The persistent and often debilitating nature of arthritis, affecting an estimated 50 million Americans, continues to drive scientific inquiry into both conventional and alternative therapeutic approaches. Osteoarthritis of the knee, the most prevalent form of the condition and a leading contributor to disability, is characterized by complex inflammatory pathways. This has led researchers to explore the potential anti-inflammatory properties of various foods. While some foods, such as strawberries, have demonstrated an ability to reduce specific inflammatory mediators like tumor necrosis factor in the bloodstream, the direct translation of these findings into clinically significant symptom relief for patients with knee osteoarthritis has been met with mixed results.
For instance, studies involving cherry juice have shown a reduction in C-reactive protein, a marker of inflammation. However, in clinical trials assessing knee osteoarthritis, cherry juice failed to provide superior pain relief or symptom improvement compared to a placebo, leading to conclusions that its perceived benefits were largely subjective or attributable to the placebo effect rather than direct therapeutic action. While cherries may offer some benefit for other forms of arthritis, such as gout, their efficacy for osteoarthritis remains unsubstantiated by robust clinical evidence.
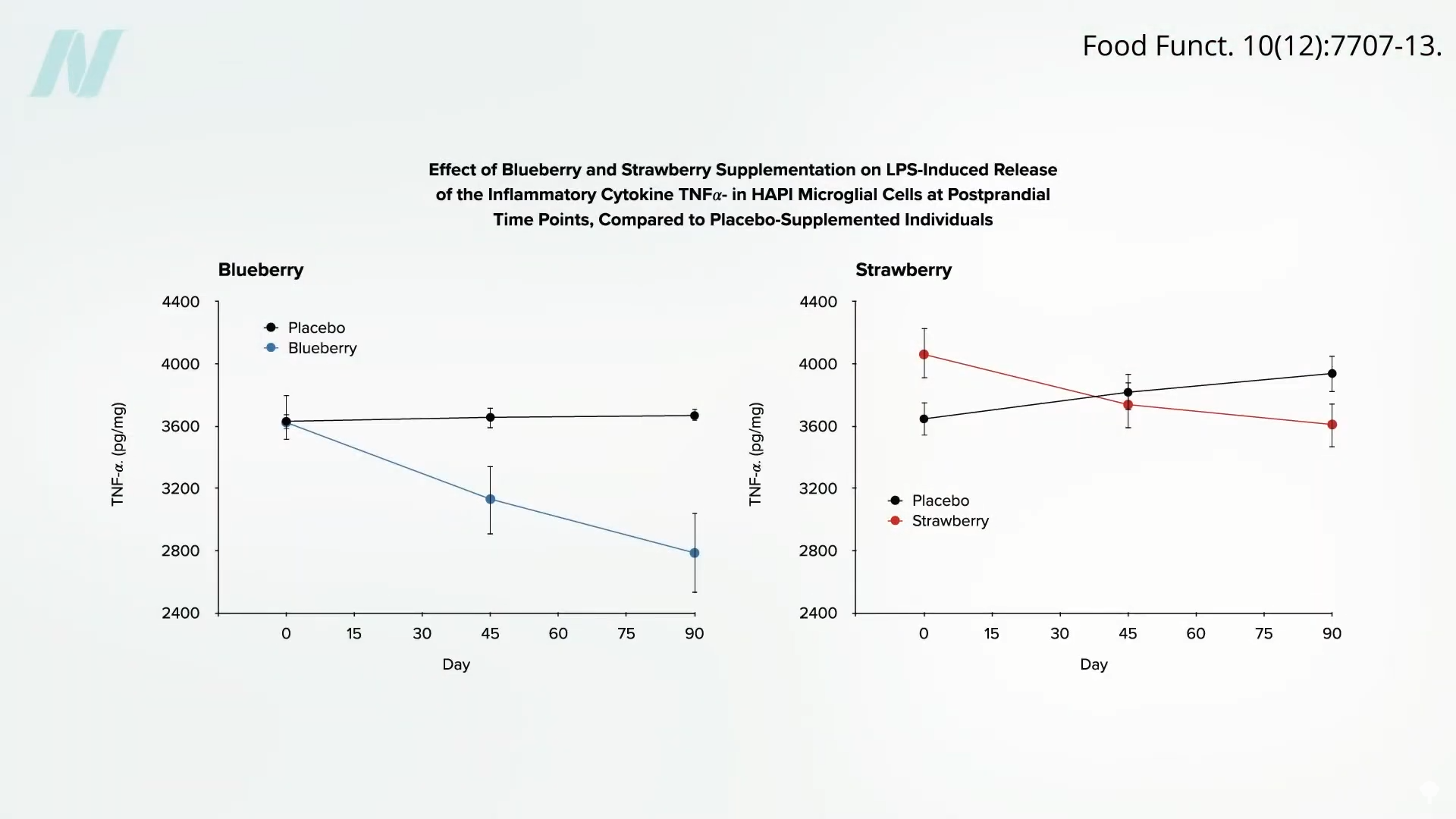
Conversely, research into the effects of strawberries has yielded more promising outcomes. A randomized, double-blind, crossover trial indicated that dietary consumption of strawberries led to a significant decrease in inflammation. Crucially, this study also reported a significant analgesic effect, translating to a noticeable reduction in pain for participants. This finding is particularly noteworthy when contrasted with the high cost and potential severe side effects associated with some pharmaceutical interventions. For example, tumor necrosis factor inhibitor drugs, while available, come with an annual price tag of approximately $40,000, and can carry serious risks, including potentially fatal lymphomas. The appeal of a natural, affordable alternative like strawberries, which demonstrably reduces inflammation and pain, becomes increasingly significant in this context.
Further investigation into the mechanisms behind berry consumption revealed that when individuals consumed the equivalent of one cup of blueberries or two cups of strawberries daily, their blood plasma, when applied to cells in laboratory settings, exhibited a marked reduction in inflammatory markers compared to plasma from individuals who consumed placebo berries. This in vitro evidence suggests a direct anti-inflammatory impact. Notably, the observed anti-inflammatory effect appeared to intensify over time, hinting at a cumulative benefit from sustained berry consumption. This observation prompts further exploration into other dietary components that might elicit similar sustained anti-inflammatory responses.

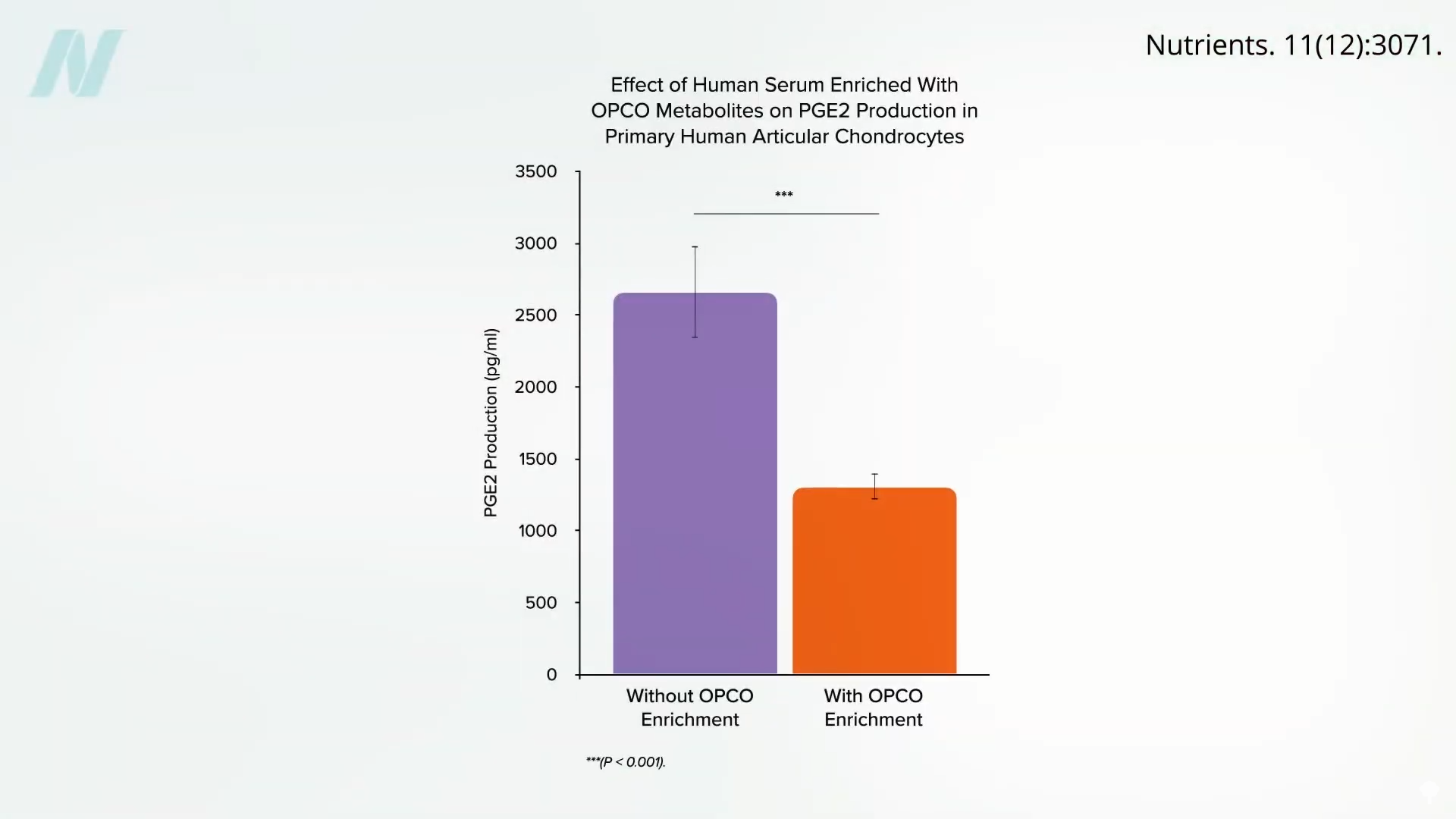
Exploring other natural compounds, researchers in France investigated the effects of grapeseed and olive extracts on cartilage explants obtained from knee replacement surgeries. When these cartilage samples were exposed to blood from volunteers who had consumed a substantial dose of these extracts, a significant reduction in inflammation was observed. While human studies specifically examining grapeseeds for arthritis are limited, an olive extract demonstrated a positive impact on pain reduction and improvement in daily activities for individuals with osteoarthritis.
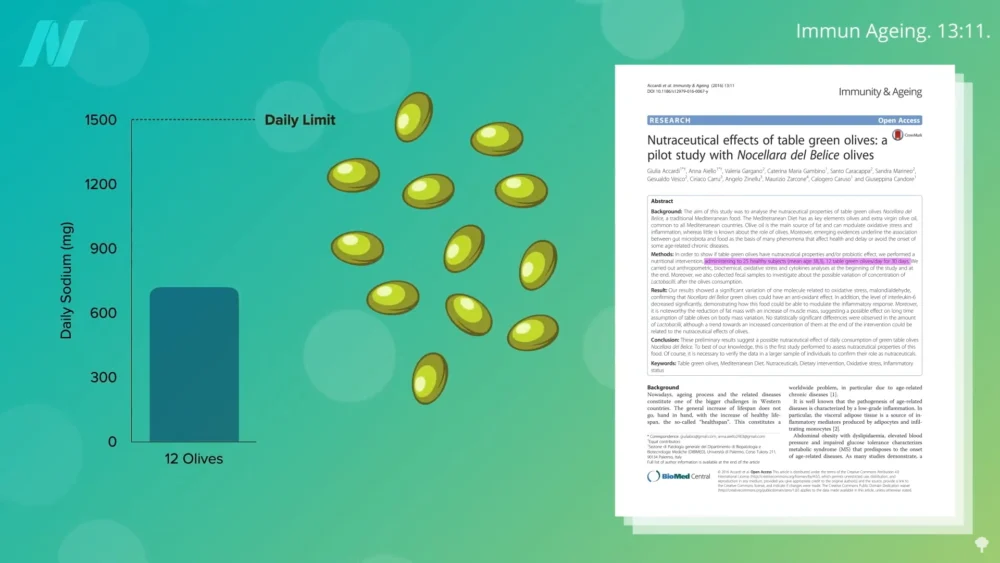
However, a critical distinction emerged regarding olive oil. The promising results observed with olive extracts were attributed to freeze-dried olive vegetation water, which contains water-soluble components of the olive – elements often absent in refined olive oil. This highlights that the beneficial compounds are not necessarily the oil itself but rather other constituents of the olive plant. Consuming whole olives, for example, has been linked to a decrease in inflammatory mediators. In contrast, systematic reviews and meta-analyses suggest that olive oil, when consumed orally, does not appear to offer significant anti-inflammatory benefits for arthritis. Claims of "remarkable anti-inflammatory activity" attributed to extra virgin olive oil in some studies are often based on rodent models, and human trials indicate that its effect on inflammation may be comparable to butter and even less effective than coconut oil.
The high sodium content of whole olives presents a dietary challenge, as consuming a dozen large green olives can account for nearly half of the recommended daily sodium intake. This limitation further complicates the notion of relying solely on whole olives for arthritis management.
While oral consumption of olive oil has shown limited benefits for arthritis, its topical application has emerged as a subject of significant interest. Previous research indicated that extra virgin olive oil did not significantly alleviate fibromyalgia symptoms, though it did demonstrate superior efficacy to canola oil in managing symptoms of inflammatory bowel disease. The absence of direct studies on oral olive oil intake for arthritis was a notable gap in the literature, leading to questions about the title of a research inquiry: "Can Olive Oil Compete with Arthritis Drugs?" The answer, it appears, lies in its topical application.
Topical Application: A Promising Avenue
A pivotal randomized, double-blind, clinical trial directly compared the efficacy of topical virgin olive oil with a gel containing an ibuprofen-type drug for osteoarthritis of the knee. In this study, a small quantity of olive oil – just one gram, equivalent to less than a quarter teaspoon, applied three times daily – proved to be remarkably effective. The cost of this topical application was minimal, amounting to less than three cents per day. The results were striking: topical olive oil demonstrated statistically significant superiority over the ibuprofen-type gel in reducing pain levels experienced by participants. This finding suggests that the mechanism of action for olive oil in pain relief might be localized and distinct from its effects when ingested.
The clinical trial, which lasted for one month, provided compelling evidence for the efficacy of topical olive oil. The observed improvements in pain reduction raise the question of whether these benefits might continue to accrue with longer-term application. Future research could explore the sustained effects of topical olive oil over extended periods to fully understand its potential as a chronic pain management strategy.
Rheumatoid Arthritis and Topical Olive Oil
Further investigation extended to the realm of rheumatoid arthritis, a systemic autoimmune disease characterized by inflammation of the joints. A study specifically examined the effectiveness of topical extra virgin olive oil in managing morning inflammatory pain in the fingers and knees of women diagnosed with rheumatoid arthritis. The research design was comprehensive, comparing the application of extra virgin olive oil against a control group that applied no substance and another group that used the standard ibuprofen-type gel. The findings indicated a notable decrease in disease activity scores in the group that utilized extra virgin olive oil topically, outperforming both the no-treatment control and the ibuprofen gel. This suggests that topical olive oil may offer a viable alternative or adjunct therapy for managing inflammatory pain associated with rheumatoid arthritis.
Analysis and Implications
The findings regarding topical olive oil present a significant development in the search for accessible and effective arthritis management strategies. The demonstrated efficacy of topical olive oil in reducing pain and disease activity in both osteoarthritis and rheumatoid arthritis, particularly when compared to conventional NSAID gels, warrants further attention. The low cost and minimal side effects associated with topical olive oil make it an attractive option for a broad range of patients, especially those seeking natural remedies or who experience adverse reactions to oral medications.
The distinction between the efficacy of ingested olive oil and its topical application is crucial. While oral consumption has shown limited direct anti-inflammatory benefits for arthritis, the localized application appears to target inflammatory processes effectively. This suggests that the beneficial compounds in olive oil may exert their effects through direct interaction with inflamed joint tissues when applied topically.
The research underscores the importance of considering different modes of administration when evaluating the therapeutic potential of natural compounds. What may not be effective when ingested could prove highly beneficial when applied locally. This paradigm shift could encourage further exploration of topical applications for other natural substances with known anti-inflammatory properties.
The implications of these findings extend to healthcare providers and patients alike. For healthcare professionals, this research provides a potential non-pharmacological option to recommend to patients suffering from joint pain and inflammation. For patients, it offers a cost-effective, readily available, and potentially safer alternative to manage their conditions, complementing existing treatment plans.
Future Directions
While the current evidence is encouraging, further research is warranted to fully elucidate the mechanisms by which topical olive oil exerts its anti-inflammatory and analgesic effects. Investigating the specific compounds within olive oil responsible for these benefits and understanding their interactions with joint tissues at a molecular level could lead to more targeted therapies. Long-term studies are also necessary to confirm the sustained efficacy and safety of topical olive oil application for arthritis management over extended periods. Additionally, comparative studies with a wider range of conventional arthritis medications and other topical treatments would provide a more comprehensive understanding of olive oil’s place in the therapeutic landscape. The growing body of evidence suggests that topical olive oil is not merely an anecdotal remedy but a scientifically supported intervention with the potential to significantly improve the quality of life for millions suffering from arthritis.






