The alarming global rise in type 2 diabetes, a condition currently affecting over half a billion adults and projected to increase by 50% within a generation, is prompting a re-examination of effective treatment strategies. Emerging research indicates that significant weight loss, specifically a 15% reduction in body weight, may offer a pathway to remission for a substantial majority of individuals diagnosed with type 2 diabetes within the last four years. This finding holds particular significance as it suggests a powerful, non-pharmacological approach to managing and potentially reversing a chronic disease that places a considerable burden on individuals and healthcare systems worldwide.
The Historical Context of Weight Management in Diabetes Treatment
The concept of managing diabetes through dietary restriction and weight reduction is not a modern revelation. Historical accounts reveal a long-standing understanding of the link between excess body weight and the manifestation of diabetes. Early observations, dating back centuries, suggested that a significant reduction in food intake, often to the point of near starvation, could halt the progression of diabetes and alleviate its symptoms.
One of the earliest documented proposals for managing diabetes through extreme dietary measures comes from an Ayurvedic text, offering a stark perspective: "Poor diabetic people’s medicine. He should live like a saint (Munni); He should walk for 800–900 miles. Or he shall dig a pond; Or he shall live only on cow dung and cow urine." While these methods are clearly archaic and unscientific by today’s standards, they underscore a fundamental, albeit extreme, recognition that reducing caloric intake was central to managing the disease.
A more structured, though still challenging, approach emerged in the late 18th century with Dr. Rollo’s diet for diabetes in 1797. This regimen, unfortunately, involved the consumption of rancid meat and emetics to induce vomiting, highlighting a historical tendency to associate relief with inducing sickness, which effectively reduced food consumption. The diet’s inclusion of congealed blood and spoiled meat, while unpalatable and dangerous, achieved its intended effect by drastically limiting caloric intake.
The siege of Paris during the Franco-Prussian War provided further anecdotal evidence. During this period of extreme food scarcity, individuals with diabetes experienced improved health, leading to the widely adopted advice to "mangez le moins possible," or "eat as little as possible." This observation was later formalized into the Allen starvation treatment, pioneered by Dr. Frederick Madison Allen in the early 20th century. Considered a major advancement before the discovery of insulin, "The Allen Era" emphasized severe caloric restriction as the primary therapeutic intervention.
Dr. Allen’s Pioneering Work and the Concept of Fat Toxicity
Dr. Allen’s research was driven by his observation that many severe diabetes cases saw remission following the onset of wasting diseases like tuberculosis or cancer. He hypothesized that the severe caloric deficit associated with these illnesses was the key factor. Through rigorous testing, he demonstrated that even in the most severe forms of diabetes, blood sugar levels could be normalized within days by drastically reducing food intake.
Allen’s treatment principles were twofold: maintaining an underweight status for patients and strictly restricting dietary fat. He noted that while symptoms could be alleviated temporarily, the reintroduction of dietary fats, such as butter or olive oil, could rapidly trigger a resurgence of diabetic symptoms. This early observation foreshadowed the modern understanding of diabetes as a disease linked to fat accumulation.
Contemporary research has solidified the connection between dietary fat and the development of insulin resistance, a hallmark of type 2 diabetes. Studies have shown that infusing fat intravenously can lead to rapid fat accumulation in muscle cells, significantly increasing insulin resistance within hours. Similarly, high-fat diets, even for short durations of three days, or a single high-fat meal, can acutely impair insulin sensitivity.
This phenomenon is critical because insulin resistance in muscle tissue, particularly when combined with excessive calorie intake, can lead to a cascade of metabolic dysfunctions. Fat begins to accumulate in the liver, a condition known as non-alcoholic fatty liver disease (NAFLD), which further exacerbates insulin resistance. Subsequently, fat can infiltrate the pancreas, impairing the function of insulin-producing beta cells. This gradual deterioration culminates in the clinical diagnosis of type 2 diabetes. As researchers now understand, "Type 2 diabetes can now be understood as a state of excess fat in the liver and pancreas, and remains reversible for at least 10 years in most individuals."

The Mechanism of Remission: Weight Loss and Fat Mobilization
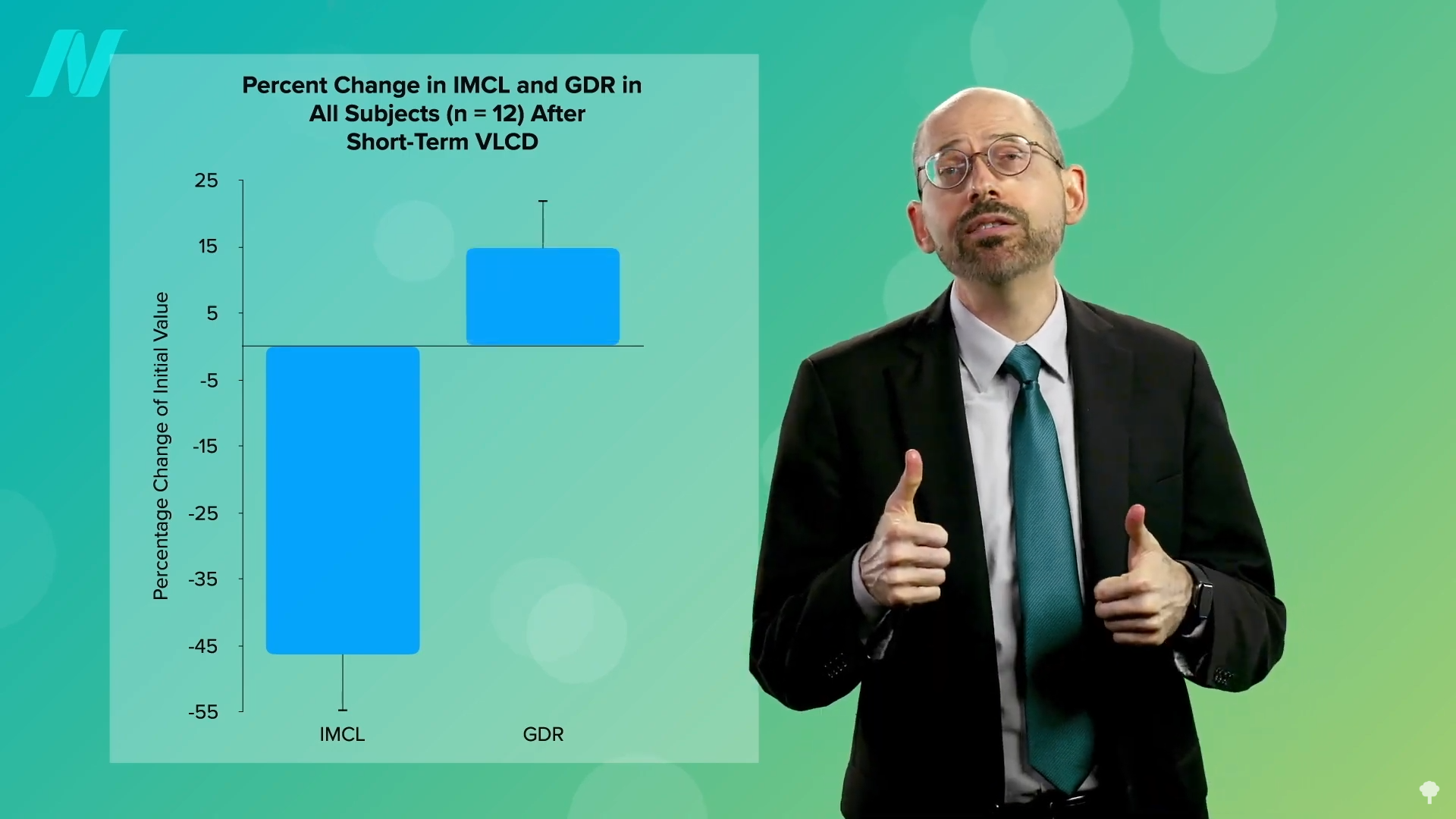
The breakthrough in understanding how weight loss leads to diabetes remission lies in the body’s ability to mobilize stored fat. When individuals are placed on very low-calorie diets, such as 700 calories per day, the body begins to access its fat reserves. This process directly impacts the fat accumulation in muscle cells, leading to a significant improvement in insulin sensitivity.
Scientific imaging techniques, including high-tech MRI scanners, have visually demonstrated this phenomenon in real-time. Studies using very low-calorie diets have shown a marked reduction in the fat content within muscle cells, directly correlating with enhanced insulin sensitivity. This reduction in intramuscular fat is a crucial step in reversing insulin resistance.
Furthermore, prolonged caloric restriction has been shown to decrease fat accumulation in the liver. As the diet continues and excess fat is mobilized, the pancreas also benefits from reduced fat infiltration, allowing its beta cells to regain function. If caught early enough in its progression, this reversal of fat accumulation can lead to sustained healthy blood sugar levels, effectively putting type 2 diabetes into remission without the need for medication.
Quantifying the Impact: Weight Loss Thresholds for Remission
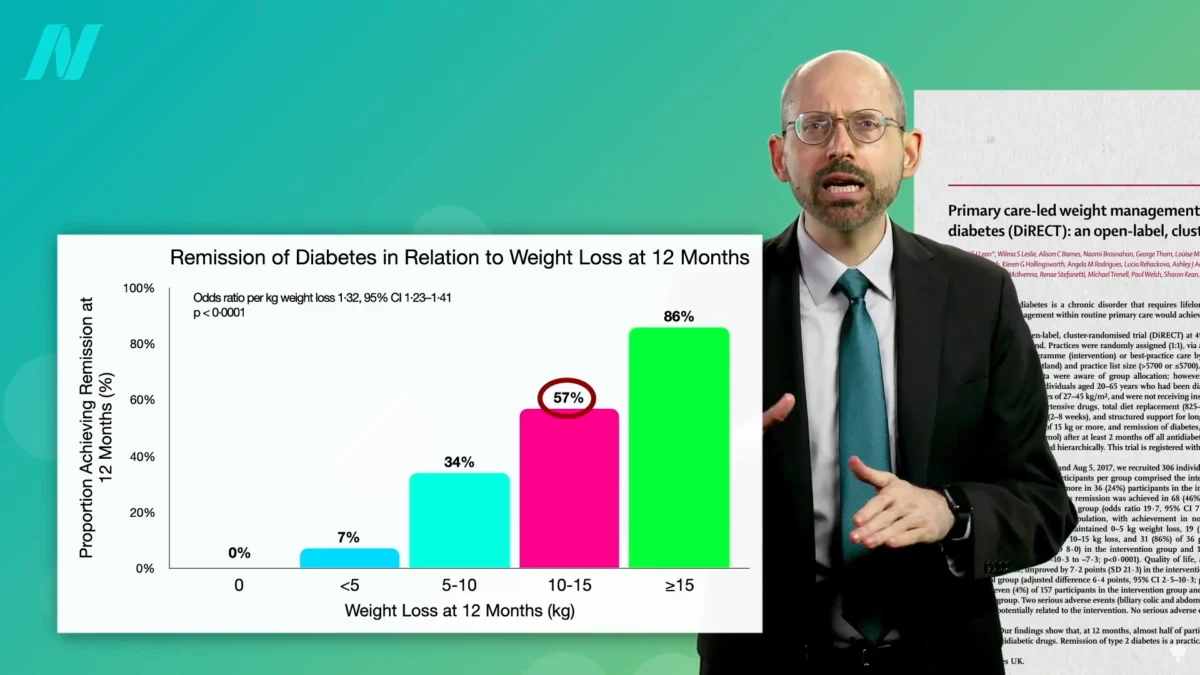
Recent studies have provided concrete data on the amount of weight loss required for diabetes remission. The most compelling findings indicate that a loss of approximately 15% of body weight can lead to non-diabetic blood sugar levels in nearly 90% of individuals diagnosed with type 2 diabetes within the past four years. This suggests a critical window of opportunity for intervention, where the disease is more responsive to lifestyle changes.
The effectiveness of weight loss as a treatment for type 2 diabetes appears to be time-dependent. For individuals who have lived with the disease for longer than eight years, the remission rates drop to approximately 50%, even with comparable weight loss. This highlights the progressive nature of the disease and the importance of early intervention.
Comparative Efficacy: Weight Loss vs. Bariatric Surgery
Remarkably, the remission rates achieved through significant weight loss through diet and lifestyle interventions can surpass those of bariatric surgery, a procedure often considered the gold standard for substantial weight reduction in cases of severe obesity. Studies have shown that while bariatric surgery can lead to significant weight loss, remission rates for type 2 diabetes following surgery are lower than those observed with successful dietary interventions. For instance, patients undergoing bariatric surgery may experience remission rates of around 62% in individuals losing more weight, compared to the nearly 90% observed with a 15% body weight reduction through lifestyle changes. This suggests that the mechanism of fat reduction and metabolic reset achieved through dietary means is highly potent.
Evidence further indicates that individuals who have had type 2 diabetes for an average of three years can achieve remission after losing approximately 30 pounds. This substantial, yet achievable, weight loss through dietary adjustments and exercise offers a powerful alternative or complementary strategy to medical interventions. The adage that "your forks are better than surgeons’ knives" gains significant weight when considering these outcomes.
Maintaining Remission: The Crucial Role of Sustained Lifestyle Changes
While achieving remission is a significant milestone, maintaining it requires sustained commitment to a healthy lifestyle. The historical data and modern research both underscore a critical point: weight regain is strongly linked to the recurrence of diabetes. If individuals regain the lost weight, their diabetes is likely to return.
Physician-supervised, water-only fasting regimens have also demonstrated the potential to induce diabetes remission. However, the long-term success of such extreme interventions hinges on the individual’s ability to maintain the achieved weight loss. This reinforces the idea that the underlying metabolic improvements are tied to sustained lower body weight and reduced fat accumulation.
The Evolution of Diabetes Management: Beyond Insulin
The discovery of insulin in 1921 was a monumental achievement, revolutionizing the treatment of type 1 diabetes and saving countless lives. However, for individuals with type 2 diabetes, insulin alone, while essential for survival and symptom management, has proven insufficient in preventing long-term complications such as blindness, kidney failure, stroke, and amputations.
This realization led pioneers in diabetes care, such as Elliott Joslin, to advocate for a return to the foundational principles of diet and exercise management that were central to diabetes care before the widespread availability of insulin. Joslin argued that self-discipline in diet and exercise should remain a cornerstone of managing type 2 diabetes, even in the era of pharmacological advancements. His perspective highlights a continuous tension in diabetes management: the immediate relief provided by medication versus the long-term, potentially curative, power of fundamental lifestyle changes.
Implications and Future Directions
The growing body of evidence supporting the role of weight loss in type 2 diabetes remission has profound implications for public health policy, clinical practice, and individual patient empowerment. It suggests a paradigm shift towards prioritizing preventative and lifestyle-based interventions.
Public Health Implications:
The global prevalence of type 2 diabetes necessitates scalable and effective interventions. Focusing on weight management strategies, such as promoting healthy eating patterns and regular physical activity, could significantly reduce the incidence and burden of the disease. This requires public health campaigns that educate individuals about the link between weight and diabetes and provide accessible resources for weight loss and management.
Clinical Practice:
Healthcare providers are increasingly encouraged to incorporate comprehensive weight management programs into their treatment plans for patients with type 2 diabetes. This includes thorough patient education, motivational interviewing, and referrals to registered dietitians and certified diabetes educators. The emphasis is shifting from solely managing blood sugar levels with medication to addressing the root causes of the disease.
Individual Empowerment:
The findings offer a message of hope and agency to individuals living with type 2 diabetes. It underscores that remission is not only possible but achievable through significant, yet attainable, lifestyle modifications. Empowering individuals with the knowledge and tools to take control of their weight can lead to significant improvements in their health and quality of life.
Further Research:
Continued research is crucial to understand the long-term sustainability of diabetes remission achieved through weight loss, identify personalized approaches for different patient populations, and explore the optimal timing and intensity of interventions. Understanding the specific metabolic pathways involved in fat mobilization and insulin sensitivity could lead to even more targeted and effective treatments.
In conclusion, the scientific community’s understanding of type 2 diabetes is evolving, moving beyond a singular focus on blood sugar control to a more holistic view that recognizes the disease as a metabolic disorder often reversible through substantial weight loss. The historical journey from starvation diets to modern, evidence-based weight management strategies illustrates a consistent thread: the power of the body to heal itself when provided with the right conditions, primarily achieved through fundamental changes in diet and lifestyle. The potential for nearly 90% remission in early-stage type 2 diabetes with a 15% body weight reduction represents a significant beacon of hope in the ongoing battle against this global health crisis.
Doctor’s Note: For a deeper understanding of the underlying causes of type 2 diabetes, the video "Diabetes as a Disease of Fat Toxicity" is recommended. Further exploration of fasting for disease reversal can be found in related resources. It is important to note that while fasting can be a component of weight loss strategies, it is not universally the most effective method for weight loss. For comprehensive guidance on optimal weight loss and disease prevention, the video "Friday Favorites: The Best Diet for Weight Loss and Disease Prevention" offers valuable insights.






