The landscape of weight management and its profound impact on type 2 diabetes is undergoing rigorous re-evaluation, particularly concerning the efficacy and underlying mechanisms of bariatric surgery. While surgical interventions have long been lauded for their dramatic results in diabetes remission, emerging research suggests that the benefits may not be solely attributable to anatomical alterations. Instead, a growing body of evidence points to the potent metabolic effects of severe caloric restriction, a component often intrinsically linked to bariatric procedures. This comprehensive analysis delves into the complexities of this debate, exploring the scientific findings, the evolving terminology within the medical community, and the broader implications for patient care.
The Shifting Paradigm: From Bariatric to Metabolic Surgery
The surgical community has actively sought to reframe the perception of bariatric surgery, moving away from descriptions that imply drastic, potentially unnecessary alterations of healthy organs. Terms like "internal jaw wiring" or "cutting into healthy organs" are contested, with proponents advocating for the designation of "metabolic surgery." This shift in nomenclature underscores a key argument: that the anatomical rearrangements inherent in these procedures induce significant changes in digestive hormones, thereby offering unique physiological benefits that extend beyond mere weight reduction.
Historically, bariatric surgery, encompassing procedures such as gastric bypass, gastric banding, and sleeve gastrectomy, has been a cornerstone in managing severe obesity. These interventions fundamentally alter the digestive tract, influencing food intake, nutrient absorption, and hormonal signaling. For individuals struggling with obesity-related comorbidities, particularly type 2 diabetes, the results have often been nothing short of remarkable.
Remarkable Remission Rates: A Surgical Success Story?
The statistics surrounding bariatric surgery and type 2 diabetes remission are compelling. Studies have indicated that approximately 50% of obese individuals with diabetes, and an impressive 75% of those categorized as "super-obese" with diabetes, experience remission. Remission, in this context, signifies the normalization of blood sugar levels to a point where diabetes medication is no longer required, all while adhering to a regular diet. This normalization can occur with astonishing speed, sometimes within days of the surgical procedure. Long-term follow-up studies further bolster these findings, with data suggesting that around 30% of patients remain diabetes-free 15 years post-surgery. This contrasts sharply with a significantly lower remission rate of approximately 7% observed in non-surgical control groups over similar timeframes.
These impressive figures have led many to attribute the diabetes reversal directly to the surgical intervention itself, positing that the anatomical changes trigger a cascade of beneficial hormonal shifts. However, a critical question has emerged: to what extent are these outcomes driven by the surgery versus the drastic dietary interventions that typically accompany it?
Unpacking the Role of Caloric Restriction
A crucial aspect of preparing for and recovering from bariatric surgery involves stringent dietary protocols. Patients are often placed on extremely low-calorie diets, sometimes less than 500 calories per day, for weeks both before and after the procedure. This dietary regimen is not merely about reducing overall intake; it is designed to achieve rapid weight loss, which can have significant physiological consequences, particularly for organs affected by obesity, such as the liver.

Obese individuals frequently present with enlarged, fatty livers. This condition poses surgical challenges, increasing the risk of liver injury and bleeding during procedures. An enlarged liver can necessitate a transition from less invasive laparoscopic techniques to more extensive open surgery, resulting in larger scars, increased risk of wound infections, and prolonged recovery. However, even a modest weight loss of just 5% of body weight can lead to a notable reduction in liver fat, by as much as 10%. This pre-operative dietary intervention, therefore, plays a vital role in optimizing patients for surgery and mitigating surgical risks.
The question then arises: could the observed improvements in blood sugar levels following bariatric surgery be a direct consequence of this severe caloric restriction, rather than a unique metabolic benefit conferred by the surgical alterations alone? This hypothesis led researchers to design studies aimed at dissecting the contributions of surgery versus diet.
The University of Texas Study: A Controlled Comparison
To address this critical question, researchers at a bariatric surgery clinic at the University of Texas embarked on a meticulously designed study. Patients scheduled for gastric bypass surgery who also had type 2 diabetes volunteered for a controlled experiment. In the first phase, these patients remained hospitalized for 10 days and adhered to the same extremely low-calorie diet (less than 500 calories per day) that they would typically follow pre- and post-surgery, but without undergoing the surgical procedure itself.
After a period of several months, during which the patients regained the weight lost during the initial diet, they then underwent the actual gastric bypass surgery. Crucially, they repeated the same low-calorie diet, matched day-for-day with their initial dietary phase. This innovative design allowed researchers to directly compare the effects of caloric restriction with and without the surgical intervention, utilizing the same patients and the same diet. The core principle was to isolate the variable of surgery to determine if the anatomical rearrangement provided any additional metabolic advantage beyond what diet alone could achieve.
Surprising Findings: Diet Outperforms Surgery in Key Metrics
The results of this controlled study yielded unexpected and significant findings. Contrary to the prevailing assumption that anatomical rearrangement was the primary driver of metabolic improvement, the data revealed that caloric restriction alone was responsible for substantial improvements in blood sugar levels, pancreatic function, and insulin sensitivity.
Moreover, several key measures of diabetic control actually improved more significantly in the group that underwent caloric restriction without surgery. In some aspects, the surgical intervention appeared to place patients at a metabolic disadvantage compared to their non-surgical dietary counterparts. This suggests that the dramatic improvements previously attributed solely to bariatric surgery might be largely mediated by the profound metabolic shifts induced by severe calorie deprivation.
The Biological Pathway: Fat Mobilization and Insulin Sensitivity
The mechanism by which caloric restriction exerts its powerful effects on type 2 diabetes is rooted in the mobilization of fat from key organs. Type 2 diabetes is widely understood to be linked to the accumulation of excess fat in the liver, which then spills over into other organs like the pancreas. This "personal fat threshold" concept posits that individuals have a limit to how much fat they can safely store. When this limit is exceeded, fat infiltrates the liver, leading to insulin resistance.
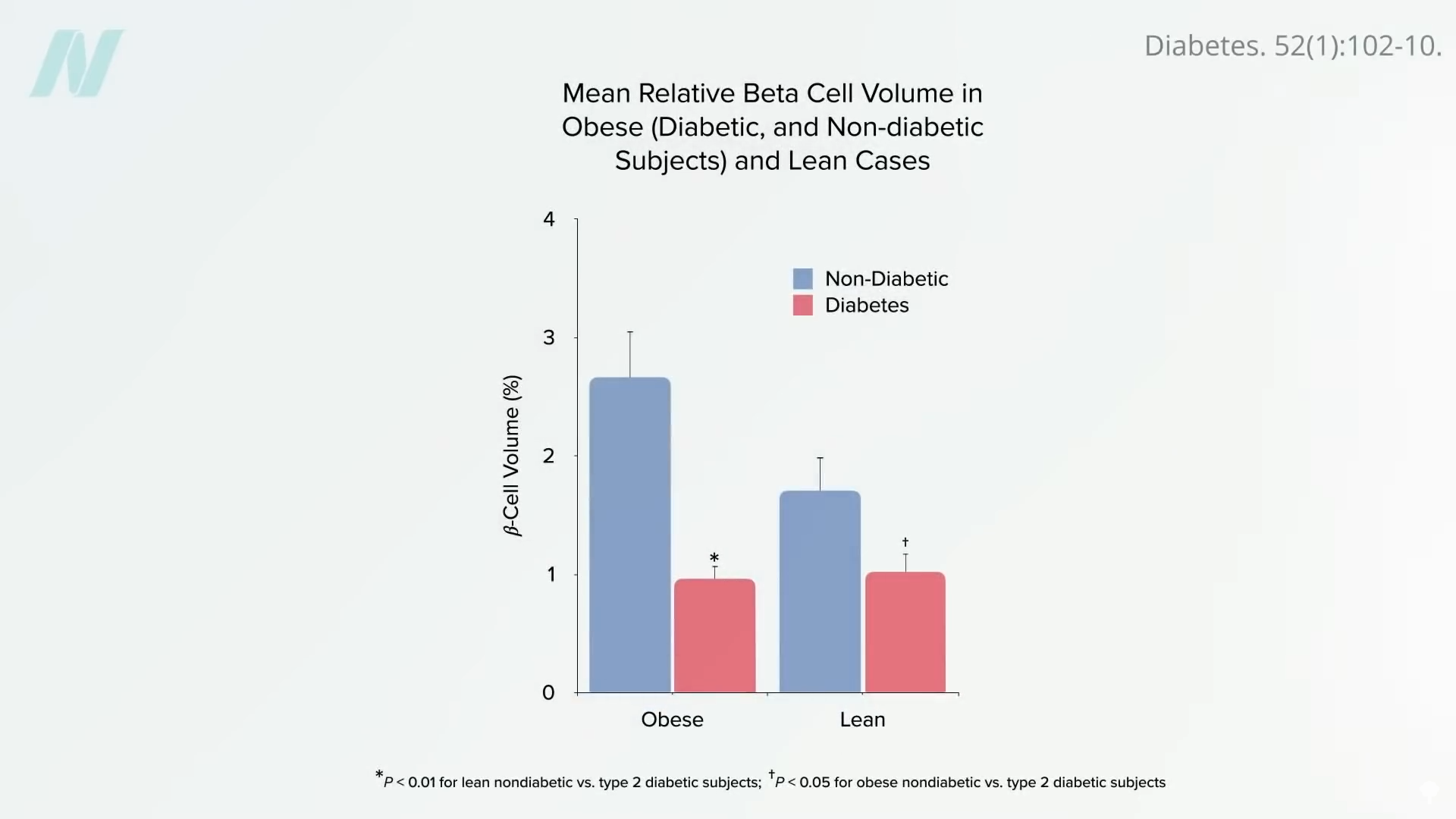
The liver, in an attempt to offload this excess fat, releases fat transport molecules (VLDL) into the bloodstream. These molecules can then accumulate in the pancreas, a vital organ responsible for producing insulin, the hormone that regulates blood sugar. This pancreatic fat accumulation can damage or even destroy the insulin-producing beta cells. By the time type 2 diabetes is diagnosed, it is estimated that as much as half of these crucial insulin-producing cells may have already been destroyed.
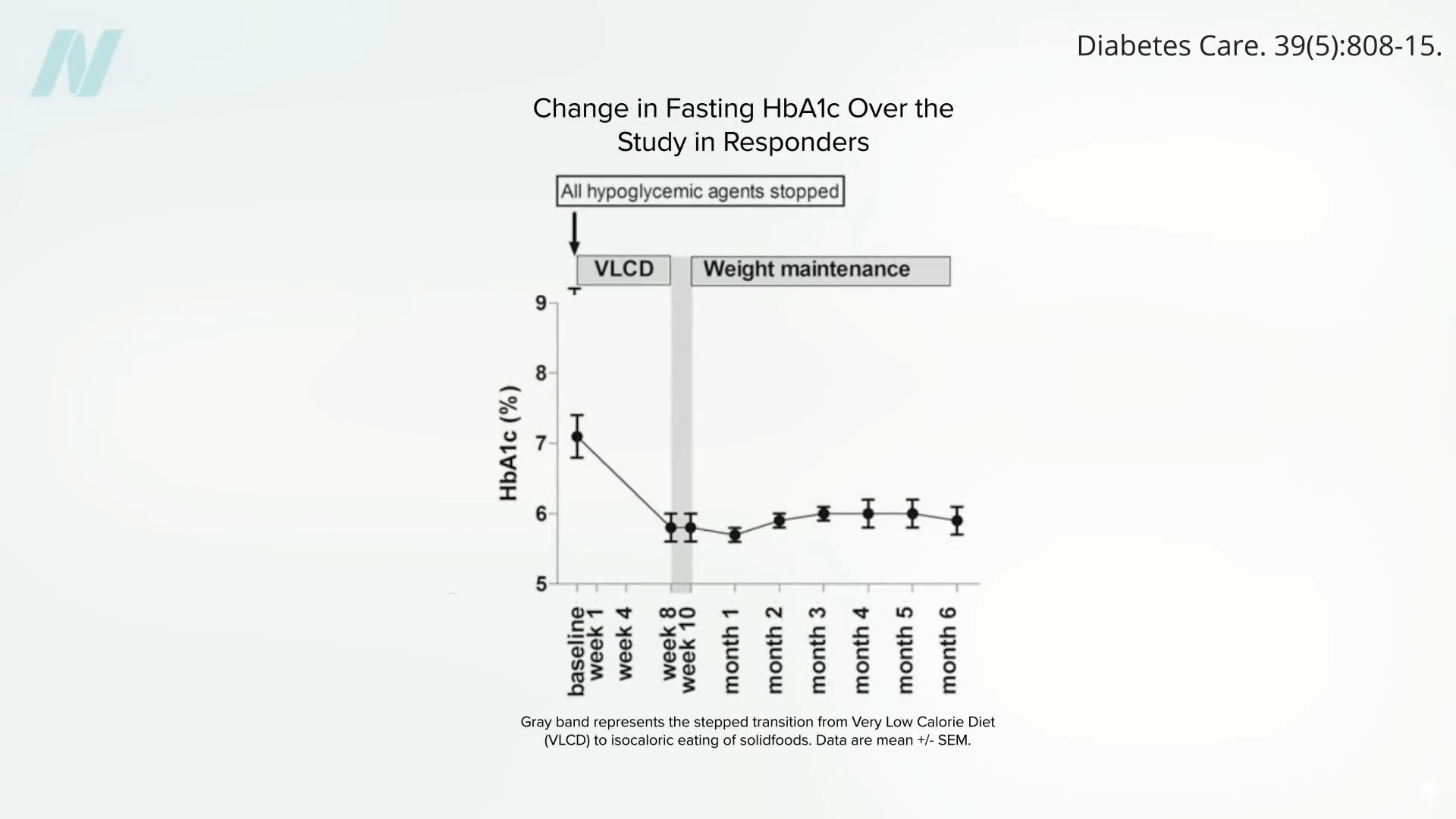
However, the body’s capacity for reversal through caloric restriction is remarkable. A significant calorie deficit can trigger a profound drop in liver fat within a matter of days, leading to a resurgence of liver insulin sensitivity. Sustained caloric restriction can further reduce liver fat to the point where pancreatic fat levels and function begin to normalize, often within eight weeks. Once an individual drops below their personal fat threshold, they may be able to resume a normal caloric intake and maintain their diabetes remission.
Broader Implications for Weight Loss and Diabetes Management
The implications of these findings are far-reaching for how we approach weight loss and the management of type 2 diabetes. While bariatric surgery undeniably offers significant benefits for many, particularly those with severe obesity and multiple comorbidities, the research highlights the potent therapeutic power of diet-induced weight loss.
Dietary Intervention: A Powerful Alternative
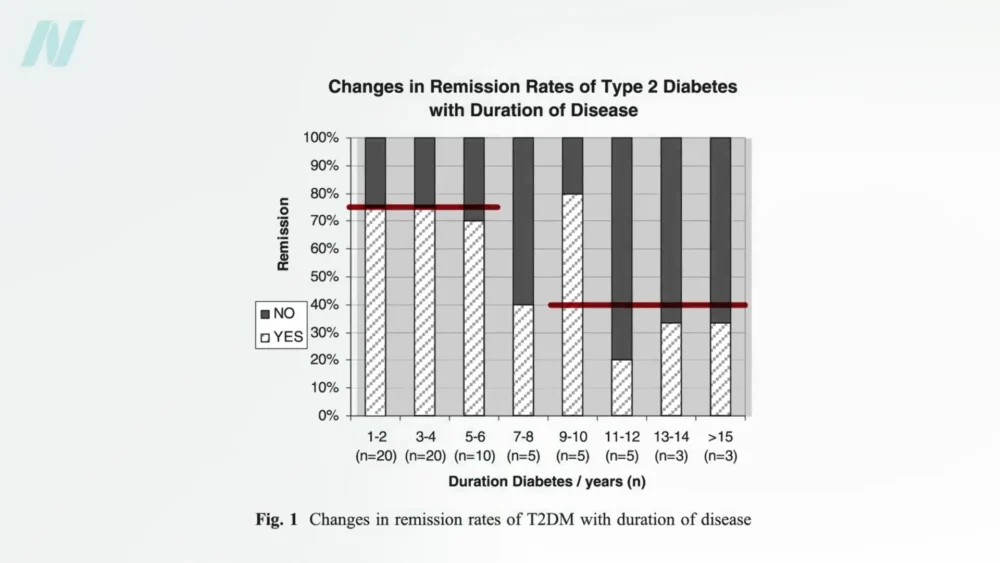
Losing a substantial amount of weight through diet alone can lead to significant improvements in blood sugar control. Studies suggest that individuals who lose more than 30 pounds (approximately 13.6 kilograms) through dietary means and have had type 2 diabetes for less than four years have a nearly 90% chance of achieving non-diabetic blood sugar levels, indicating remission. This contrasts with a lower remission rate of approximately 50% for those who have lived with the disease for eight or more years.
Conversely, even with bariatric surgery, which often results in greater weight loss, the remission rates for diabetes may not always surpass those achieved through intensive dietary intervention, especially in individuals with longer-standing diabetes. For instance, individuals with diabetes for up to six years may see around 75% remission rates with surgery, while those with diabetes for longer periods may experience only about 40% remission.
Systemic Inflammation and Diabetic Complications
Beyond blood sugar control, weight loss achieved through diet alone has also demonstrated the ability to significantly improve markers of systemic inflammation, such as tumor necrosis factor. In contrast, studies have shown that when a similar amount of weight is lost via gastric bypass, these inflammatory markers can actually worsen. This suggests that the quality of the diet and the metabolic state achieved through non-surgical weight loss might be more beneficial in mitigating systemic inflammation.
The impact on long-term diabetic complications, such as blindness and kidney failure requiring dialysis, is also a critical consideration. While reversing diabetes through bariatric surgery can lead to improvements in kidney function, surprisingly, it may not effectively prevent the onset or progression of diabetic vision loss. This phenomenon could be attributed to the fact that bariatric surgery primarily affects the quantity of food consumed, rather than necessarily influencing the quality of dietary choices that contribute to long-term health.
This observation echoes findings from large-scale studies, such as one published in The New England Journal of Medicine, which randomized thousands of individuals with diabetes to an intensive lifestyle program focused on weight loss. After a decade, the study was halted prematurely because participants did not exhibit longer lifespans or a reduction in heart attacks. A potential explanation for this outcome is that participants, while consuming smaller portions, continued to adhere to diets high in heart-clogging components. This underscores the critical importance of dietary composition, not just caloric intake, in managing chronic diseases.
Conclusion: A Nuanced Approach to Weight Management and Diabetes
The ongoing debate surrounding bariatric surgery versus dietary interventions for type 2 diabetes underscores the complexity of metabolic health. While bariatric surgery remains a powerful tool for significant weight loss and can lead to remarkable diabetes remission, emerging evidence strongly suggests that severe caloric restriction plays a pivotal role in these outcomes. The distinction between "metabolic surgery" and purely anatomical alteration is crucial, as it prompts a deeper understanding of the underlying physiological mechanisms at play.
For patients considering weight loss interventions, particularly those with type 2 diabetes, a nuanced approach is paramount. This involves a thorough understanding of the risks and benefits associated with both surgical and non-surgical pathways, with a particular emphasis on the potent metabolic effects of dietary changes. The scientific community’s ongoing exploration into these areas promises to refine treatment strategies, ultimately empowering individuals to achieve sustainable health and well-being.
Doctor’s Note: This analysis is part of a series examining the multifaceted aspects of bariatric surgery. Previous installments have explored "The Mortality Rate of Bariatric Weight-Loss Surgery" and "The Complications of Bariatric Weight-Loss Surgery." Further exploration into sustainable weight loss can be found in the book How Not to Diet.






