestinal permeability involves the use of inert markers, such as blue food coloring. In individuals with a healthy and intact intestinal barrier, this marker typically remains within the gastrointestinal tract. However, in critically ill patients, particularly those suffering from sepsis – a life-threatening systemic inflammatory response to infection – researchers have detected this marker in the bloodstream. This observation signifies a breakdown in the gut lining, allowing substances that should remain confined to the intestine to enter the circulation, potentially exacerbating the systemic inflammatory cascade.
However, the concept of a "leaky gut" is not confined to severe medical emergencies or intensive care unit settings. Evidence suggests that even individuals in good health can experience a transient increase in intestinal permeability through the use of commonly available over-the-counter medications.
The Impact of Over-the-Counter Pain Relievers
Non-steroidal anti-inflammatory drugs (NSAIDs), a class of medications widely used for pain relief and inflammation reduction, have been identified as significant contributors to intestinal barrier dysfunction. Studies have demonstrated that even a single dose of common NSAIDs can increase gut leakiness. For instance, research indicates that taking just two standard aspirin tablets (325 mg each) or two extra-strength aspirin tablets (500 mg each) can measurably increase intestinal permeability. This finding suggests that even healthy individuals should exercise caution and judiciously use aspirin, as it possesses the potential to disrupt the gastrointestinal barrier.
The concern extends beyond standard aspirin formulations. Buffered aspirin, which combines aspirin with an antacid, is often marketed with the implication that it mitigates gastrointestinal irritation. However, scientific inquiry suggests this buffering effect may be largely superficial. Studies have revealed that both regular aspirin and buffered aspirin formulations can induce multiple erosions in the delicate inner lining of the stomach and intestine. Endoscopic examinations, where a camera is inserted into the digestive tract, have documented extensive redness and erosions in the gastrointestinal lining of a significant percentage (up to 90%) of individuals who took aspirin or Bufferin at recommended doses. Alarmingly, this damage can manifest rapidly, with researchers observing significant erosions within just five minutes of administration.
In contrast, acetaminophen, widely known in the United States as Tylenol, appears to present a lower risk of gastrointestinal damage compared to NSAIDs. While acetaminophen is generally considered a safer alternative for the stomach and intestines, it is crucial to note potential liver toxicity, especially in individuals with pre-existing liver conditions or when taken in excessive doses.
Furthermore, some dietary supplements, rather than offering protection, may exacerbate the effects of NSAIDs on gut permeability. Vitamin C supplements, for example, have been observed in some studies to worsen the aspirin-induced increase in gut leakiness, suggesting a complex interplay between nutritional factors and drug-induced gut damage.
NSAIDs and Food-Induced Anaphylaxis: A Growing Concern
The link between NSAID use and compromised intestinal integrity may also shed light on the increased risk of severe allergic reactions to food. NSAID medications, including aspirin, ibuprofen, and naproxen, have been implicated in up to 25% of food-induced anaphylaxis cases. This association suggests that these drugs may be linked to over a tenfold increase in the odds of life-threatening food allergy attacks. The prevailing hypothesis is that by increasing intestinal permeability, NSAIDs allow tiny food particles, which would normally be processed without issue, to enter the bloodstream. Once in circulation, these food particles can trigger an exaggerated immune response in susceptible individuals, leading to anaphylaxis.

The Influence of Physical Activity and Alcohol
While often lauded for its health benefits, strenuous physical activity can, under certain circumstances, transiently impact intestinal barrier function. Prolonged or intense exercise, such as an hour at 70% of maximum capacity, can divert a significant volume of blood away from internal organs, including the intestines, to supply working muscles. This reduced blood flow can lead to temporary injury of the intestinal lining, resulting in mild gut leakiness. This effect can be further amplified if athletes concurrently use NSAIDs. The common practice of athletes consuming ibuprofen or other NSAIDs for pain management or recovery, therefore, presents a dual risk of exercise-induced gut stress compounded by drug-induced permeability.
Alcohol consumption also emerges as a potential risk factor for food allergy attacks, operating through a similar mechanism of increasing gut leakiness. By compromising the integrity of the intestinal barrier, alcohol can facilitate the entry of food components into the bloodstream, potentially triggering allergic responses. Conversely, abstaining from alcohol may offer a pathway for the gut to heal and restore its barrier function.
Dietary Fat: A Silent Culprit?
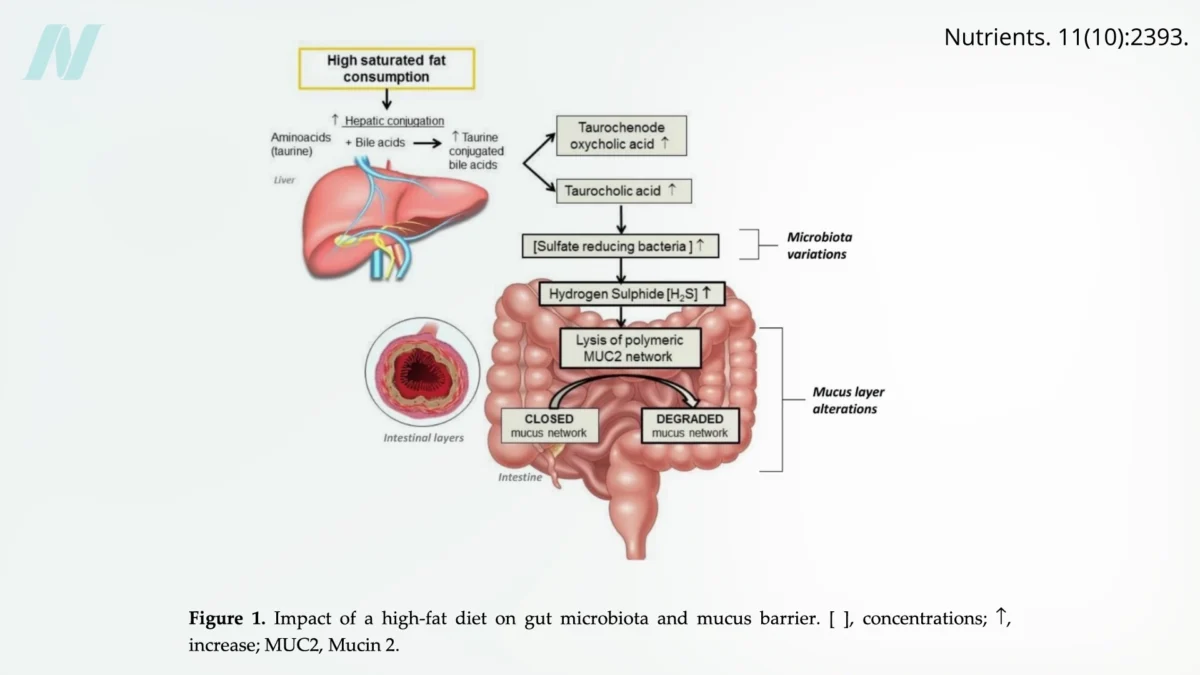
Beyond medications and alcohol, dietary patterns play a significant role in maintaining gut health. Elevated consumption of saturated fats, commonly found in red meat, dairy products, and processed "junk" foods, has been linked to an increase in the proliferation of certain gut bacteria. These bacteria can produce hydrogen sulfide, a gas with a rotten-egg odor, which has been shown to degrade the protective mucus layer that lines the gut. This mucus layer acts as a crucial physical barrier, preventing direct contact between gut contents and the epithelial cells of the intestinal wall.
While much of the research detailing the negative impact of high-fat diets on intestinal health has been conducted in laboratory animals or in vitro (in petri dishes), the implications for human health are increasingly being explored. There is a recognized need to translate these findings into human interventional studies to confirm the observed effects.
The parallel rise in obesity and other cardiometabolic disorders with the global dietary shift towards higher-fat consumption has prompted closer examination. Disturbances in the balance of beneficial gut flora (microbiome) have been strongly associated with an increased risk of these same diseases. Rodent studies suggest that high-fat diets can disrupt the gut microbiome and impair the gut barrier, leading to disease development.
Human Trials Illuminate the Impact of Dietary Fat
To bridge the gap between animal research and human understanding, a six-month randomized controlled feeding trial was conducted to investigate the effects of dietary fat on gut microbiota and barrier function in humans. This study provided compelling evidence that higher fat consumption was indeed associated with unfavorable alterations in the gut microbiome and increased levels of proinflammatory factors in the blood.
Importantly, this trial demonstrated these effects even when the dietary fat was not primarily saturated fat. Researchers simply replaced refined carbohydrates with refined fats, for example, by swapping white rice and wheat flour for soybean oil. The findings suggest that countries undergoing dietary transitions towards Westernized patterns should consider advising against increased dietary fat intake. Similarly, nations that have already adopted such diets may benefit from recommendations to reduce their fat consumption.
Broader Implications for Public Health
The growing body of evidence linking common lifestyle factors and dietary choices to compromised intestinal barrier function carries significant public health implications. The "leaky gut" theory is evolving from a niche concept to a recognized pathway for disease development and progression. Understanding these mechanisms can inform strategies for disease prevention, potentially mitigating the burden of chronic inflammatory diseases, autoimmune conditions, and even certain allergic disorders.
Future research is likely to focus on developing targeted interventions to restore and maintain intestinal barrier integrity. This could involve dietary modifications, the use of specific probiotics or prebiotics, or the development of novel therapeutic agents. The medical community’s increasing recognition of intestinal permeability as a key health indicator suggests a paradigm shift in how we approach chronic disease management and prevention.
Doctor’s Note on Gut Health
Further exploration into the complexities of gut health and the "leaky gut" phenomenon can be found in related resources. Discussions on the potential role of animal products in promoting inflammation through the "leaky gut" theory, and practical dietary strategies for healing a compromised gut barrier, offer valuable insights for individuals seeking to improve their digestive and overall well-being. Additionally, the relationship between gut leakiness and conditions like Small Intestinal Bacterial Overgrowth (SIBO) highlights the interconnectedness of the gastrointestinal system and the importance of a holistic approach to health.
The continuous advancement of scientific understanding underscores the profound impact of our daily choices – from the medications we take to the foods we eat and the beverages we consume – on the integrity of our intestinal barrier and, consequently, on our overall health.






