The landscape of weight-loss surgery, while offering significant potential benefits for individuals struggling with severe obesity, is increasingly revealing a critical factor influencing patient outcomes: surgeon proficiency. Emerging research and clinical observations highlight that the very effectiveness and safety of bariatric procedures, such as sleeve gastrectomy and Roux-en-Y gastric bypass, can be profoundly impacted by the experience and technical skill of the operating surgeon. This complexity is underscored by the fact that revisions to correct complications from previous bariatric surgeries have become the third most common procedure in this field.
The Rising Tide of Revisions and Reoperations
The necessity for follow-up surgeries following initial bariatric interventions is a growing concern within the medical community. Data indicates that a substantial proportion of patients, up to 25%, may require a return to the operating room to address issues arising from their primary bariatric procedure. These reoperations carry a significantly elevated risk profile, with mortality rates potentially ten times higher than primary surgeries. Furthermore, there is no inherent guarantee of success for these subsequent interventions, leaving patients in a precarious position.
The spectrum of complications that necessitate revisional surgery is broad and can include:
- Leaks: Inadequate healing at surgical connections can lead to leakage of digestive contents into the abdominal cavity, a potentially life-threatening condition.
- Fistulas: Abnormal connections can form between organs or between an organ and the skin, leading to persistent drainage and infection.
- Ulcers: These can develop at surgical sites, causing pain, bleeding, and obstruction.
- Strictures: Narrowing of the surgically altered digestive tract can impede the passage of food, leading to nausea, vomiting, and malnutrition.
- Erosions: Material from surgical staples or implants can erode into surrounding tissues.
- Obstructions: Blockages in the digestive pathway can occur due to scarring, inflammation, or internal hernias.
- Severe Acid Reflux: While sometimes improved, bariatric surgery can also exacerbate or induce severe gastroesophageal reflux disease in some individuals.
Surgeon Skill: A Critical Determinant of Risk
A landmark study published in The New England Journal of Medicine shed significant light on the direct correlation between surgeon competency and patient outcomes. In this research, bariatric surgeons voluntarily submitted videos of their surgical procedures for evaluation by a panel of their peers. The findings revealed a wide disparity in technical proficiency among these surgeons. This variation in skill was directly linked to differing rates of patient complications, hospital readmissions, the need for reoperations, and even mortality. Patients who underwent surgery with less proficient surgeons experienced nearly three times the rate of complications and a five-fold increase in their risk of death compared to those treated by highly skilled practitioners.

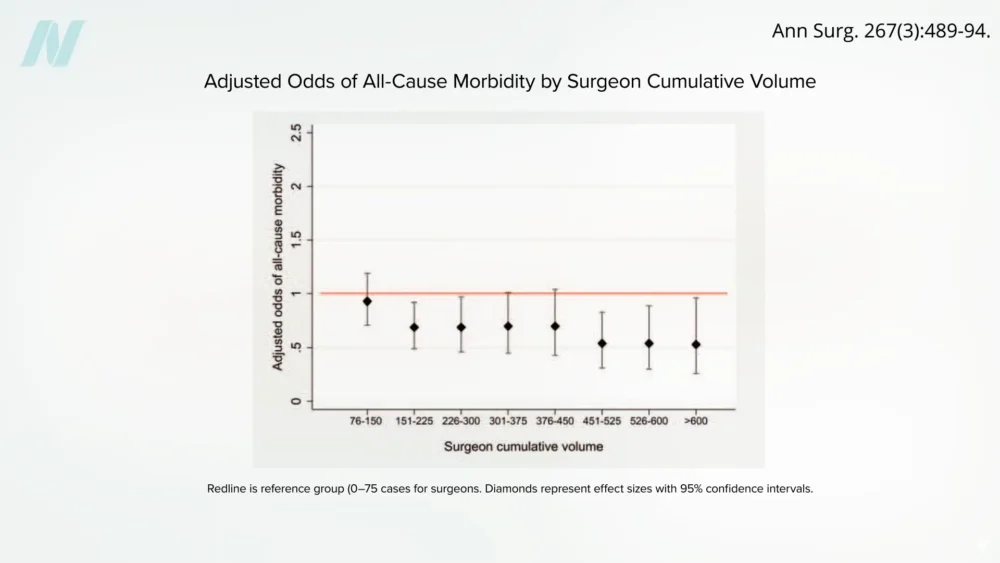
This phenomenon can be analogized to other fields requiring high levels of dexterity and judgment, such as music or athletics. While innate talent may play a role, rigorous training and extensive practice are essential for achieving mastery. In the context of bariatric surgery, the learning curve for complex procedures like gastric bypass is steep. It is estimated that a surgeon may need to perform as many as 500 cases to achieve a level of proficiency where complication rates begin to plateau. Surgeons who have performed over 600 bypass procedures generally demonstrate the lowest rates of adverse outcomes.
The statistical implications are stark. Data suggests that the odds of a fatal outcome can be more than double for patients operated on by surgeons with fewer than 75 prior cases compared to those who have performed more than 450. This underscores the critical importance of patient due diligence when selecting a surgeon.
Navigating the Decision: Patient Empowerment and Institutional Support
Given these findings, prospective patients are strongly advised to inquire about their surgeon’s experience. Key questions to consider include the total number of bariatric procedures performed by the surgeon and their specific experience with the chosen surgical technique. Beyond individual surgeon credentials, choosing an accredited bariatric "Center of Excellence" is also a critical step. These designated centers adhere to stringent quality standards and have demonstrated lower surgical mortality rates, often two to three times lower than non-accredited institutions. This focus on institutional standards can provide an additional layer of safety and quality assurance for patients.
While surgeon skill is paramount, it is important to acknowledge that patient behavior can also contribute to post-operative complications. A cautionary anecdote from a surgeon’s report, titled "The Dangers of Broccoli," illustrates this point. In this case, a woman, three months post-gastric bypass, consumed large, unchewed portions of healthy foods, including broccoli and lima beans, at an all-you-can-eat buffet. This led to a rupture of her surgical staples and required emergency surgery. While highlighting the importance of mindful eating and proper chewing post-surgery, the incident also serves as a broader reminder that the long-term success of bariatric surgery is intertwined with sustained lifestyle changes, including dietary modifications, even before the procedure itself.
Lifelong Nutritional Vigilance: An Unavoidable Consequence
Even in cases where the surgical procedure itself is executed flawlessly, bariatric surgery fundamentally alters the digestive system, necessitating lifelong nutritional replacement and vigilant monitoring. The procedures, particularly those involving malabsorption like gastric bypass, are designed to impair calorie absorption by bypassing or removing segments of the intestines. This intentional malabsorption comes at the cost of reduced absorption of essential vitamins and minerals.
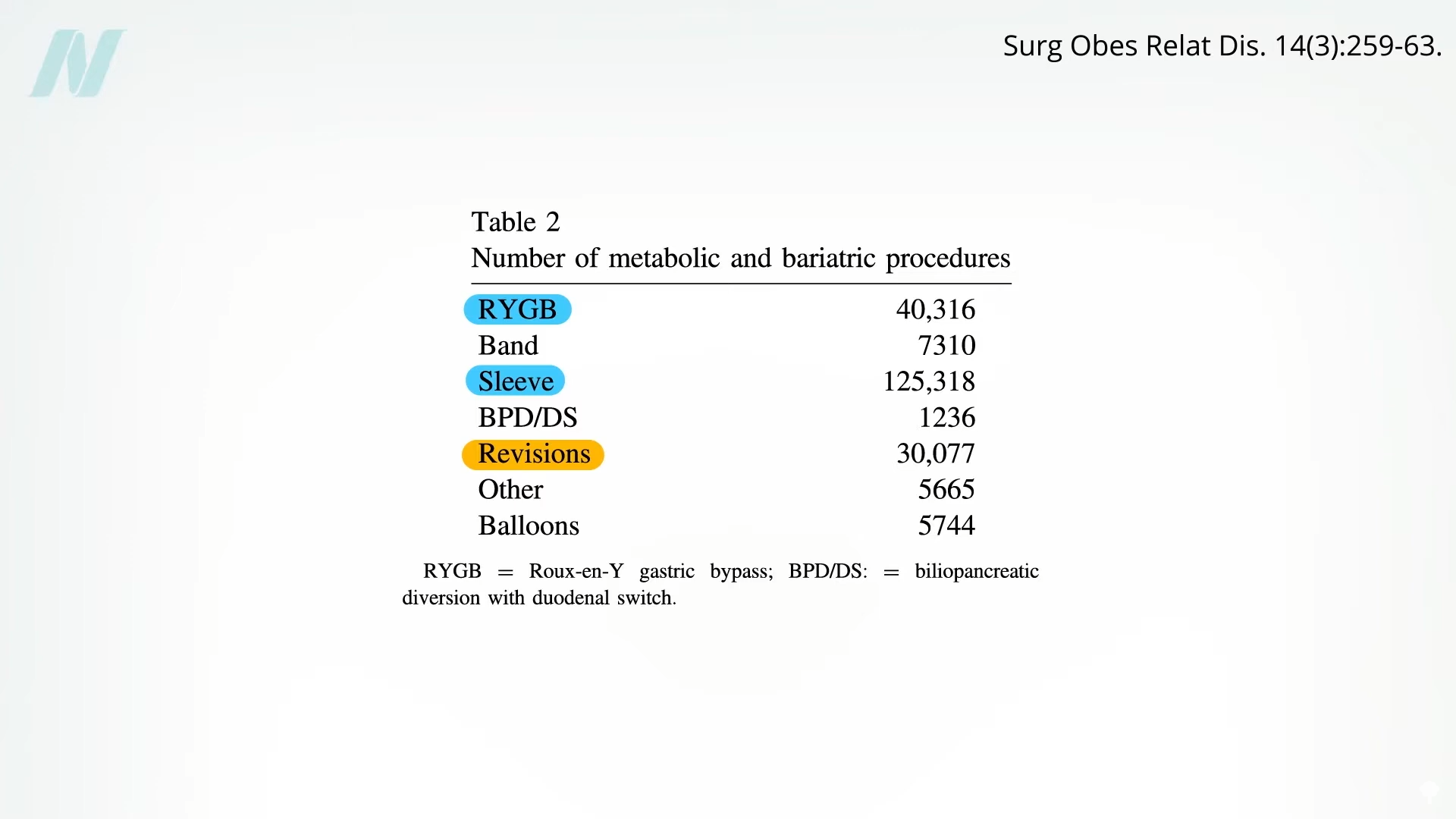

The consequences of these deficiencies can extend far beyond common issues like anemia, osteoporosis, or hair loss. Patients are at risk for severe, life-threatening deficiencies, including:
- Beriberi: Caused by thiamine (vitamin B1) deficiency, leading to neurological and cardiovascular problems.
- Pellagra: Resulting from niacin (vitamin B3) deficiency, characterized by dermatitis, diarrhea, and dementia.
- Kwashiorkor: A severe form of protein-energy malnutrition.
- Nerve Damage: Deficiencies in various vitamins and minerals can lead to neurological impairment. For instance, copper deficiency, even years or decades after surgery, can manifest as vision loss.
- Thiamine Deficiency: Tragically, severe thiamine deficiency has been reported to progress to permanent brain damage in nearly one in three patients before diagnosis.
Even restrictive procedures like stomach stapling can place patients at risk for nutrient deficiencies, often due to persistent vomiting. This vomiting, reported by up to 60% of patients post-bariatric surgery, is frequently attributed to "inappropriate eating behaviors," essentially an inability to adapt to the altered capacity and function of the stomach. The vomiting, while aiding weight loss, can be likened to the mechanism of certain medications designed to deter unhealthy behaviors through aversive physical responses.
The Role of Dumping Syndrome in Behavior Modification
Another significant post-operative phenomenon, "dumping syndrome," further contributes to the behavioral modification aspect of bariatric surgery. A substantial percentage of gastric bypass patients experience symptoms such as abdominal pain, diarrhea, nausea, bloating, fatigue, or palpitations after consuming calorie-dense foods. This occurs because food bypasses the stomach too quickly and empties directly into the intestines. Surgeons often describe dumping syndrome not as a complication, but as an intended feature of the surgery. The unpleasant physiological response serves as a powerful deterrent, discouraging patients from consuming high-energy foods and thereby supporting long-term weight management.
Broader Implications and Future Directions
The evolving understanding of bariatric surgery’s risks and benefits points towards a future where patient selection, surgeon training, and post-operative care are even more rigorously scrutinized. The data on surgeon experience is a critical piece of information that empowers patients to make more informed decisions. The emphasis on Centers of Excellence highlights the importance of institutional commitment to high standards of care.
As research continues, the focus is shifting not only to surgical technique but also to the long-term metabolic and nutritional consequences of these procedures. The ongoing series of reports, including this one, aims to provide a comprehensive overview of bariatric surgery, examining its mortality rates, its effectiveness in reversing conditions like diabetes, and the sustainability of weight loss achieved through these interventions. This detailed exploration is crucial for guiding individuals and healthcare providers in navigating the complex terrain of weight-loss surgery. The ultimate goal is to maximize the benefits while meticulously mitigating the inherent risks, ensuring that patients embarking on this journey have the most comprehensive understanding and support possible.






