The discourse surrounding weight loss interventions, particularly bariatric surgery, has undergone a significant evolution, moving beyond a purely anatomical perspective to embrace a more nuanced understanding of its metabolic implications. While the surgical community has historically advocated for bariatric procedures, often rebranding them as "metabolic surgery," recent research is prompting a critical re-evaluation of the primary drivers behind the observed benefits, particularly concerning type 2 diabetes remission. The advantages of non-surgical weight loss, such as dietary changes and caloric restriction, are increasingly being highlighted for their comparable, and in some aspects superior, outcomes without the inherent risks associated with invasive procedures.
The Promise and Peril of Metabolic Surgery
Bariatric surgery, encompassing procedures like gastric bypass, has long been lauded for its dramatic impact on obesity and its associated comorbidities, most notably type 2 diabetes. The surgical community has actively sought to reframe these interventions, moving away from descriptions that evoke drastic alterations of healthy organs, such as "internal jaw wiring" or "cutting into healthy organs," towards the more sophisticated term "metabolic surgery." This rebranding reflects a belief that the anatomical rearrangements inherent in these procedures trigger significant changes in digestive hormones, thereby offering unique physiological benefits that extend beyond mere weight reduction.
A cornerstone of this argument has been the remarkably high remission rates for type 2 diabetes observed post-bariatric surgery. Studies have indicated that approximately 50% of obese individuals with diabetes, and a striking 75% of those classified as "super-obese" with diabetes, achieve remission. This remission is characterized by the normalization of blood sugar levels, allowing patients to discontinue diabetes medications and maintain healthy glucose levels through a regular diet. In some instances, this normalization can occur with astonishing speed, sometimes within days of the surgery. Long-term follow-up data has also shown sustained benefits, with a significant percentage of patients remaining diabetes-free years after the procedure, outperforming non-surgical control groups.
However, a crucial question lingers: to what extent are these impressive outcomes attributable to the surgery itself, as opposed to the profound dietary changes that invariably accompany it? The surgical journey for bariatric procedures, especially for individuals with significant obesity, is often preceded and followed by stringent dietary protocols. For instance, a common pre-operative requirement involves a period of caloric restriction to reduce liver size. Obese individuals frequently present with enlarged, fatty livers, which can complicate surgical access and increase the risk of complications such as bleeding and liver injury. Lifting a significantly enlarged liver during surgery can necessitate a transition from minimally invasive laparoscopic techniques to more extensive open surgery, leading to larger scars, increased risk of wound infections, prolonged recovery, and a higher overall complication rate.

The strategic pre-operative diet, often involving an extremely low-calorie liquid regimen, aims to shrink the liver by as much as 10% with just a 5% reduction in body weight. This underscores the potent impact of caloric deficit on metabolic health. Similarly, post-surgery, patients are typically placed on very low-calorie diets for extended periods to facilitate healing and initial weight loss. This raises a critical hypothesis: could the observed improvements in blood sugar levels and diabetic control be primarily a consequence of this intensive caloric restriction, rather than a unique metabolic advantage conferred by the surgical alteration of the gastrointestinal tract?
Investigating the Caloric Restriction Factor: A Landmark Study
To disentangle the effects of surgical intervention from those of caloric restriction, researchers at a bariatric surgery clinic at the University of Texas designed a compelling study. Patients scheduled for gastric bypass surgery who also had type 2 diabetes were invited to participate. The study involved two phases, carefully matched to isolate variables.
In the first phase, these patients remained hospitalized for 10 days and adhered to the same extremely low-calorie diet (less than 500 calories per day) that they would have followed pre- and post-operatively, but without undergoing the surgical procedure. Following this initial period, they were discharged and allowed to regain the lost weight over a period of months. In the second phase, the same patients then underwent the actual gastric bypass surgery. Crucially, their post-operative dietary regimen was meticulously matched, day for day, to the caloric intake and composition of the diet they had followed during the non-surgical hospitalization period. This innovative design allowed researchers to directly compare the impact of caloric restriction both with and without the anatomical changes of bariatric surgery, using the same individuals as their own controls.
The findings of this study provided significant insights. While the immediate improvements in blood sugar levels, pancreatic function, and insulin sensitivity were comparable in both phases, several key measures of diabetic control actually showed greater improvement when patients relied solely on caloric restriction, without the surgery. In essence, the surgical intervention, in some respects, appeared to place patients at a metabolic disadvantage compared to the non-surgical caloric restriction group.
The Physiological Basis of Reversible Diabetes
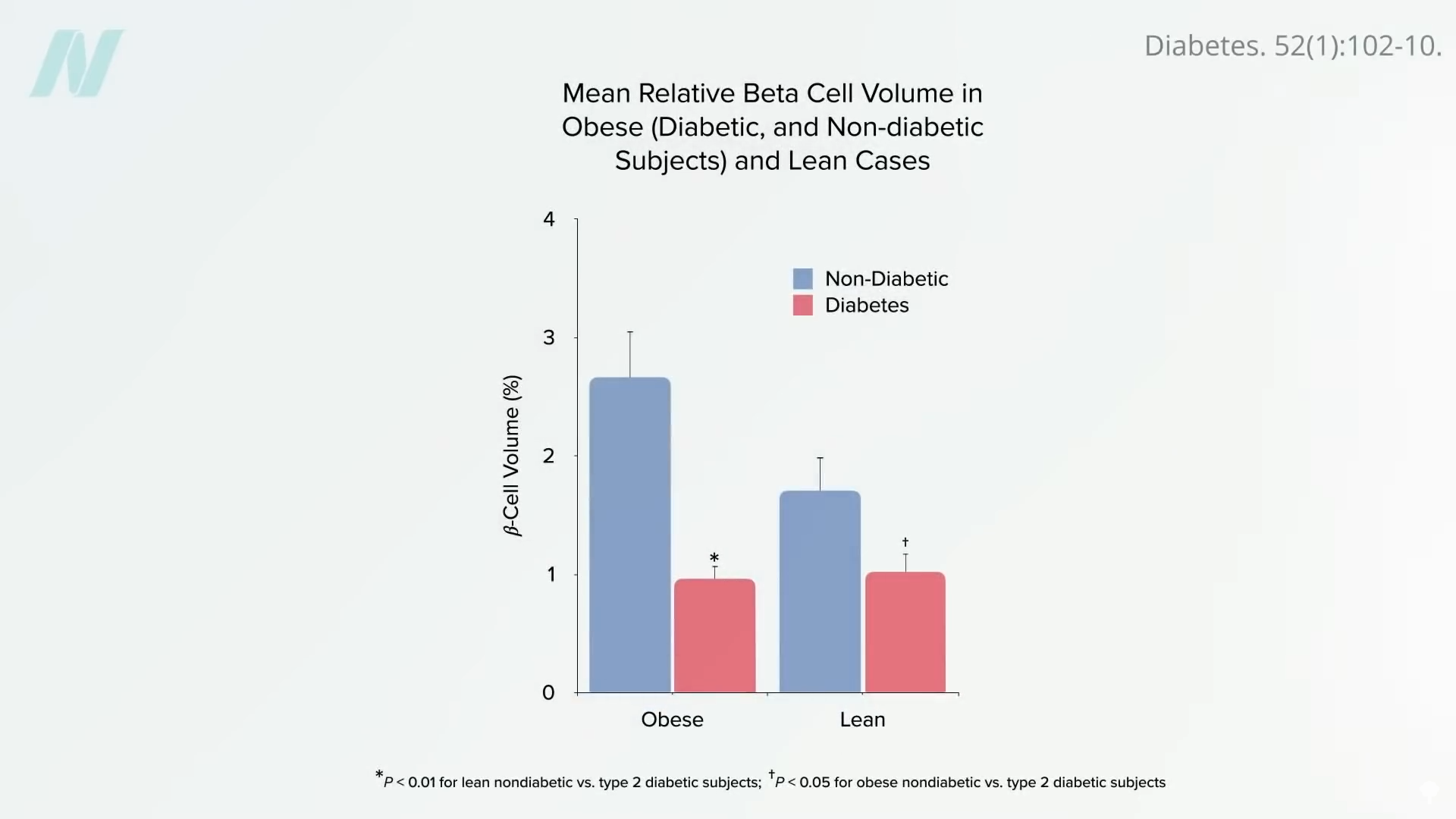
The prevailing scientific understanding of type 2 diabetes links its development to the accumulation of excess fat, particularly in the liver. When the liver becomes saturated with fat, it can lead to insulin resistance, a state where the body’s cells do not respond effectively to insulin. This fat accumulation can prompt the liver to offload excess lipids into the bloodstream in the form of very-low-density lipoproteins (VLDL). These circulating fats can then accumulate in the pancreas, where they are toxic to the insulin-producing beta cells. By the time type 2 diabetes is diagnosed, it is estimated that up to half of these vital insulin-producing cells may have already been destroyed.
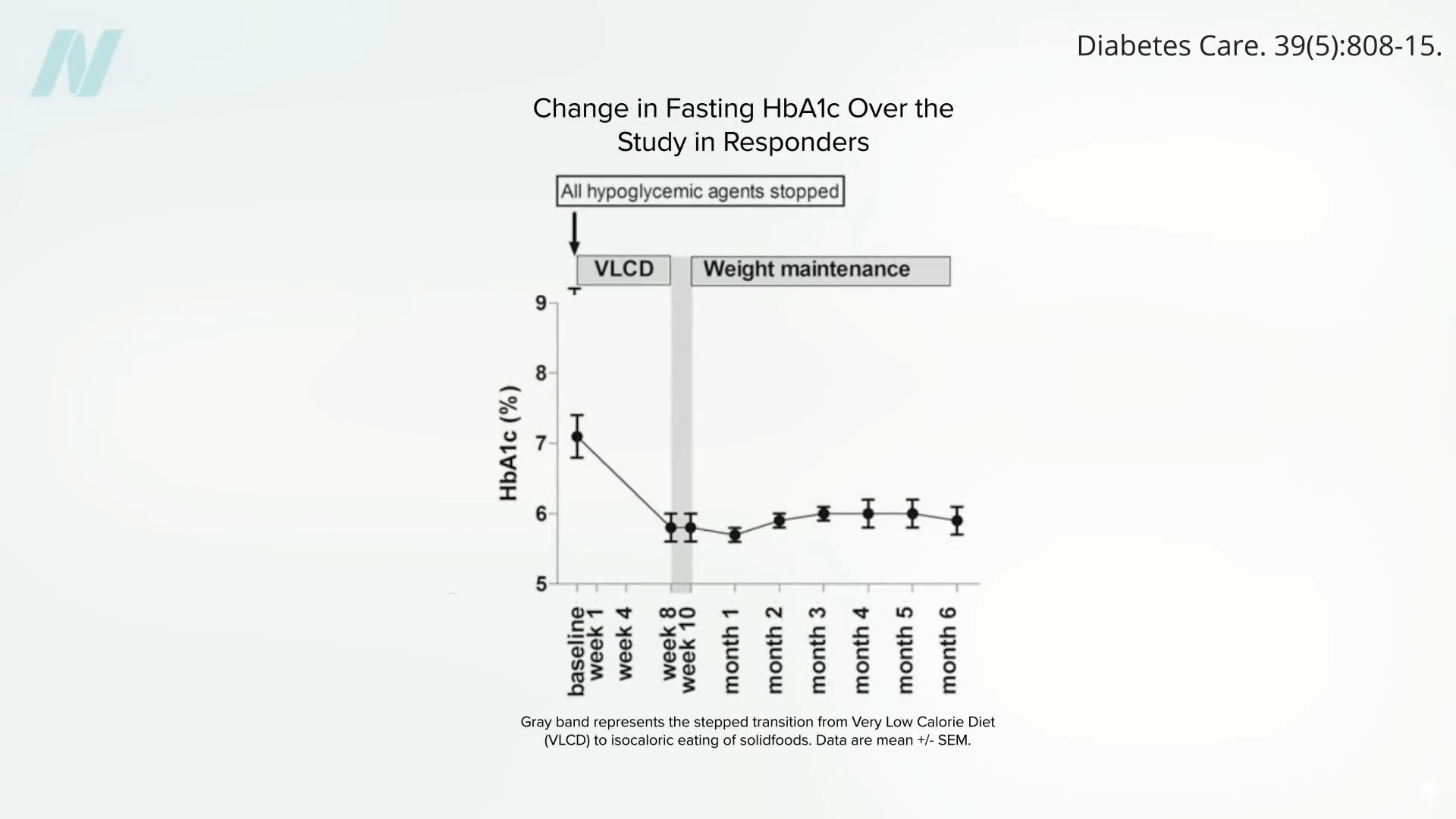
Caloric restriction offers a direct pathway to reversing this pathological process. By creating a significant calorie deficit, the body is compelled to mobilize stored fat. This process begins with a reduction in liver fat. Within a mere seven days of a substantial calorie deficit, liver insulin sensitivity can be resurrected as liver fat levels drop. Sustained caloric restriction over approximately eight weeks can lead to a normalization of pancreatic fat levels and improved pancreatic function.
The concept of a "personal fat threshold" is central to this understanding. Each individual has a limit for safely storing excess fat. Exceeding this threshold initiates the cascade of metabolic dysfunction leading to type 2 diabetes. Once this threshold is brought back down through significant weight loss, individuals can often resume a normal caloric intake and maintain their diabetes remission. This suggests that type 2 diabetes, when caught early enough, is a reversible condition, with the primary mechanism of reversal being the reduction of excess fat stores, particularly in the liver and pancreas.
Comparing Remission Rates: Diet vs. Surgery
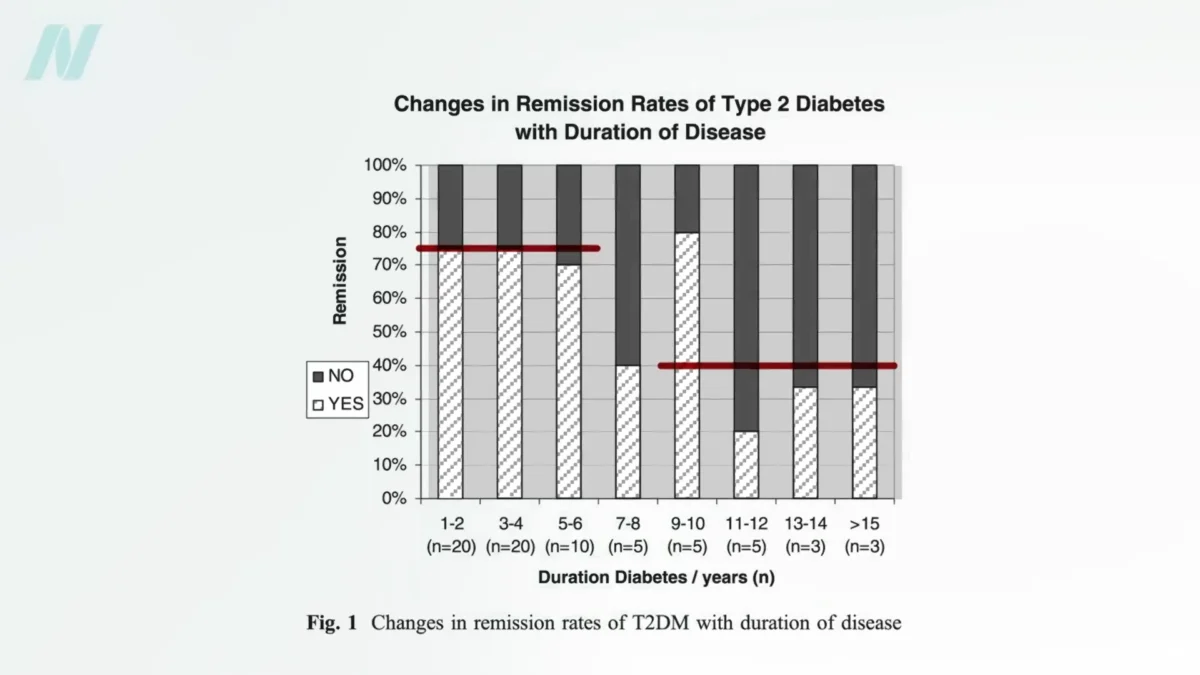
The data regarding diabetes remission rates further complicates the narrative that bariatric surgery is the sole or superior pathway to recovery. Studies indicate that weight loss achieved through diet alone can lead to significant improvements in blood sugar levels. For individuals who have had type 2 diabetes for less than four years, losing more than 30 pounds (approximately 13.6 kilograms) through dietary means can result in non-diabetic blood sugar levels in nearly 90% of cases, suggesting remission. However, for those who have lived with the disease for eight or more years, the remission rate through diet alone may decrease to around 50%.
In contrast, bariatric surgery, which often leads to more substantial weight loss, shows remission rates that, while high, are not always dramatically superior to diet-induced weight loss, particularly for longer-standing diabetes. For patients who have had diabetes for up to six years, bariatric surgery might yield a remission rate of around 75% after losing more than twice the weight compared to diet-only interventions. However, for those with diabetes of longer duration (eight years or more), the remission rate after bariatric surgery may only be around 40%. This suggests that while surgery can induce significant weight loss and improve remission rates, the duration of diabetes plays a critical role, and the absolute benefit of surgery over substantial dietary weight loss might be less pronounced than previously assumed, especially for those with more established disease.
Beyond Blood Sugar: Systemic Inflammation and Complications
The benefits of non-surgical weight loss extend beyond glycemic control. Individuals with diabetes who achieve weight loss through diet alone have demonstrated significant improvements in markers of systemic inflammation, such as tumor necrosis factor. Conversely, studies have shown that when a similar amount of weight is lost via bariatric surgery, these inflammatory markers can actually worsen. This highlights a potential advantage of lifestyle-based interventions in addressing the broader inflammatory milieu associated with obesity and diabetes.
Furthermore, the impact of these interventions on long-term diabetic complications warrants careful consideration. While reversing diabetes through bariatric surgery can improve kidney function, surprisingly, it may not always prevent the occurrence or progression of diabetic vision loss. This is a complex issue, and one hypothesis suggests that bariatric surgery might influence the quantity of food consumed but not necessarily the quality, a concept echoed in some large-scale studies. For instance, a landmark study published in The New England Journal of Medicine, which randomized thousands of individuals with diabetes to an intensive lifestyle program focused on weight loss, was stopped prematurely. After ten years, participants in the intensive lifestyle group did not exhibit increased longevity or a reduction in heart attacks compared to the control group. A potential explanation offered is that participants maintained their same "heart-clogging" dietary habits, albeit in smaller portions, thus failing to address the underlying dietary quality that contributes to cardiovascular risk.
Implications for Future Treatment Paradigms
The evolving research landscape prompts a recalibration of how bariatric surgery is perceived and utilized in the management of type 2 diabetes. While it remains a powerful tool for significant weight loss and can induce diabetes remission, the evidence increasingly suggests that the metabolic benefits are not solely or even primarily derived from the surgical alteration of the gastrointestinal anatomy. Instead, the profound caloric restriction inherent in both pre- and post-operative dietary regimens appears to be a major driver of physiological improvements.
This realization has significant implications for patient care and public health messaging. It underscores the critical importance of intensive dietary interventions as a primary therapeutic strategy for type 2 diabetes, potentially delaying or even obviating the need for surgery for many individuals, especially when diagnosed early. For those who do undergo bariatric surgery, a thorough understanding of the synergistic role of dietary adherence is paramount to maximizing long-term health outcomes and mitigating potential complications.
The medical community continues to grapple with these findings, seeking to refine treatment protocols and patient selection criteria. The focus is shifting towards personalized approaches that leverage the power of lifestyle modification, recognizing its potent, non-invasive capacity to reverse the metabolic damage of type 2 diabetes and improve overall systemic health, while reserving surgical interventions for carefully selected cases where other approaches have proven insufficient or when the risks of obesity pose an immediate and severe threat. The ongoing dialogue and research in this field are crucial for ensuring that patients receive the most effective, safe, and evidence-based care for this widespread metabolic disorder.
Doctor’s Note:
This article is part of a series exploring the multifaceted aspects of bariatric surgery. Previous installments include "The Mortality Rate of Bariatric Weight-Loss Surgery" and "The Complications of Bariatric Weight-Loss Surgery." For those interested in sustainable weight loss strategies, the book How Not to Diet offers comprehensive guidance. Proceeds from the author’s books are donated to charity.






