The stark contrast between the efficacy of healthy lifestyle choices and pharmaceutical interventions in preventing heart attacks is a critical public health revelation. While medications may offer a modest reduction in risk, a comprehensive shift towards a healthier lifestyle has the potential to mitigate up to 90% of heart attack risk. This significant disparity underscores the urgent need to address the root causes of cardiovascular disease, which, alarmingly, begin in adolescence.
The Silent Onset of Arterial Hardening
Atherosclerosis, the progressive hardening and narrowing of the arteries, stands as the leading cause of mortality for both men and women globally. Disturbingly, research indicates that the foundational stages of this disease, known as fatty streaks, can commence as early as the teenage years, particularly for individuals adhering to the standard American diet.
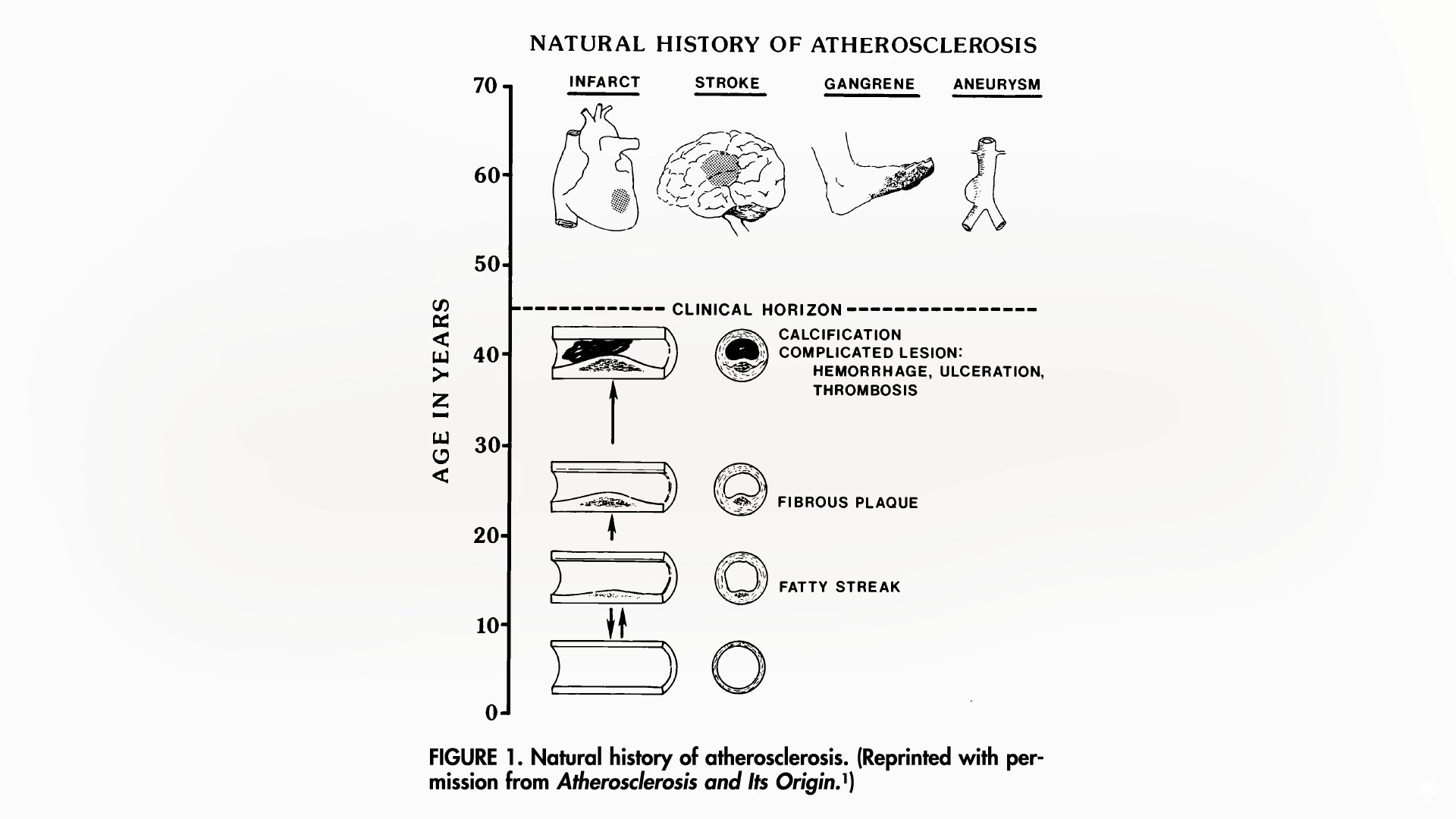
A groundbreaking study involving the examination of approximately 3,000 coronary arteries and aortas from individuals aged 15 to 34, who tragically succumbed to accidents, homicides, and suicides, provided compelling evidence of this early onset. The findings revealed that fatty streaks, the initial precursors to atherosclerotic plaques, are prevalent in adolescents. By their twenties, these streaks transform into more established plaques, which continue to develop and worsen through the thirties, significantly increasing the risk of life-threatening events such as heart attacks and strokes. The progression of this disease can be visualized, demonstrating how these arterial changes begin subtly and escalate over time, impacting major blood vessels that supply vital organs like the heart and brain.

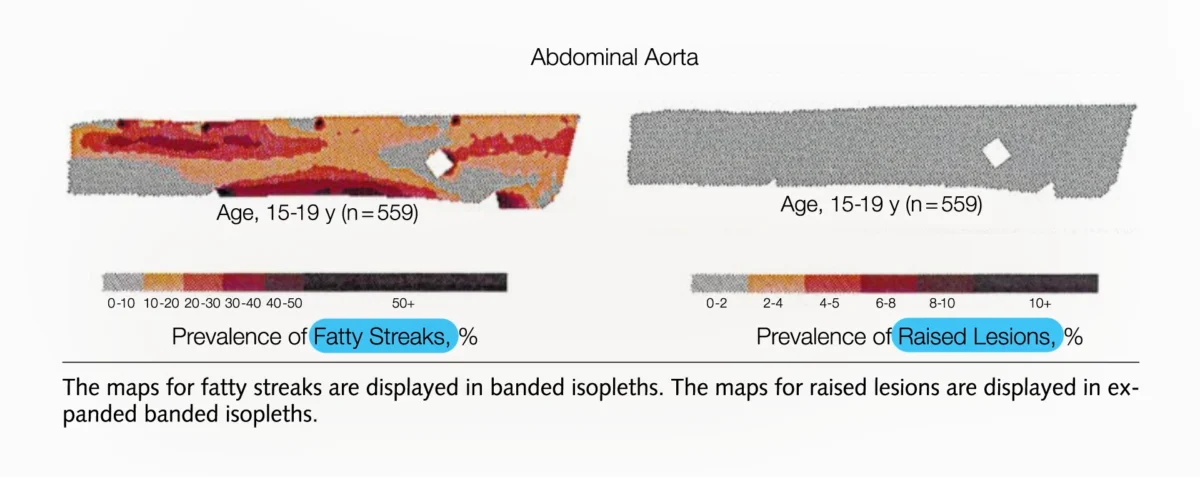
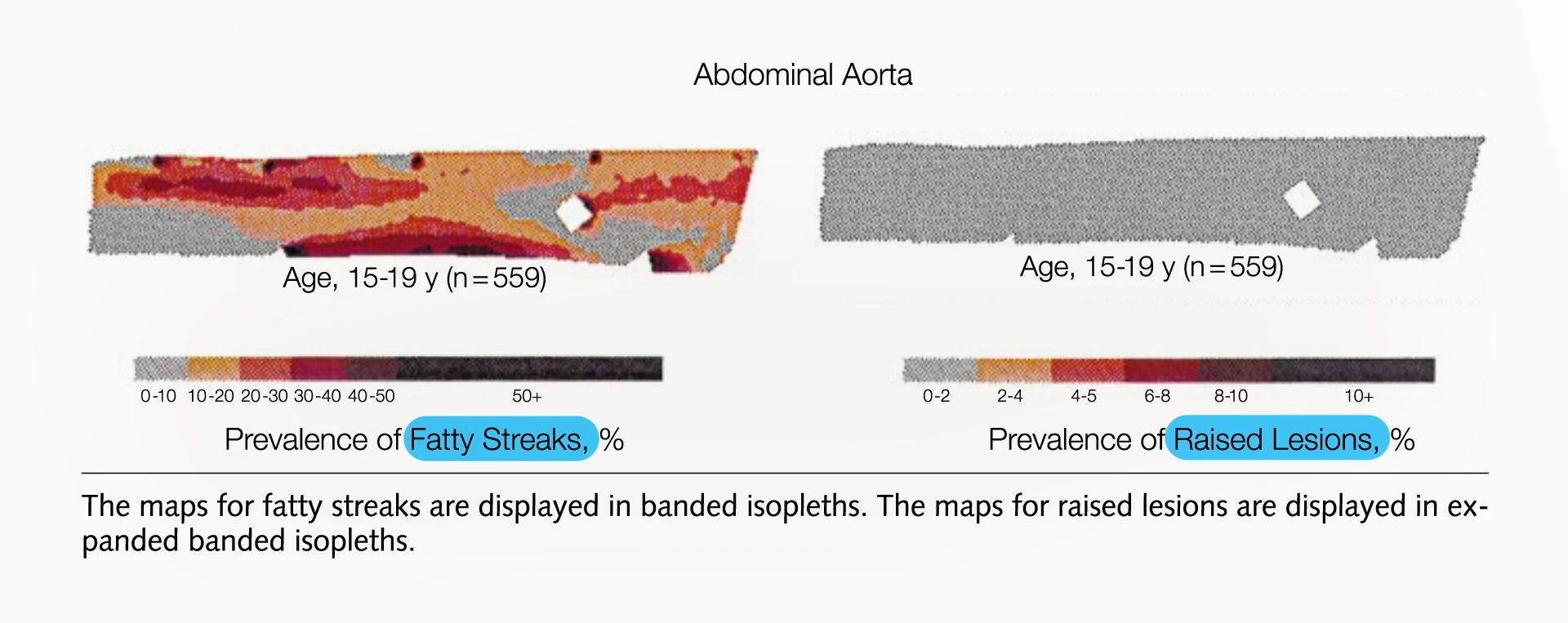
The pervasiveness of this early arterial damage is staggering. In the studied cohort, 100% of the teenagers exhibited fatty streaks within their arteries. By their early thirties, a majority had progressed to developing atherosclerotic plaques that encroached upon the arterial lumen. The research meticulously documented this progression, showing that while fatty streaks were widespread throughout the aortas of teenagers (ages 15-19), established plaques were not yet the norm. However, this shifted rapidly.
A Timeline of Arterial Degradation
The timeline of atherosclerosis development, as revealed by scientific inquiry, paints a concerning picture:
- Adolescence (15-19 years): The initial formation of fatty streaks begins in the arteries. In the abdominal aorta, these fatty streaks are present, but significant plaque buildup is not yet evident.
- Early Twenties: The abdominal aorta starts to show the emergence of atherosclerotic plaques. Fatty streaks continue to be present.
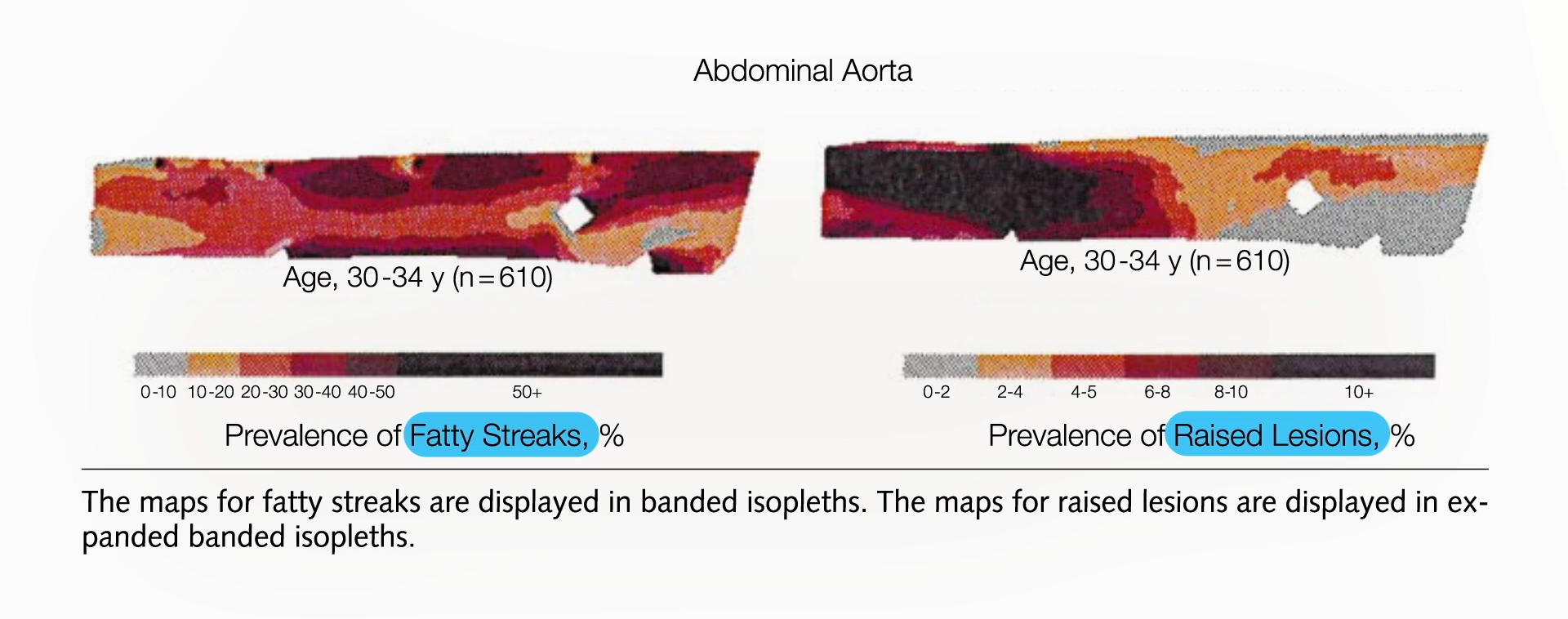
- Late Twenties: Plaques become more pronounced in the abdominal aorta, and fatty streaks have infiltrated more extensively.
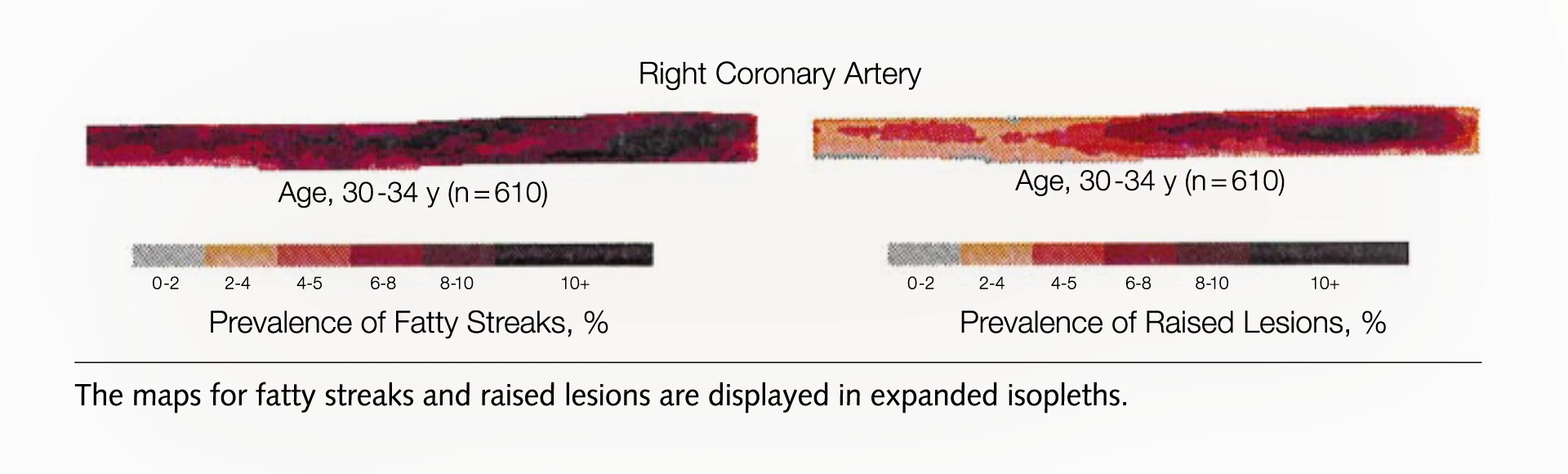
- Early Thirties: Arteries, including the coronary arteries supplying the heart, are significantly affected. Most individuals in this age group exhibit established plaques in their coronary arteries, mirroring the progression observed in the abdominal aorta.
This detailed chronological mapping of arterial disease underscores that by the time individuals reach their thirties, their vascular system may already be compromised, setting the stage for future cardiovascular events. The implications are profound: delaying intervention until symptoms manifest is a strategy fraught with risk, as the underlying disease has likely been developing for decades.
The Power of Prevention: Lifestyle vs. Pharmaceuticals
The disparity in risk reduction between lifestyle interventions and drug therapies is a critical point of discussion in cardiovascular health. While statin medications, commonly prescribed to lower LDL cholesterol, can reduce the risk of heart attacks by approximately 20% to 30%, adopting a heart-healthy lifestyle has demonstrated the capacity to eliminate up to 90% of this risk.
Understanding the Mechanism of Action
The key to this dramatic difference lies in the duration and totality of intervention. Atherosclerosis is a chronic disease that develops over a lifetime. Lifestyle changes, such as adopting a diet low in saturated fat and cholesterol—meaning a reduction in the consumption of eggs, meat, dairy, and processed junk foods—effectively lower LDL cholesterol levels naturally and sustainably. This approach addresses the fundamental drivers of plaque formation and progression.
Conversely, medications, while beneficial, often act as a later-stage intervention. They may be necessary to manage existing disease or mitigate risk in individuals with established risk factors. However, relying solely on drugs to reverse decades of arterial damage can be less effective than preventing the damage from occurring in the first place.
The Role of Lifelong Low LDL Cholesterol
Evidence from genetic studies provides a powerful illustration of the long-term benefits of sustained low LDL cholesterol levels. Individuals born with a specific genetic mutation in the PCSK9 gene, which leads to approximately a 40% reduction in LDL cholesterol throughout their lives, exhibit dramatically lower rates of coronary heart disease. Studies have shown an 88% reduction in risk compared to individuals without this mutation, even when those individuals possess multiple other cardiovascular risk factors such as high blood pressure, obesity, smoking, and diabetes.
This near-90% reduction in heart attacks and sudden cardiac death occurred at an average LDL cholesterol level of around 100 mg/dL. This suggests that a lifelong maintenance of LDL cholesterol below this threshold, achieved through consistent healthy habits, can offer unparalleled protection.
The question then arises: why does a genetic reduction in LDL cholesterol by roughly 40 mg/dL lead to a nearly 90% decrease in cardiovascular risk, while a similar reduction achieved with statin drugs only yields a 20% to 30% decrease? The most compelling explanation points to the duration of these low cholesterol levels. A genetically determined lifelong low LDL cholesterol offers a sustained defense against arterial buildup, whereas drug-induced reductions, often initiated later in life, may not compensate for years of arterial exposure to higher cholesterol levels.
The Imperative for Early Intervention
The findings that atherosclerosis begins in adolescence present a clear imperative for early intervention. Waiting until heart disease becomes symptomatic is akin to treating a developing cancer only after it has metastasized. Just as one would not delay treatment for diabetes until blindness sets in, addressing atherosclerosis must commence proactively.
Primordial Prevention: A Radical Yet Practical Proposal
The concept of "primordial prevention," which aims to prevent the development of risk factors before they emerge, is not merely an academic ideal but a critical strategy for combating chronic diseases. Altering lifestyle choices, beginning in infancy or early childhood, is proposed as a means to stem the tide of atherosclerosis. While this may sound like a "radical proposal," the potential to eliminate our number one killer warrants serious consideration and commitment to behavioral change.
The success in reducing smoking rates and subsequent lung cancer incidence demonstrates that significant public health shifts are achievable. Similarly, embracing healthy eating habits, which are demonstrably safe and appropriate for all stages of life, including pregnancy, as affirmed by the Academy of Nutrition and Dietetics, is a feasible goal. This organization, a leading professional body in nutrition, recognizes plant-based diets as suitable for all life stages, underscoring the scientific backing for such dietary patterns.
The Goal of Curing Atherosclerosis
A significant study published in the Journal of the American College of Cardiology boldly declared that "Curing Atherosclerosis Should Be the Next Major Cardiovascular Prevention Goal." This ambitious objective hinges on the understanding that lifelong suppression of LDL cholesterol is paramount. The genetic evidence of PCSK9 mutation carriers strongly supports the idea that sustained low LDL cholesterol can lead to substantial risk reduction, even in the presence of other adverse risk factors.
Navigating Cholesterol Levels: Lifelong Habits vs. Later-Life Medications
The optimal LDL cholesterol target for preventing cardiovascular disease appears to be intrinsically linked to the duration of maintaining those levels.
Lifestyle-Driven Prevention
For individuals who adopt healthy lifestyle choices early in life, maintaining an LDL cholesterol level around 100 mg/dL may be sufficient to significantly reduce the risk of heart attacks. This level is generally achievable through dietary modifications and regular physical activity. Country-specific data has historically suggested that heart disease mortality rates tend to plateau at population averages around 100 mg/dL of LDL cholesterol, reinforcing the protective effect of consistently low levels.
Medication-Assisted Management
For those who have not consistently maintained a heart-healthy lifestyle, the landscape shifts. When medication is introduced later in life to halt the progression of coronary atherosclerosis, lower LDL cholesterol targets may be necessary. To arrest the disease’s advancement, LDL levels might need to fall below 70 mg/dL.
If an individual is attempting to counteract a lifetime of poor dietary habits with medication, the LDL cholesterol target to achieve zero coronary heart disease events could potentially be as low as 55 mg/dL. For patients who have already experienced a heart attack and are striving to prevent subsequent events, an aggressive LDL reduction to approximately 30 mg/dL is often considered ideal.
The Benefits of Extremely Low LDL
Achieving and maintaining such exceptionally low LDL cholesterol levels, around 30 mg/dL, offers profound benefits. Not only can it prevent the formation of new atherosclerotic plaques, but it can also stabilize existing plaques. This stabilization is crucial, as it reduces the likelihood of plaques rupturing, a primary trigger for heart attacks and strokes.
The question of whether such extremely low cholesterol levels are safe has been a subject of considerable scientific inquiry. While concerns have been raised in the past, the overwhelming evidence from individuals with genetic predispositions to lifelong low LDL cholesterol suggests that these levels can be maintained safely and effectively, providing significant protection against cardiovascular disease. Further exploration into the safety and efficacy of very low LDL cholesterol levels is ongoing, aiming to provide a comprehensive understanding of its implications for long-term health.
The battle against heart disease is a lifelong endeavor, and the evidence increasingly points to the transformative power of early, consistent, and comprehensive lifestyle interventions as the most potent weapon in our arsenal. While medications play a vital role in managing cardiovascular risk, they cannot fully replicate the profound and enduring protective benefits of a truly healthy lifestyle.






