In a significant neuroscientific breakthrough, researchers at Tulane University have precisely identified the specific brain circuits responsible for dictating our reactions to danger and, crucially, how these responses evolve and diminish as perceived threats recede. This groundbreaking study challenges long-held assumptions about fear, shifting the focus from a simple "on-off" switch to a sophisticated control mechanism within the central amygdala, offering unprecedented insights into conditions like post-traumatic stress disorder (PTSD).
For decades, the scientific community’s understanding of fear responses largely revolved around the concept of "freezing" – an involuntary immobility often observed in animals and humans facing immediate peril. While undeniably a critical defensive strategy, this singular focus provided only a partial picture of the complex repertoire of behaviors organisms employ when confronted with danger. The new research, spearheaded by neuroscientist Jonathan Fadok at the Tulane Brain Institute, expands this understanding dramatically, revealing that the central amygdala acts as a nuanced command center, actively selecting between passive freezing and a range of dynamic, active escape behaviors such as "darting" or "jumping." This discovery suggests that the brain doesn’t just register fear; it actively orchestrates a spectrum of defensive actions tailored to the perceived threat level.
Furthermore, the study sheds new light on the process of fear extinction – the gradual unlearning of a fear response. Contrary to the intuitive belief that overcoming fear involves "erasing" a traumatic memory, the Tulane team discovered that extinction is a process of neural recalibration. Instead of deleting the fear memory, the brain effectively reassigns control to different neural circuits, gradually shifting from high-intensity defensive responses to more regulated, lower-intensity states. This "nuanced view" of fear regulation provides a biological framework for understanding why PTSD manifests with such diverse symptoms, ranging from chronic hypervigilance and anxiety to acute panic attacks, varying significantly from one individual to another.
A Deeper Dive into the Brain’s Fear Architecture
The central amygdala, a small almond-shaped structure deep within the temporal lobe, has long been recognized as a crucial hub for processing emotions, particularly fear and anxiety. However, the precise mechanisms by which it orchestrates a diverse array of defensive behaviors remained largely elusive. Fadok and his team sought to unravel this complexity by studying the intricate interplay of distinct neuronal populations within this vital brain region.
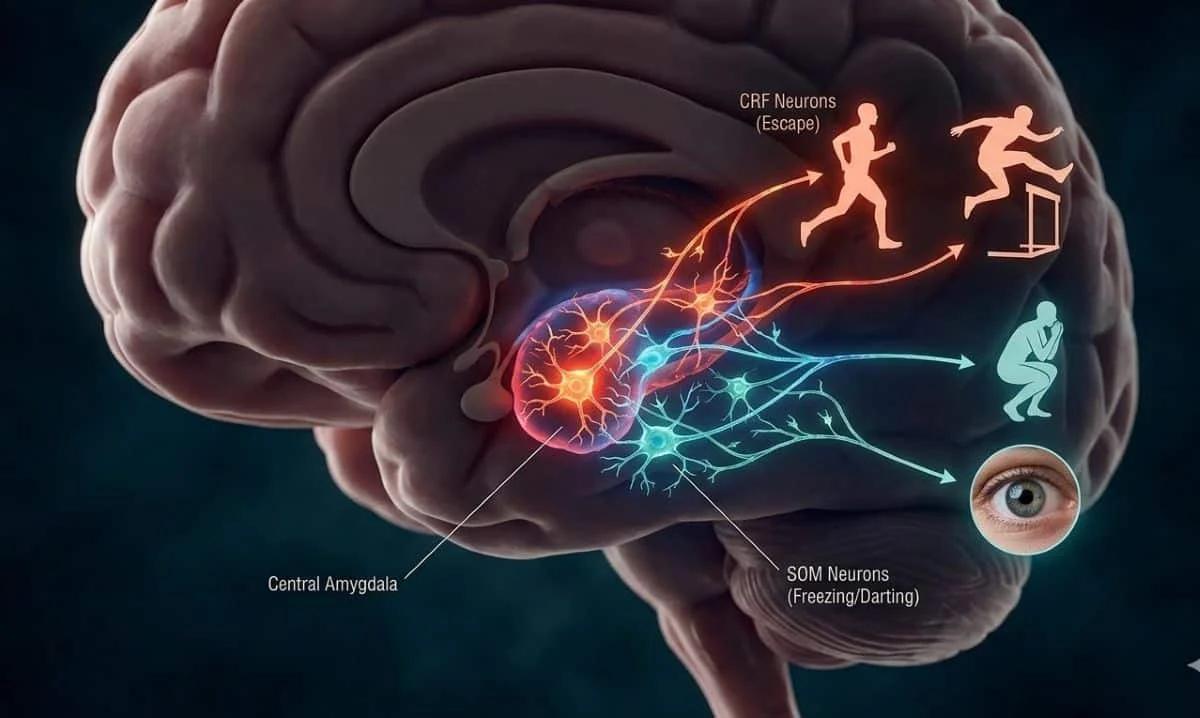
Their investigation focused on two specific types of neurons: corticotropin-releasing factor (CRF) neurons and somatostatin (SOM) neurons. Through meticulous experimentation using a modified conditioning paradigm in mice, the researchers were able to observe a broad spectrum of defensive behaviors within a single experimental setting, moving beyond the traditional focus on freezing. This innovative approach allowed them to track how these behaviors dynamically shifted during the process of fear extinction.
The findings were striking. They revealed that activity in CRF neurons primarily supported higher-intensity, active escape-like responses, such as sudden jumping or rapid darting away from a perceived threat. In stark contrast, SOM neurons were found to promote freezing behavior and played a critical role in regulating lower-intensity defensive states. This suggests a sophisticated neural "dial" within the central amygdala, where the relative activity of these two neuronal populations dictates the precise nature and intensity of the defensive response.
To further validate their observations, the researchers experimentally manipulated these circuits. Inhibiting the activity of CRF neurons significantly reduced the mice’s propensity for escape jumping, suggesting a direct causal link between CRF activity and high-intensity flight behaviors. Conversely, activating SOM neurons caused a noticeable shift in behavior, pushing the animals away from active flight and towards a more passive freezing response. These manipulations provided compelling evidence that the central amygdala is not merely a generator of a generic fear signal, but an active decision-maker in selecting the most appropriate defensive strategy.
The Evolution of Fear Research: From Simple Reflexes to Complex Circuits
The understanding of fear has undergone a significant evolution in neuroscience. Early theories, such as Walter Cannon’s "fight-or-flight" response proposed in the 1920s, laid the groundwork by identifying the physiological arousal associated with perceived danger. Cannon’s work highlighted the role of the sympathetic nervous system in preparing the body for immediate action. Later, researchers like Joseph LeDoux meticulously mapped the neural pathways involved in fear conditioning, solidifying the amygdala’s role as a central processor of fear memories.
However, much of this foundational research, particularly in animal models, relied heavily on observing "freezing" as the primary measure of fear. This was largely due to its ease of quantification and its clear evolutionary significance as a predator evasion tactic. While invaluable, this focus inadvertently narrowed the scope of understanding, potentially overlooking the rich diversity of other defensive behaviors that animals, and by extension humans, employ. The Tulane study represents a significant paradigm shift by explicitly incorporating and differentiating these active escape behaviors, thereby providing a more comprehensive model of fear processing. It acknowledges that fear is not a monolithic response but a dynamic continuum, adaptable to the immediate context and the perceived imminence and intensity of the threat.
The concept of fear extinction has also seen its share of reinterpretation. Initially, it was often conceptualized as the simple "unlearning" or "erasure" of a previously conditioned fear. However, subsequent research, including this latest study, has increasingly supported the idea that extinction is not about forgetting but about new learning – specifically, learning to inhibit or override the original fear response. This "new learning" model suggests that the original fear memory persists but is suppressed by newly formed safety memories. The Tulane findings further refine this by pinpointing the specific neural circuits involved in this recalibration, suggesting that it’s a shift in circuit dominance rather than a mere suppression of a single memory trace.
Implications for Post-Traumatic Stress Disorder and Mental Health
The implications of this research for understanding and treating psychiatric conditions, particularly PTSD, are profound. PTSD affects millions worldwide, with estimates suggesting that approximately 6% of adults in the U.S. will experience PTSD at some point in their lives, a figure that is significantly higher among veterans and individuals exposed to trauma. The disorder is characterized by persistent and debilitating fear responses that fail to diminish even when the original threat is no longer present.
One of the enduring challenges in PTSD research and treatment has been the wide variability in symptom presentation. As Fadok notes, "PTSD is often described as a disorder of persistent fear, but that persistence can look very different from person to person." Some individuals exhibit chronic hypervigilance, an elevated state of alertness, constantly scanning their environment for potential threats. Others experience more acute, panic-like reactions, including intense bursts of anxiety, rapid heart rate, and an overwhelming urge to flee, even in safe environments. The Tulane study provides a compelling biological explanation for this variability. If different neural circuits within the central amygdala preferentially drive different defensive behaviors (e.g., CRF for active escape, SOM for freezing), then disruptions or dysregulations in these specific circuits could account for the diverse manifestations of PTSD.
Current treatments for PTSD, such as exposure therapy and pharmacotherapy (e.g., SSRIs), aim to facilitate fear extinction. Exposure therapy, for instance, involves gradually exposing individuals to trauma-related stimuli in a safe environment to help them learn that these stimuli are no longer dangerous. While effective for many, these treatments are not universally successful, and a significant portion of individuals continue to suffer from persistent symptoms. The new findings offer a potential avenue for refining these therapies. If extinction involves shifting responses away from high-intensity states mediated by specific neurons, then interventions that can precisely target and modulate these circuits could enhance the efficacy of existing treatments or lead to entirely new therapeutic approaches.
Future Directions and Therapeutic Potential
While the research does not immediately translate into new treatments, it clearly identifies specific biological pathways that could serve as targets for future therapeutic interventions. The ability to selectively manipulate CRF and SOM neurons in animal models opens the door to developing highly specific drugs or neuromodulation techniques that could help "nudge" the brain out of a persistent high-intensity fear state and back into a more regulated, manageable one.
For instance, future pharmacotherapies might focus on compounds that selectively inhibit CRF neuron activity to reduce extreme panic or flight responses, or enhance SOM neuron activity to promote a more regulated, less reactive state. Similarly, advanced neuromodulation techniques, such as targeted deep brain stimulation or optogenetics (a technique using light to control neurons, currently experimental in humans), could theoretically be employed to rebalance the activity of these specific circuits.
Moreover, the study underscores the importance of a personalized medicine approach to mental health. If an individual’s PTSD symptoms are predominantly characterized by active escape behaviors, therapies might be tailored to specifically modulate the CRF-driven circuits. Conversely, if freezing and hypervigilance are more pronounced, interventions targeting SOM neurons could be prioritized. This level of specificity could dramatically improve treatment outcomes by addressing the unique neural underpinnings of each patient’s condition.
The collaborative nature of such research, supported by institutions like the National Institutes of Health and the U.S. Department of Veterans Affairs, highlights the critical national commitment to understanding and alleviating the burden of conditions like PTSD, especially for those who have served. This funding is essential for pushing the boundaries of neuroscience and translating fundamental discoveries into clinical applications.
The Central Amygdala: A Decision-Maker, Not Just a Generator
Perhaps one of the most significant conceptual shifts offered by this research is the refined understanding of the central amygdala’s role. As Fadok aptly summarizes, "It’s not just generating fear. It’s helping decide what that fear looks like." This statement encapsulates the idea that the amygdala is far more than a simple alarm bell. It is a sophisticated neural processor capable of evaluating threats, integrating contextual cues, and orchestrating a nuanced, adaptive array of defensive behaviors. This active "decision-making" capacity highlights the brain’s remarkable plasticity and its ability to finely tune responses to an ever-changing environment.
Understanding this intricate biological switchboard for fear responses has broader implications beyond PTSD. It could shed light on other anxiety disorders, phobias, and even the general mechanisms of stress response. By dissecting the precise neural architecture governing our most primal reactions to danger, scientists are paving the way for a new era of targeted therapies, offering hope for millions who struggle to regulate their fear in a world that, at times, can feel overwhelmingly threatening. The journey from a simple "fight or flight" concept to the intricate dance of CRF and SOM neurons within the central amygdala marks a profound leap in our quest to comprehend the human mind and its capacity for both vulnerability and resilience.








